

Featured
Rimsys Announces Rimsys AI to Eliminate Repetitive Tasks and Enhance Decision-Making for MedTech Regulatory Teams
Rimsys, the leading Regulatory Information Management (RIM) platform for the MedTech industry, today announced the launch of Rimsys AI, a suite of embedded artificial intelligence (AI) agents.

Post-market surveillance for medical devices in the European Union
This article is an excerpt from Post-market surveillance for medical device in the European Union.
Table of Contents
- What is post-market surveillance?
- What classes of medical devices require post-market surveillance?
- Components of a successful post-market surveillance plan
- PMS data requirements
- Post-market surveillance system goals
- Required post-market surveillance reporting
- Embracing post-market surveillance as an integral part of your quality program
- Getting started with post-market surveillance
Post-market surveillance (PMS) is designed to monitor the performance of a marketed medical device by collecting and analyzing field use data. Article 10 of the EU MDR and IVDR requires all device manufacturers to have a post-market surveillance system in place. The main elements of the PMS are laid out in Article 83, and additional details for lower-risk and higher-risk devices are covered in articles 84 and85, respectively.
In general, a PMS system consists of both proactive activities and reactive, or vigilance, activities. While post-market surveillance and vigilance are sometimes used interchangeably, vigilance consists of separate activities that feed post-market surveillance programs.
Post-market surveillance systems are used to collect and analyze data not only about the manufacturer’s device but also about related competitors’ devices that are on the market. Data collected through PMS procedures is then used to identify trends that may lead to, among other things, quality improvements, updates to user training and instructions for use, and identification of manufacturing issues.
Note that “market surveillance” encompasses activities performed by a Competent Authority to verify MDR compliance, and should not be confused with the topic of this ebook,“post-market surveillance," which is performed by the manufacturer.
All medical devices marketed in the EU require some level of post-market surveillance, and all medical device manufacturers must implement a post-market surveillance system (PMS). The requirements of the PMS, however, vary and should be “proportionate to the risk class and appropriate for the type of device” (MDR Chapter VII). In particular, the type and frequency of reporting vary based on a device’s risk class.
A post-market surveillance plan (PMS) is an integral part of a manufacturer’s quality management system and provides a system for compiling and analyzing data that is relevant to product quality, performance, and safety throughout the entire lifetime of a device. The PMS should also provide methods for determining the need for and implementing any preventative and corrective actions. A PMS system should include and define:
Surveillance data sources
With the increased focus on proactive risk identification in the MDR, it is important to design post-market surveillance systems that actively acquire knowledge and detect potential risks. It is not sufficient to rely solely on spontaneous reporting by healthcare providers, patients, and other stakeholders.
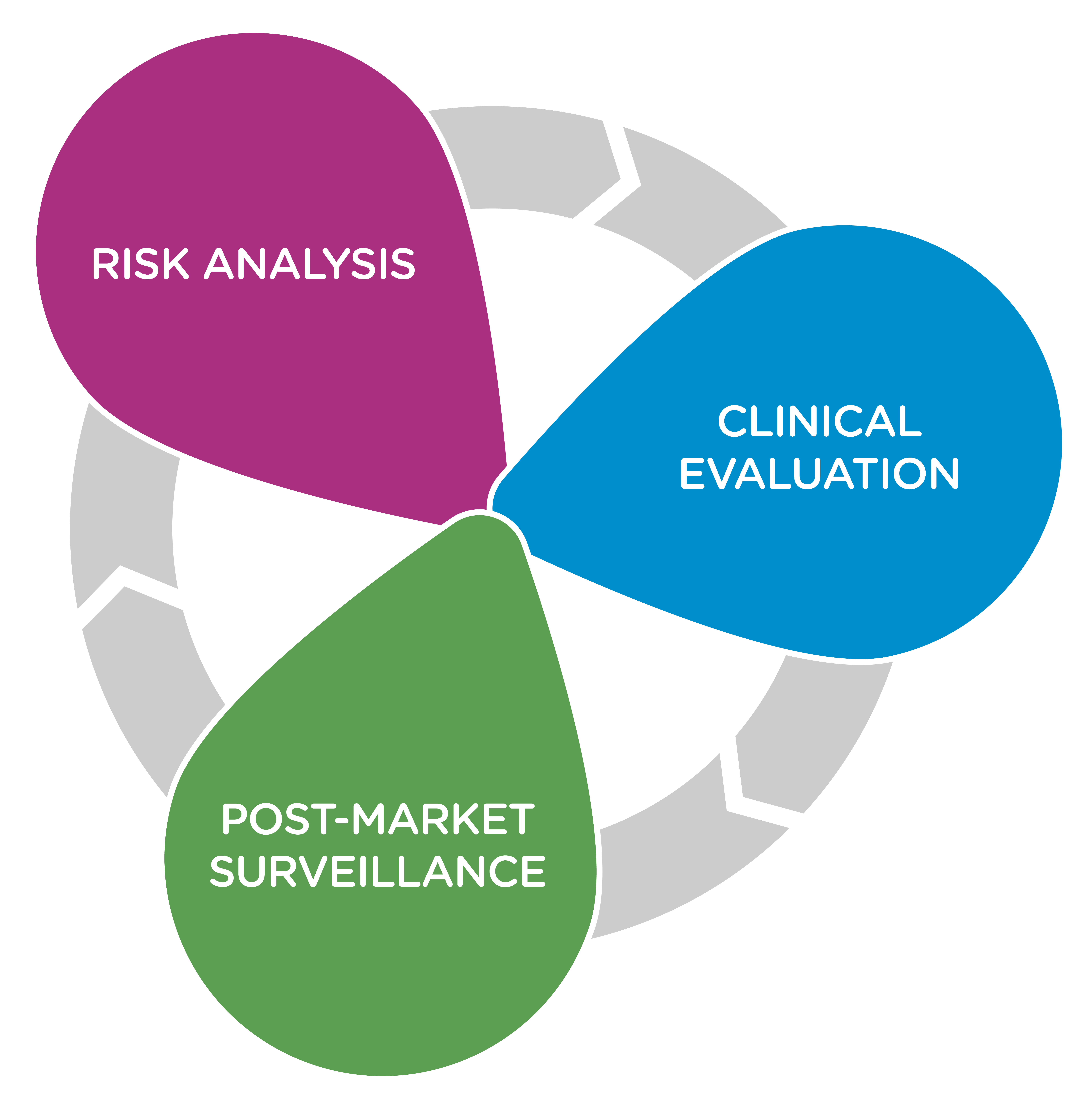
In addition to information coming from Clinical Evaluation Reports and complaint and adverse event reporting, typical sources of surveillance data include:
• Social media networks: Because many of your stakeholders may be communicating on social media networks, it is important to employ social listening techniques and/or tools to identify issues and concerning trends as they develop.
• Industry and academic literature: Any studies, academic papers, and other literature that addresses similar devices or the specific use cases for which your device is designed should be evaluated. In particular, risk factors and adverse events identified with similar devices should be closely examined. It is also important to identify newer technologies that may affect the benefit-risk ratio and establish a new definition of “state of the art” for the device type.
• EUDAMED: While the European Database on Medical Devices (EUDAMED) is not yet fully functional, it is intended to provide a living picture of the lifecycle of all medical devices marketed in the EU. Manufacturers should take special care to consider information for similar devices made available through the EUDAMED system in the future.
• Registries: Patient, disease, and device registries can provide information that informs the clinical evaluation process which provides input into the post-market surveillance system.
Data analysis methodology
A well-defined data analysis methodology will accurately identify trends and lead to defendable decisions in the application of post-market experience. Once the necessary information has been identified and collected, and potentially cleaned of incomplete or otherwise unusable data, the data needs to be analyzed.
The goal is to identify meaningful trends, correlations, variations, and patterns that can lead to improvements in the safety and efficacy of the device. There are many data analysis tools available that can assist with:
• Regression analysis that will identify correlations between data (e.g. the device location/geography correlates to battery life).
• Data visualization that can be useful in spotting trends in the data.
• Predictive analytics, which can be particularly useful with large data sets, to identify future trends based on historical data.
• Data mining, which is also normally used with large datasets, to organize data and identify data groups for further analysis.
Benefit-risk indicators and thresholds
The MDR requires that medical device manufacturers not only demonstrate the clinical benefit of their device but also quantify the benefit-risk ratio. The benefit of a device must be shown to clearly outweigh the risk for it to gain market approval. Article 2 (24) of the MDR defines the benefit-risk determination as “the analysis of all assessments of benefit and risk of possible relevance for the use of the device for the intended purpose when used in accordance with the intended purpose given by the manufacturer.”
A PMS system should clearly define benefit-risk calculations and the data used to support them. Post-market surveillance activities are critical in order to re-evaluate and maintain the benefit-risk calculations and determinations of a device throughout its life. Information that is gained through a PMS system can lead to:
• Identification of new risk factors.
• Adjustments to risk frequency and/or severity values based on actual use data.
• Adjustments to established risk calculations based on new “state of the art” technologies becoming available.
• Adjustments to established benefit calculations based on actual use data.
While complaint handling and other feedback tracking are more often described as part of post-market vigilance systems, they play a role in the more proactive post-market surveillance processes as well. A PMS system should define ...
To continue reading this ebook, download the full version.

An overview of 21 CFR Part 820 - quality systems for medical device manufacturers
What is 21 CFR Part 820?
21 CFR 820 is the FDA federal regulation that pertains to quality systems for medical device manufacturers, and it is part of the agency’s set of Current Good Manufacturing Practices (CGMP) for industry. Also referred to as the FDA’s quality system regulation (QSR), the regulation defines design controls and quality processes at all stages of device development in order to ensure that all medical devices marketed in the United States are safe and effective.
21 CFR 820 consists of 15 subparts, which define quality system requirements for each stage and function within the medical device manufacturing process. We define each subpart below.
Federal regulations are organized as Title → Chapter → Subchapter → Part, which means that 21 CFR 820 is short-hand for:

21 CFR 820 vs ISO 13485
ISO 13485 is the de facto international quality system standard for medical device manufacturers, but this is not currently the standard in the United States. While Part 820 and ISO 13485 are structured differently, they have no conflicting requirements. Therefore, companies that are marketing medical devices in the U.S. and in other markets will need to comply with both ISO 13485 and the FDA’s QSR, as defined in 21 CFR 820.
However, the FDA is moving towards harmonizing these standards, and on February 23, 2022 issued a proposed rule to amend the QSR to align more closely with the international consensus standard for Quality Management Systems, primarily by incorporating reference to the ISO 13485 standard. The FDA has published FAQ’s about the proposed rule.
21 CFR Part 820 Requirements
Part 820: General Controls (subpart A)
The General Controls subpart contains three sections providing general information about the regulation, including the scope and applicability along with key definitions.
Scope
The regulation defines current good manufacturing practice (CGMP) requirements governing the methods, facilities, and controls used for the “design, manufacture, packaging, labeling, storage, installation, and servicing of all finished devices intended for human use." Specifically, this subpart defines:
- Applicability:
The requirements of this regulation are intended to ensure the safety and efficacy of all finished medical devices intended for human use that are manufactured in or imported into the United States. Manufacturers that are involved in some, but not all, manufacturing operations should comply with those requirements that are applicable to the functions they are performing.
Exceptions:
- This regulation does not apply to manufacturers of medical device components, but such manufacturers are encouraged to use this regulation as guidance.
- Class I medical devices are exempt from the Design Controls defined in this regulation, except for those listed in § 820.30(a)(2).
- Manufacturers of blood and blood components are not subject to this regulation but are subject to Biologics good manufacturing practices as defined in Subchapter F, Part 606 of the regulation.
Definitions
This section of the regulation contains definitions for a number of terms used throughout the document. The following are the major definitions related to quality records:
- Design history file (DHF): A compilation of records that describes the design history of a finished device.
- Design input: The physical and performance requirements of a device that are used as a basis for device design.
- Design output: The results of a design effort at each design phase and at the end of the total design effort. The finished design output is the basis for the device master record. The total finished design output consists of the device, its packaging and labeling, and the device master record.
- Device history record (DHR): A compilation of records containing the production history of a finished device.
- Device master record (DMR): A compilation of records containing the procedures and specifications for a finished device.
Quality System
The section of the regulation sets the basic requirement for a quality system by stating that “Each manufacturer shall establish and maintain a quality system that is appropriate for the specific medical device(s) designed or manufactured, and that meets the requirements of this part.”
The term “appropriate” is used throughout this regulation and can be open to interpretation. A manufacturer, however, should assume that all requirements are appropriate and applicable except in cases where non-implementation of the requirement can be shown to have no effect on the product's specified requirements or ability to carry out necessary corrective actions.
Quality system requirements (subpart B)
This section of the regulation defines the overall responsibilities and the resources required for the management of the quality system.
Management responsibilities
Executive management is responsible for establishing a quality policy and ensuring adequate resources to effectively maintain and manage the quality system. In addition, management is responsible for establishing a specific quality plan, consisting of relevant practices, resources, activities, and procedures.
Quality audit
Periodic audits of the quality system are required to be conducted by personnel not directly responsible for the activities being audited. The dates and results of each audit need to be documented, along with the results of the audit. It is expected that corrective actions and, when necessary, reaudits, be performed for any identified noncompliances.
Personnel
Manufacturers are responsible for assigning sufficient personnel with appropriate experience and training to perform all tasks required by the quality system plan.
Design controls (subpart C)
Manufacturers of all class II and class III medical devices, along with the specific class I devices listed in paragraph (a)(2) of this regulation, are required to establish design control procedures that ensure design requirements are met as specified.
Design controls shall define:
- Design and development planning - Plans that describe the design and development activities, and responsibilities for these activities and their implementation.
- Design input - Procedures that ensure design requirements are appropriate and address the intended use of the device.
- Design output - Procedures that document design output, including acceptance criteria, so that conformance to design input requirements can be adequately evaluated.
- Design review - Formal and documented reviews of the ensign results that include participation from representatives of all.
- Design verification - Procedures for verifying the device design that confirm that the design output meets the design input requirements.
- Design validation - Procedures for validating the device design, ensuring that devices conform to defined user needs and intended uses, and including testing of production units under actual or simulated conditions.
- Design transfer - Procedures to ensure that the device design is correctly translated into production specification.
- Design changes - Procedures for identifying, documenting, validating, and managing the verification and approval process of all design changes before they are implemented.
- Design history file - A design history file (DHF) is required for each type of device and should include or reference the records necessary to demonstrate that the design was developed in accordance with the approved design plan and device requirements.
Document controls (subpart D)
Medical device manufacturers are required to put in place document controls for all documents required in this regulation.
Document approval and distribution
One or more people must be assigned to review and approve documents prior to issuance. The approval must be documented, include a date and the signature of the approver, and be made available at all locations where applicable. Procedures must also be in place to ensure that obsolete documents are removed and/or prevented from being used.
Document changes
Similar to document approval procedures, changes to documents must be approved, reviewed, and documented. Records of all changes must be maintained.
Purchasing controls (subpart E)
To continue reading this Regulatory Brief, including a definition of the remaining subparts and a comparison of 21 CFR 820 to ISO 13485, please download the full brief.

A primer on medical device classification
While it may seem simple, medical device classification can be a challenging task for many medical device and IVD manufacturers. Device classes for specific regions and countries have a number of small variations, and each of those variations can impact the process by which a device obtains market clearance. Getting it wrong can lead to delays in getting to market. This article explores the classification systems for three major markets, and their associated regulations.
An important component of achieving regulatory approval is the appropriate classification of a medical device or in vitro diagnostic device, according to the specific regulations within a country or region. Product classifications are related to the intended use of the product and the perceived risk that it poses to a patient using the device. While this general approach is pretty standard across all regions, there are many small variations in different country classification systems that can impact how a device is regulated. It would be much easier if there was one global classification system that everyone followed.
However, since there are different guidelines to classifying a medical device (per country), we’ll dig into the most popular classification systems—Canada, the European Union and the United States. These three are globally perceived to have strong, thorough, and trusted quality and regulatory systems. Their approaches are often mirrored or used as proxies for market clearance in other countries.
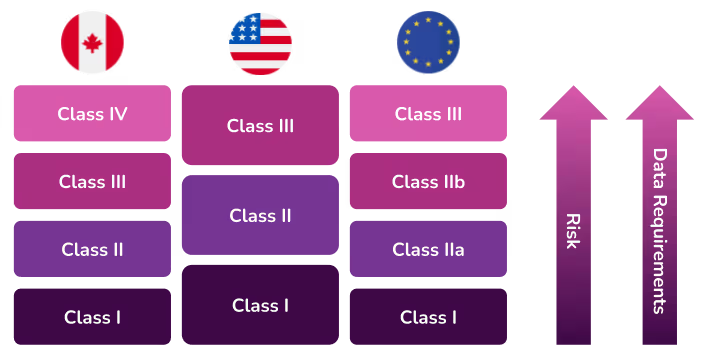
Canada
The Canadian Medical Devices Regulations include guidelines that classify devices into four risk classes. If a medical device can be classified into more than one class, the class representing the higher risk always applies.
- Class I devices do not require a medical device licence to be sold in Canada, but manufacturers, distributors and importers of these devices are required to obtain an establishment licence.
- Class II requires a medical device licence
- Class III requires a medical device licence
- Class IV requires a medical device licence
Some examples of different classes of devices in Canada include:
European Union
One of the main changes introduced with the new MDR/IVDR regulations are new classification rules for medical devices and in vitro diagnostic devices. If you have gone through the process of getting your medical device in the European market before, you might find it more difficult with the new EU MDR rules. For example, a new medical device you want to bring to market might now fall into a higher classification than it would have previously (under the MDD), and therefore require more testing, updates to documents, quality approvals, etc.
The new EU MDR brings the classification of medical devices in Europe more in line with international regulations, specifically the United States. These updated rules are listed in MDR 2017/745 for devices and IVDR 2017/746 for in vitro diagnostic products. As with Canada, if a medical device can be classified into more than one class, the class representing the higher risk always applies.
The EU has recently released a new guidance document MCDG 2021-24 to assist device manufacturers with device classification questions.
Class I – this classification is for the lowest risk device. Most medical devices in this category do not require a conformity assessment from a Notified Body so instead, they can be self-assessed. However, manufacturers must still complete a Technical File as part of the approval process.According to MDCG 2019-15, there are three subclasses under Class I. Unlike most Class I devices, these will require the involvement of a Notified Body.
- Class Im: a product with a measuring function
- Class Is: a product that is sterile
- Class Ir: a product that is a reusable, surgical instrument
Class IIa – this classification is for a medium risk device. A conformity assessment by a Notified Body is required for this classification.
Class IIb – this classification is for medium-to-high risk devices. A conformity assessment by a Notified Body is required for this classification.
Class III – this classification is for the highest risk devices. A conformity assessment by a Notified Body is required for this classification.
Examples of different classes of devices in the European Union include:
In Vitro Diagnostic Devices:
Class A – this classification is for the lowest risk in vitro diagnostic devices. Most IVD devices in this category do not require a conformity assessment. Instead, they can be self-assessed.
Class B – this classification is for medium risk in vitro diagnostic devices. A conformity assessment by a Notified Body is required for this classification.
Class C – this classification is for medium-to-high risk in vitro diagnostic devices. A conformity assessment by a Notified Body is required for this classification.
Class D – this classification is for the highest risk in vitro diagnostic devices. A conformity assessment by a Notified Body is required for this classification.
Examples of the different in vitro diagnostic device classes in the European Union include:
United States
In the United States, the Food and Drug Administration (FDA) is responsible for overseeing the safety of medical devices. The FDA has established classifications for approximately 1,700 different types of devices and grouped them into 16 medical specialties referred to as panels. All three classes of devices are subject to General Controls which are the baseline requirements of the Food, Drug and Cosmetic (FD&C) Act.
- Class I – General Controls (with or without exemptions)
- Class II – General Controls and Special Controls (with or without exemptions)
- Class III – General Controls, Special Controls and Premarket Approval
You are permitted to classify your own medical device based upon the FDA guidance documents and set regulations. However, if you wish for the FDA to assist with establishing your classification you can submit a 513(g) Request for Information. Note that there is a user fee associated with a 513(g) Request.
The device class determines which type of premarketing submission/application is required for market clearance.
In some instances, you do have the opportunity to reclassify your product after it’s been released to the market. The regulatory class of a device type, as defined by the Federal Food, Drug and Cosmetic Act (FD&C Act), may be changed through petition to the FDA. This process is only applied to a device type though, not to an individual device.
Examples of medical device classification in the US include:
Getting classification correct
Medical device classification is simple in that each country and region generally follows the same classification approach, and complex in that minor differences can change how a device is classified across markets. Understanding how a device is classified is one of the critical first steps regulatory affairs teams need to take when entering a new market, as medical device class often determines the pathway to market.
For example, in the EU classification can mean the difference between self-certification and a required conformity assessment from a Notified Body. In the US, classification can mean the difference between a 510(k) or PMA process for market clearance. Getting classification correct can ensure a smoother and faster route to market.
To learn more about market clearance processes for medical devices in the US, check out the Beginner’s Guide to the 510(k).

MDSAP - the ultimate guide to the medical device single audit program
This article is an excerpt from The ultimate guide to the medical device single audit program (MDSAP) ebook.
Table of contents
- What is MDSAP?
- History of MDSAP
- Who is responsible for the MDSAP?
- How does an MDSAP audit work?
- Audit sequence
- You got a nonconformity – now what?
- What does an MDSAP audit cost?
- Why choose the MDSAP certification process?
- Potential disadvantages of the MDSAP
- Ready to participate? – Here’s how to get started
- Completing a successful MDSAP audit
The Medical Device Single Audit Program (MDSAP) was designed and developed to allow a single audit of a medical device manufacturer to be applied to all country markets whose regulatory authorities are members of the program. The MDSAP provides efficient and thorough coverage of the standard requirements for medical device manufacturer quality management systems, and requirements for regulatory purposes (ISO 13485:2016). In addition, there are specific requirements of each medical device regulatory authority participating in the MDSAP that must be met:
- Conformity Assessment Procedures of the Australian Therapeutic Goods (Medical Devices) Regulations (TG(MD)R Sch3)
- Brazilian Good Manufacturing Practices (RDC ANVISA 16)
- Medical Device Regulations of Health Canada (ISO 13485:2003)
- Japan Ordinance on Standards for Manufacturing Control and Quality Control of Medical Devices and In Vitro Diagnostic Reagents (MHLW Ministerial Ordinance No 169)
- Quality System Regulation (21 CFR Part 820), and specific requirements of medical device regulatory authorities participating in the MDSAP program.
This means that a report from a single MDSAP audit of a medical device manufacturer would be accepted as a substitute for routine inspections by all the member Regulatory Authorities (RAs) across the world. There are currently five participating Regulatory Authorities (RA) representing the following countries: Australia, Brazil, Canada, Japan and the USA.

In April, 2021, the RAs released an “Audit Approach” document (MDSAP AU P0002.006) that combines the formerly separate MDSAP Audit Model and Process Companion documents into a single guidance document. It includes guidance for assessing the conformity of each process and includes an audit sequence, instructions for auditing each specific process, and identifies links that highlight the interactions between the processes.
In March 2012 the US FDA announced that they had approved a final pilot guidance document “Guidance for Industry, Third Parties and Food and Drug Administration Staff: Medical Device ISO 13485:2003 Voluntary Audit Report Submission Pilot Program.” This allowed the owner or operator of a medical device manufacturing facility to be removed from FDA’s routine inspection work plan for 1 year upon completing a ISO 13485:2003 audit. This guidance document went into effect in June 2012, and was intended as an interim measure while a single audit program was being developed.
This pilot program was not very successful and few companies signed up because they did not see any advantage in participating. The manufacturer had to pay for a third party to inspect their facilities, generate a report, and share the inspection results back to the FDA. Many companies were reluctant to contract “someone else” to perform their inspection when they could easily wait for the FDA to conduct an inspection for free.
During its inaugural meeting in Singapore in 2012, the International Medical Device Regulators Forum (IMDRF) appointed a working group to develop a set of documents for a harmonized third-party auditor system. Hence, the “Medical Device Single Audit Program” (MDSAP) was formed. The concept was similar to the FDA’s original idea of creating a third-party auditor to help reduce their workload of performing regulatory audits of medical device manufacturers’ quality management systems. This new approach would consist of a single audit that would review regulatory QMS compliance, conducted by a third-party, who would later be called an Auditing Organization (AO).
From January 2014 to December 2016, five countries participated in a Medical Device Single Audit Program Pilot. In June 2017, a report was generated summarizing the outcomes of prospective “proof- of-concept” criteria established to confirm the success of the program. The outcomes are documented in the final MDSAP Pilot Report and recommended that the program become fully active and open to any manufacturer who requested this type of audit.
The governing body of the MDSAP is the Regulatory Authority Council (RAC), which is composed of two senior managers (and a few other staff members) from each participating RA. They are responsible for executive planning, strategic priorities, setting policy, and making decisions on behalf of the MDSAP International Consortium. The RAC also reviews and approves documents, procedures, work instructions, and more. The mission of the MDSAP International Consortium is to jointly leverage regulatory resources to manage an efficient, effective, and sustainable single audit program focused on the oversight of medical device manufacturers on a global scale.
Other international partners that are involved in the MDSAP include:
MDSAP Observers:
- European Union (EU)
- United Kingdom’s Medicines and Healthcare products Regulatory Agency (MHRA)
- The World Health Organization (WHO) Prequalification of In Vitro Diagnostics (IVDs) Program
MDSAP Affiliate Members:
- Argentina’s National Administration of Drugs, Foods and Medical Devices (ANMAT)
- Republic of Korea’s Ministry of Food and Drug Safety
- Singapore’s Health Sciences Authority (HSA)
The observers and affiliate members are not the same as the participating member RA’s. The observers simply observe and/or contribute to RAC activities. Affiliate members, on the other hand, are interested in engaging in the MDSAP program and are subject to certain rules. They are only given access to a certain level of information about the manufacturers, audit dates, and information in audit reports.
They are also invited to attend sessions that are open to members, observers, and affiliates only.
Audits can also be conducted by MDSAP participating RAs at any time and for various reasons including:
- "For Cause" due to information obtained by the regulatory authority
- as a follow up to findings from a previous audit
- to confirm the effective implementation of the MDSAP requirements
The purpose of audits conducted by the RAs is to ensure appropriate oversight of the AOs MDSAP auditing activities. The AOs are appointed by the RAs and a list of the currently approved AO’s is published on the FDA website. Most AOs offer a broad range of management system certification services, beyond just medical devices. Manufacturers should verify that prospective AOs are clearly trained and perform MDSAP audits of medical devices.
AOs have the final word as to whether a manufacturer has met the requirements for the MDSAP during the execution of the audit and generation of the associated reports summarizing the results. MSDAP RAC participating RAs have the final decision regarding all development, implementation, maintenance, and expansion activities associated with the program.
Although an unannounced visit by an AO is rare, it can happen in circumstances where high-grade nonconformities have been detected.
To continue reading this eBook including a detailed look at the MDSAP audit process and grading, pros and cons of the approach, and how to get started please register to download the full version.

Rimsys joins MedTech Europe
This week Rimsys became an associate member of MedTech Europe, the European trade association representing the medtech industry, alongside some of the world’s largest medical technology companies. As a member of the organization, we’ll have visibility into regulatory changes across the region as they’re being formed, and the opportunity to shape how those regulations are implemented. This access will help us to ensure that the digitization and automation of regulatory processes remains in reach for all medtech companies, and that our software will be best positioned to help them.
What is MedTech Europe?
MedTech Europe is a trade association focused on making innovative medical technology available to more people, and making healthcare systems more sustainable. Members of the organization include medical technology companies—device and in vitro diagnostic manufacturers, industry service and technology providers, and country-level associations within the European region.
The organization serves as a trusted resource of medical technology information for the public, providing data and highlighting the value of new technologies, and for policy-makers and other key stakeholders. It publishes industry research and statistics, contributes to health-related policy and legislation, and works to expand patient and provider access to new, lifesaving technologies.
Why did we join?
At Rimsys, we’re passionate about the medical technology industry, and focused on providing technology solutions to help medtech companies strengthen regulatory compliance, and bring new products to market more quickly. The European region is a focal point for medical technology regulation, and the MDR/IVDR regulations that began to take effect this year will inform the approaches of health authorities around the world.
Regulatory digitization and automation happens both at the manufacturer level and the health authority level. MDR/IVDR brings unique device identification (UDI) requirements, and a centralized technology system for product and post market surveillance information (EUDAMED) to the market. Both of these elements are digital by nature, and can serve as end-points of automated processes run within the Rimsys Platform.
Earlier this year, we introduced a new approach to UDI, one that ties together market requirements, product information, registrations, and selling status in an integrated regulatory lifecycle. Rather than managing UDI data separately from other regulatory information and activities, companies can auto-populate compliant UDI information directly, and will soon be able to submit that information electronically to the EUDAMED database. As a MedTech Europe member, we can participate in working groups around these systems, and ensure that we have the insights and access that we need to develop and deliver features like this for our customers.
How does this benefit our customers?
For Rimsys customers, this is all about maximizing the value they can get from our holistic Regulatory Information Management (RIM) platform. Our platform is designed to support a wide range of regulatory processes, and many of these processes are shaped by the regulations themselves. As members of MedTech Europe, we’ll be involved in policy discussions as they happen, and can ensure that the updates we make and features that we add are in alignment with the latest regulations. Understanding how regional policy is evolving also allows us to share that intelligence in-product—alerting customers to relevant changes, and updating market entrance requirements.
The second key benefit is access. The automation of regulatory processes is most effective when it can be done end to end. This therefore includes interactions with health authorities. Government agencies, including the European Commission, are establishing digital channels for product registration, UDI, and clinical and post market surveillance data. Our goal at Rimsys is to provide as many direct integrations with these systems as possible. As MedTech Europe members, we’ll be part of the groups that advise policy-makers, and help to develop these systems. As a result, we can help to ensure that our integrations are as functional and effective as possible.
Learn more about automation and digitization for regulatory affairs
Whether you distribute medical products in the European Union or in other markets, there can be significant benefits associated with digitizing and automating regulatory processes including better information access, more cross-company collaboration, less manual administrative work, and faster time to market for new products. To learn some more, see the Top 6 Benefits of a RIM system, or contact us to request a custom demo.

FDA 510(k) - a beginner's guide
This article is an excerpt from The beginner's guide to the 510(k) ebook.
Table of Contents
- Introduction
- 510(k) basics
- Contents of a Traditional 510(k)
- 510(k) submission and timelines
- Other 510(k) forms
Congratulations! You have successfully developed a new medical device. Now you need to take it to market. In the United States, this often means submitting a 510(k). A 510(k) is a structured package of information about your device and its performance and safety that you submit to the Food and Drug Administration (FDA) for “clearance” before you can sell your device in the U.S. In order to receive clearance from the FDA, your 510(k) will need to demonstrate that your medical device is substantially equivalent to another legally marketed device (called a predicate device). The substantial equivalence approval process is a simple equation that looks something like this:

The 510(k) is generally the most efficient route to market clearance in the U.S. because you show your device is safe and effective based on this substantial equivalence standard, instead of needing to present more extensive clinical trial data.
There are three types of 510(k): Traditional, Abbreviated, and Special. This eBook will begin with a general overview of the 510(k) process, including its purpose and benefits. Next, we will explore the Traditional 510(k) and the sections and components required in depth. Finally, we will look at the Special and Abbreviated 510(k).
FDA: background and device oversight
Before we explain what a 510(k) is let’s first talk generally about the FDA and device oversight. The FDA is the U.S. governmental agency responsible for overseeing medical devices, drugs, food, and tobacco products. When it comes to medical devices, the FDA’s mission is to “protect the public health by ensuring the safety, efficacy, and security of…medical devices.” At the same time, the FDA also has an interest in “advancing public health by helping to speed innovations.” In other words, the FDA’s goal is to make sure devices are safe and effective for public use, while also ensuring that devices have a quick and efficient path to market.
In order to achieve this balance of safety and efficiency, the FDA has three different levels of oversight depending on the risk level of the device: (1) exempt from premarket submission, (2) Premarket Notification, also known as 510(k), and (3) Premarket Approval (PMA).
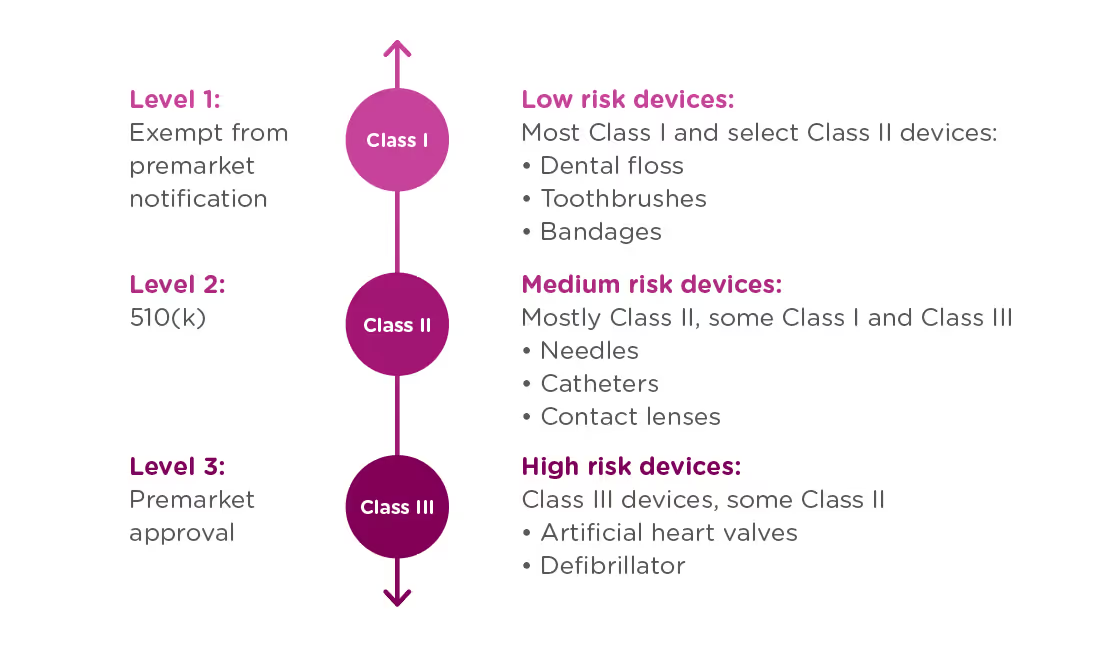
When is a 510(k) required?
A 510(k) is required for medium risk devices that have a predicate on the market which can be used to demonstrate the safety and effectiveness of the new device. Meanwhile, a PMA is required for high-risk or novel devices which require a higher level of scrutiny to be confirmed safe and effective.
A 510(k) is not only required for new devices, but also for devices that have been modified in a way that could impact safety or effectiveness. This could include changes to the:
- Design
- Components
- Materials
- Chemical composition
- Energy source
- Manufacturing process
- Intended use
You must submit your 510(k) at least 90 days before marketing the device.
What Exactly is Substantial Equivalence?
Now that we know what a 510(k) is, let’s talk about the substantial equivalence standard. You’ll recall from the introduction that your 510(k) must show that the new (or modified) device is substantially equivalent to at least one other legally marketed device, called a predicate device. Substantial equivalence looks at the intended use and the technological characteristics of the two devices.
More specifically, you must show:
- that the new device has the same intended use as the predicate, and
- the differences between the two devices do not raise questions about the safety and effectiveness of the new device.
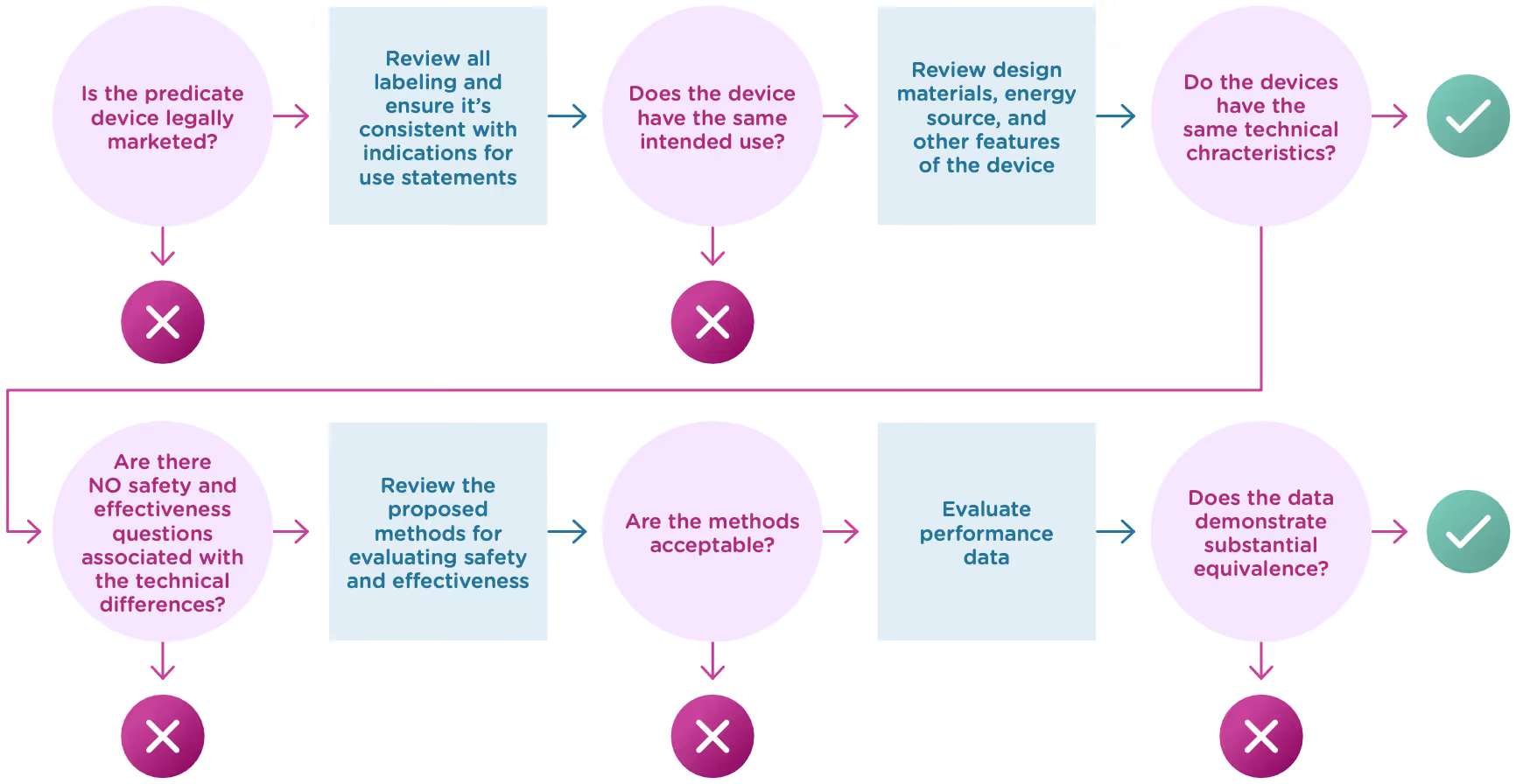
Now let’s take a closer look at intended use and technological characteristics.
Intended use
Intended use means the general purpose or function of the device. The FDA will look at your proposed labelling and your Indications of Use section of the 510(k) to determine the intended use of your device (this is covered in Chapter 2). Intended use includes:
Technological characteristics
Once the FDA has determined that a predicate device exists and that the new device and the predicate device have the same intended use, it will move on to compare the technological characteristics. Technological characteristics include:
- Materials
- Design
- Energy source
- Other device features
The two devices do not have to be identical, and in fact they almost never are. The key here is to demonstrate that any differences do not have a significant impact on safety or effectiveness. Here’s what to cover when you compare your device’s technological characteristics with that of the predicate device:
Overall description of the device design
- Engineering drawings or diagrams to explain the device and component parts.
- List of component parts and explanation of how each component contributes to the overall use and function of the device.
- Physical specifications: dimensions, weight, temperature, tolerances, etc.
Materials
- Detailed chemical formulation used in all materials of constructions (especially those that come into contact with a patient).
- Any additives, coatings, paint, or surface modifications.
- How materials have been processed and what state they’re in.
Energy Sources
- Use of batteries, electricity, etc.
Other technological features
- Software/hardware
- Features
- Density
- Porosity
- Degradation characteristics
- Nature of reagents
- Principle of the assay method
In deciding whether the differences in technological characteristics impact safety or effectiveness, the FDA will typically rely on descriptive information about the technological characteristics as well as non-clinical and clinical performance data.
Let’s look at an example: A manufacturer submits a 510(k) for a new type of contact lens. Both the new device and the predicate device are indicated for daily wear for the treatment of astigmatism. The predicate device is only available in a clear lens, but the new device comes in a line of colors, including purple tinted lenses.

Who is responsible for submitting a 510(k)?
The following four types of organizations may be responsible for submitting a 510(k):
Manufacturers
- End-of-line device manufacturers who will be placing a device on the U.S. market.
- Note: Does not apply to component part manufacturers unless components will be marketed independently.
Specification developers
- Companies that develop the specifications for a finished device which has been manufactured elsewhere
Repackers or relabelers
- Required to submit a 510(k) if they significantly alter the labeling or condition of the device, including modification of manuals, changing the intended use, deleting or adding warnings, contraindications, sterilization status.
- Note: This is rare. The manufacturer, not the repackager or labeler, is typically responsible for the 510(k) submission.
Importers
- Importers that introduce a new device to the U.S. market may need to submit a 510(k), if it hasn’t already been submitted by the manufacturer.
Now that we’ve covered the basics, let’s explore what actually goes into your 510(k).
A Traditional 510(k) should contain all the following components in the list below. In some cases, a particular section may not apply to your device. When that happens, it’s a good idea to include the section anyway and just state “This section does not apply” or “N/A” under that heading.
To continue reading this eBook including a detailed walk-through of all the Traditional 510(k) components, submission requirements and timelines, and an overview of the other 510(k) forms including the Abbreviated 510(k) and the Special 510(k), please register to download the full version

EUDAMED and UDI in Europe: an overview
What is EUDAMED?
The European Databank on Medical Devices (EUDAMED) is an IT system developed by the European Commission to increase transparency and improve surveillance of medical devices (and in vitro diagnostics) that are sold within the European Union. It serves a key functional role in the unique device identification (UDI) requirements included in the MDR and IVDR regulations.
This article excerpts from The Ultimate Guide to the EU/IVDR UDI ebook to highlight the specific role and associated requirements that the EUDAMED database plays in the new regulations.
Element 4: The UDI database
The fourth component of the UDI system is entry of UDI and device information into the UDI database through EUDAMED. The MDR and IVDR require manufacturers to register all devices and submit specific information to the database before placing a device on the market. The core data elements provided through the UDI database will be accessible to the public free of charge. The list below outlines all of the required information for device registration.
Annex VI, Part A of 2017/745, states that the UDI database will contain all information about devices presently on the market and discontinued products. The database is designed to allow for linking across all packaging levels of the device. For all devices currently on the market, manufacturers are required to periodically verify the accuracy of the information in the database. If any changes are made to a device that do not require a new UDI-DI, manufacturers must still update the database within 30 days.
Information to be submitted with the device and economic operator registration must include
- Economic operator information (2017/745 Annex VI, Part A(1)):
- Information relating to the device
- Manufacturing information
The tables below outline all of the specific information that must be submitted to EUDAMED:
In addition to this information, the European Commission recently released the UDI HelpDesk. The HelpDesk will provide support to economic operators in the implementation of the obligations and requirements introduced by the new UDI system.
To learn more about EUDAMED and the European UDI system including a UDI overview, formats and issuing entities, implementation timelines, and key differences between the EU and US UDI systems, please register to download the full ebook.

Tackling regulatory continuity: How regulatory affairs teams can use technology to reduce the impact of employee turnover
Regulatory affairs is without a doubt a challenging function for all life sciences companies. In a recent survey of industry executives, 72% of them reported that regulatory affairs is one of their top 3 challenges. The pain is even more acute in the medical technology space. In the past few years medical device and in vitro diagnostic companies have had to contend with a host of new, more complex regulations for the European market (the new EU MDR/IVDR regime), as well as nascent medical device regulations in new markets around the world.
A significant additional challenge that medtech companies have to manage is that of continuity. Perhaps due to the challenges of the job, turnover among regulatory affairs (RA) professionals is surprisingly high. According to data from Zippia, RA professionals at all levels average less than 3 years in their jobs. This is echoed by the RAPS Global Compensation and Scope of Practice Report which showed that 63% of RA professionals have more than 7 years of regulatory experience, but 60% have been in their current jobs 3 years or less.
The limitations of outsourcing
One of the most common ways that medtech companies attempt to address continuity challenges is by employing external consultants. Consulting firms provide needed expertise, and especially bandwidth to resource-constrained RA teams. A recent survey by Grand View Research found that large medtech companies regularly outsource 50% or more of their regulatory activities.
Consultants are undoubtedly helpful, but the general approach to consulting engagements makes them less than ideal for a broad set of regulatory activities. Consulting engagements are inherently project-based. They generally have a specific scope, and a set of associated deliverables. However, medtech regulatory affairs is inherently product-based. Activities revolve around the product’s lifecycle—from market introduction to maintenance to withdrawal. A consulting firm may help to complete market applications for a new device in Latvia, Japan, and Brazil, but the company still needs to maintain a full post market surveillance regime, track standards in associated essential principles tables, and keep UDI information up to date as packaging permutations change.
At some point there’s a transition from the consultants back to the internal RA team, and the same continuity problem re-asserts itself. How to capture and disseminate the information, applications, and country certificates associated with a consulting project so that the internal team can move forward while maintaining compliance and market clearance?
"Poor-fit" tooling creates information silos
The lack of technology solutions designed specifically for medtech regulatory affairs is another driver of continuity issues. Regulatory activities necessitate the organization and management of large amounts of information. Detailed product specifications, performance and safety data, regulatory requirements, and relevant standards are just a few of the key pieces of information associated with each individual product and countries in which it’s sold. This is why RA professionals spend a huge amount of their time (up to 50%) simply looking for information.
Typically organizations manage regulatory information using spreadsheets or other general purpose tools. These tools, used to try and help manage information continuity, can actually create information silos. This happens for two reasons. One, the information that RA teams need for their activities is often broadly dispersed across the organization. Regulatory documents may be in a document management system (or just as often on individual employees’ computers), product and quality information is stored in PLM/QMS systems, and information about countries and selling status is contained within ERP systems. Spreadsheets don’t actually integrate with these sources, they just link. As information changes or is updated, it’s incumbent on employees to make manual updates to the spreadsheet.
Which brings us to the second problem. While there have been significant improvements in collaborative editing, documents like spreadsheets aren’t designed for the level of auditing and information management that regulatory teams need. Knowing whether an individual line item showing market status to be active, or a link to testing information in the QMS systems is up to date, still becomes “tribal knowledge” known only to the individual employees that make the update. If an employee leaves the company, all of that information goes with them.
How regulatory information management systems can improve continuity
The emergence of new technologies designed specifically for regulatory affairs activities has provided some new ways that medtech companies can tackle the continuity issue. Regulatory information management (RIM) systems provide a couple key capabilities that can increase the productivity of RA team members, and ensure that their work continues uninterrupted as team members come and go.
The first advantage of a RIM system is data association and integration. Rather than simply noting information, RIM systems can actively integrate with information sources, and automatically update as information changes. All of the information can be organized around individual products—the way that feels most intuitive to RA professionals. For any given product, an RA team member can quickly find country selling status, registrations, certificates, and expiration dates.
RIM systems can also eliminate a lot of the manual administrative work associated with regulatory activities. They can help streamline registrations with digitized authoring and publishing of regulatory submissions, and the creation and maintenance of digital essential principles tables. These capabilities are wrapped in a full set of project management tools, allowing teams to create workflows, approvals, timelines, etc. that match their internal processes and organizational goals. Individual records can be automatically updated such as the auto-population of UDI data when product details change, or bulk updates of essential principles tables when a standard is updated. These capabilities increase bandwidth across the RA team, and ensure that even new members can easily operate in accordance with the company’s processes.
RIM systems function as a “single source of truth” for RA teams. Because they work with all regulatory activities, they not only store information, but cross-link it in ways that make it instantly usable. RA team members can quickly pull regulatory information about products, product families, countries, regions, individual projects, eliminating the time spent searching for information. With enterprise integration capabilities, information can be pulled and shared with PLM, QMS, and ERP systems. This ensures that information is automatically updated, and key dependencies on regulatory activities are automatically linked. For example, clearance to enter a new market could automatically trigger a change in selling status in the ERP system. Having an organized, central source of regulatory data prevents information silos from forming, and ensures that nothing is lost when RA team members move on to other roles.
Finding the right RIM solution
Medtech regulatory complexity isn’t likely to abate any time soon, but there are steps that companies can take to better manage RA team bandwidth and continuity. Traditional approaches like outsourcing, or general productivity/information tools like spreadsheets are helpful, but they have limitations that can exacerbate continuity challenges. Modernizing the regulatory affairs toolset can be a good starting point. RIM systems with the right capabilities have the potential to increase RA team productivity, and eliminate information silos.
Key RIM features include support for a broad set of regulatory activities. Some tools focus on one aspect of RA like product registrations. As a result, they’re unlikely to effectively centralize and organize a broad set of regulatory information. While helpful from a productivity perspective, they can still lead to information silos for activities that aren’t digitized within the tool. Other RIM systems are primarily designed for the pharmaceutical industry. While they appear similar, regulations, and processes for medical technologies are different across the board. Tools that aren’t designed for medtech won’t feel as intuitive for employees, and likely won’t do as good a job at automating regulatory activities.
Rimsys provides a full-featured RIM system that is designed specifically for medtech companies, and supports a full range of regulatory activities. To see if the Rimsys Platform can improve your RA continuity, request a custom demo today.





