

Featured
Rimsys Announces Rimsys AI to Eliminate Repetitive Tasks and Enhance Decision-Making for MedTech Regulatory Teams
Rimsys, the leading Regulatory Information Management (RIM) platform for the MedTech industry, today announced the launch of Rimsys AI, a suite of embedded artificial intelligence (AI) agents.

The beginner's guide to the FDA 510(k)
This article is an excerpt from The beginner's guide to the 510(k) ebook.
Table of Contents
- Introduction
- 510(k) basics
- Contents of a Traditional 510(k)
- 510(k) submission and timelines
- Other 510(k) forms
Congratulations! You have successfully developed a new medical device. Now you need to take it to market. In the United States, this often means submitting a 510(k). A 510(k) is a structured package of information about your device and its performance and safety that you submit to the Food and Drug Administration (FDA) for “clearance” before you can sell your device in the U.S. In order to receive clearance from the FDA, your 510(k) will need to demonstrate that your medical device is substantially equivalent to another legally marketed device (called a predicate device). The substantial equivalence approval process is a simple equation that looks something like this:

The 510(k) is generally the most efficient route to market clearance in the U.S. because you show your device is safe and effective based on this substantial equivalence standard, instead of needing to present more extensive clinical trial data.
There are three types of 510(k): Traditional, Abbreviated, and Special. This eBook will begin with a general overview of the 510(k) process, including its purpose and benefits. Next, we will explore the Traditional 510(k) and the sections and components required in depth. Finally, we will look at the Special and Abbreviated 510(k).
FDA: background and device oversight
Before we explain what a 510(k) is let’s first talk generally about the FDA and device oversight. The FDA is the U.S. governmental agency responsible for overseeing medical devices, drugs, food, and tobacco products. When it comes to medical devices, the FDA’s mission is to “protect the public health by ensuring the safety, efficacy, and security of…medical devices.” At the same time, the FDA also has an interest in “advancing public health by helping to speed innovations.” In other words, the FDA’s goal is to make sure devices are safe and effective for public use, while also ensuring that devices have a quick and efficient path to market.
In order to achieve this balance of safety and efficiency, the FDA has three different levels of oversight depending on the risk level of the device: (1) exempt from premarket submission, (2) Premarket Notification, also known as 510(k), and (3) Premarket Approval (PMA).
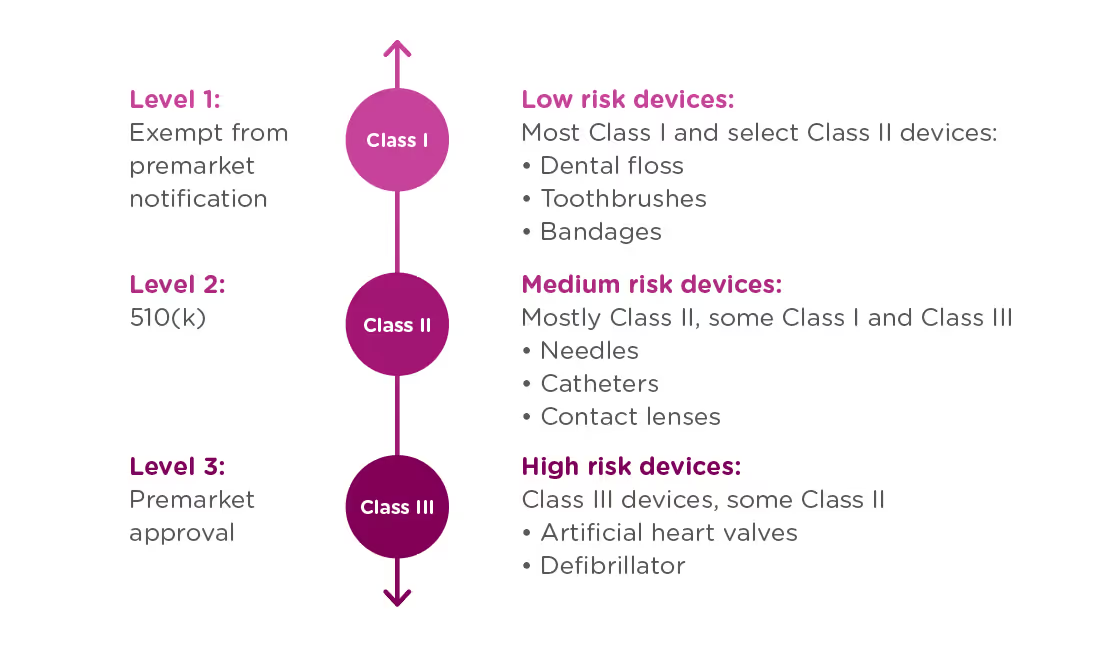
When is a 510(k) required?
A 510(k) is required for medium risk devices that have a predicate on the market which can be used to demonstrate the safety and effectiveness of the new device. Meanwhile, a PMA is required for high-risk or novel devices which require a higher level of scrutiny to be confirmed safe and effective.
A 510(k) is not only required for new devices, but also for devices that have been modified in a way that could impact safety or effectiveness. This could include changes to the:
- Design
- Components
- Materials
- Chemical composition
- Energy source
- Manufacturing process
- Intended use
You must submit your 510(k) at least 90 days before marketing the device.
What Exactly is Substantial Equivalence?
Now that we know what a 510(k) is, let’s talk about the substantial equivalence standard. You’ll recall from the introduction that your 510(k) must show that the new (or modified) device is substantially equivalent to at least one other legally marketed device, called a predicate device. Substantial equivalence looks at the intended use and the technological characteristics of the two devices.
More specifically, you must show:
- that the new device has the same intended use as the predicate, and
- the differences between the two devices do not raise questions about the safety and effectiveness of the new device.
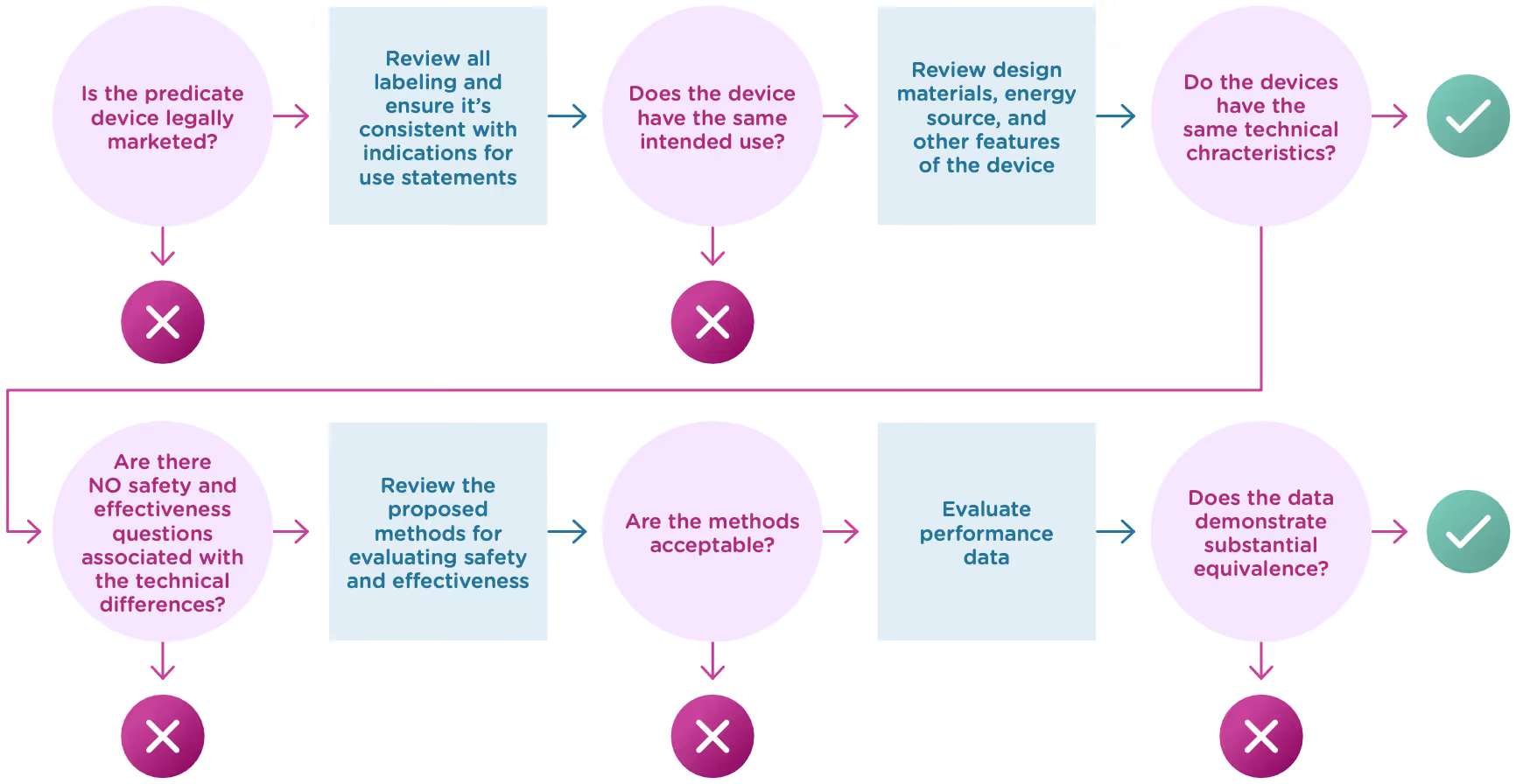
Now let’s take a closer look at intended use and technological characteristics.
Intended use
Intended use means the general purpose or function of the device. The FDA will look at your proposed labelling and your Indications of Use section of the 510(k) to determine the intended use of your device (this is covered in Chapter 2). Intended use includes:
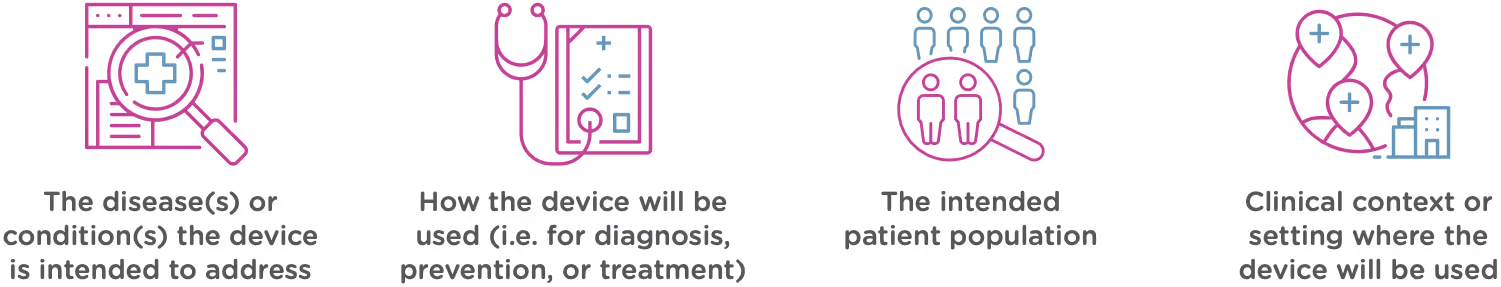
Technological characteristics
Once the FDA has determined that a predicate device exists and that the new device and the predicate device have the same intended use, it will move on to compare the technological characteristics. Technological characteristics include:
- Materials
- Design
- Energy source
- Other device features
The two devices do not have to be identical, and in fact they almost never are. The key here is to demonstrate that any differences do not have a significant impact on safety or effectiveness. Here’s what to cover when you compare your device’s technological characteristics with that of the predicate device:
Overall description of the device design
- Engineering drawings or diagrams to explain the device and component parts.
- List of component parts and explanation of how each component contributes to the overall use and function of the device.
- Physical specifications: dimensions, weight, temperature, tolerances, etc.
Materials
- Detailed chemical formulation used in all materials of constructions (especially those that come into contact with a patient).
- Any additives, coatings, paint, or surface modifications.
- How materials have been processed and what state they’re in.
Energy Sources
- Use of batteries, electricity, etc.
Other technological features
- Software/hardware
- Features
- Density
- Porosity
- Degradation characteristics
- Nature of reagents
- Principle of the assay method
In deciding whether the differences in technological characteristics impact safety or effectiveness, the FDA will typically rely on descriptive information about the technological characteristics as well as non-clinical and clinical performance data.
Let’s look at an example: A manufacturer submits a 510(k) for a new type of contact lens. Both the new device and the predicate device are indicated for daily wear for the treatment of astigmatism. The predicate device is only available in a clear lens, but the new device comes in a line of colors, including purple tinted lenses.

Who is responsible for submitting a 510(k)?
The following four types of organizations may be responsible for submitting a 510(k):
Manufacturers
- End-of-line device manufacturers who will be placing a device on the U.S. market.
- Note: Does not apply to component part manufacturers unless components will be marketed independently.
Specification developers
- Companies that develop the specifications for a finished device which has been manufactured elsewhere
Repackers or relabelers
- Required to submit a 510(k) if they significantly alter the labeling or condition of the device, including modification of manuals, changing the intended use, deleting or adding warnings, contraindications, sterilization status.
- Note: This is rare. The manufacturer, not the repackager or labeler, is typically responsible for the 510(k) submission.
Importers
- Importers that introduce a new device to the U.S. market may need to submit a 510(k), if it hasn’t already been submitted by the manufacturer.
Now that we’ve covered the basics, let’s explore what actually goes into your 510(k).
A Traditional 510(k) should contain all the following components in the list below. In some cases, a particular section may not apply to your device. When that happens, it’s a good idea to include the section anyway and just state “This section does not apply” or “N/A” under that heading.
To continue reading this eBook including a detailed walk-through of all the Traditional 510(k) components, submission requirements and timelines, and an overview of the other 510(k) forms including the Abbreviated 510(k) and the Special 510(k), please register to download the full version

The ultimate guide to the China UDI system and database
This article is an excerpt from The ultimate guide to the China NMPA UDI system and database ebook.
Table of Contents
- Overview
- UDI basics and benefits
- UDI format requirements and issuing entities
- UDI database and submission requirements
- Implementation of UDI and the UDI database in China
The current Chinese medical device regulatory regime kicked-off in 2014 with the Regulation on Supervision and Administration of Medical Devices. This core set of registration requirements, modeled after the United States and European Union systems, established a set of device classifications (class I, II, and III) based on risk and procedures for obtaining market clearance for each type of device.
Medical devices in China are regulated by the National Medical Products Administration (NMPA). Class I devices, such as clinical laboratory equipment or non-invasive skin dressings, require only notification to the NMPA for marketing authorization, and that authorization does not expire. Class II and III devices such as implantable devices or devices with a measuring function require full registration and a formal review before market clearance can be obtained.
These initial regulations have been expanded since their introduction, adding accelerated pathways to market for certain products in certain regions, easing acceptance of clinical data from overseas, and more specific roles and responsibilities for local agents of international manufacturers. In addition, in 2019, the regulations added a provision that medical devices carry a unique device identification (UDI). China’s UDI requirements are similar to those in the US and European Union. They establish specific device ID and labeling requirements, as well as a central, state-administered database of devices.
This eBook walks through the basics of medical device UDIs, the specifics of China’s implementation, and how MedTech companies who market their devices in China can prepare for the full rollout of these regulations in the coming years.
A UDI is a unique alphanumeric code that is designed to identify medical devices sold in a particular country/region from manufacturing, through distribution, to use by a patient. Like other aspects of the medical device regulatory regime, the UDI system in China follows the approach taken by the United States FDA and European Commission, and is based on the guidance from the International Medical Device Regulators Forum (IMDRF). Generally, UDI systems are designed to improve patient safety and optimize care by:
- Increasing the traceability of medical devices, including field safety corrective actions
- Providing an unambiguous identification method for medical devices throughout distribution and use
- Making adverse event reports more accessible
- Reducing medical errors by providing detailed information related to the device
- Simplifying medical device documentation and making it more consistent
There are three components to the UDI system in China:
- UDI code: The actual UDI code can be assigned by one of three (3) issuing agencies and contains information about the product, it’s expiration date, and the manufacturing batch/lot it’s associated with.
- UDI labeling: Put simply, medical devices must carry the UDI code on them. The regulations stipulate how devices and their packaging must be labeled for compliance.
- UDI database: In addition to labeling, all device UDIs must be submitted to a central database that is administered by the NMPA.
The following sections explore each of these components in more detail.
The UDI code
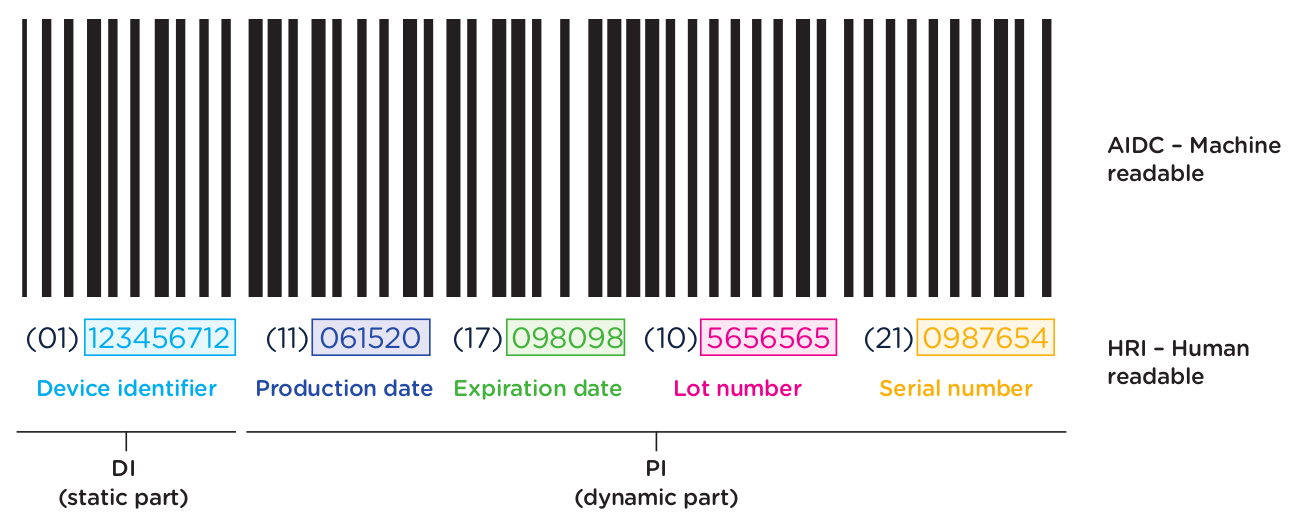
The first element of the UDI system is the code itself. The UDI code is the alphanumeric identifier that is associated with a specific medical device. UDI codes have two (2) elements to them, the UDI device identifier (UDI-DI) or static portion, and the UDI production identifier (UDI-PI) or dynamic portion. You can see the two components in the UDI diagram below:

The UDI-DI contains information about the issuing entity—the organization that is authorized to assign UDI codes. In China, this can be one of three entities: GS1, an international barcode and electronic data interchange standards organization, and two domestic organizations: the Zhongguancun Industry & Information Research Institute (ZIIOT), and AliHealth. Additional details about the issuing agencies are covered in Chapter 2. In addition, the UDI-DI contains information about the manufacturer and the specific model or version of the device.
The UDI-PI contains information about the manufacturing and production of the device. This typically includes information about the lot or batch number in which the device was manufactured, the manufacturing date and expiration date for the device (if applicable), and the specific serial number for the device. Here you can see all of the components marked up using the same UDI example:
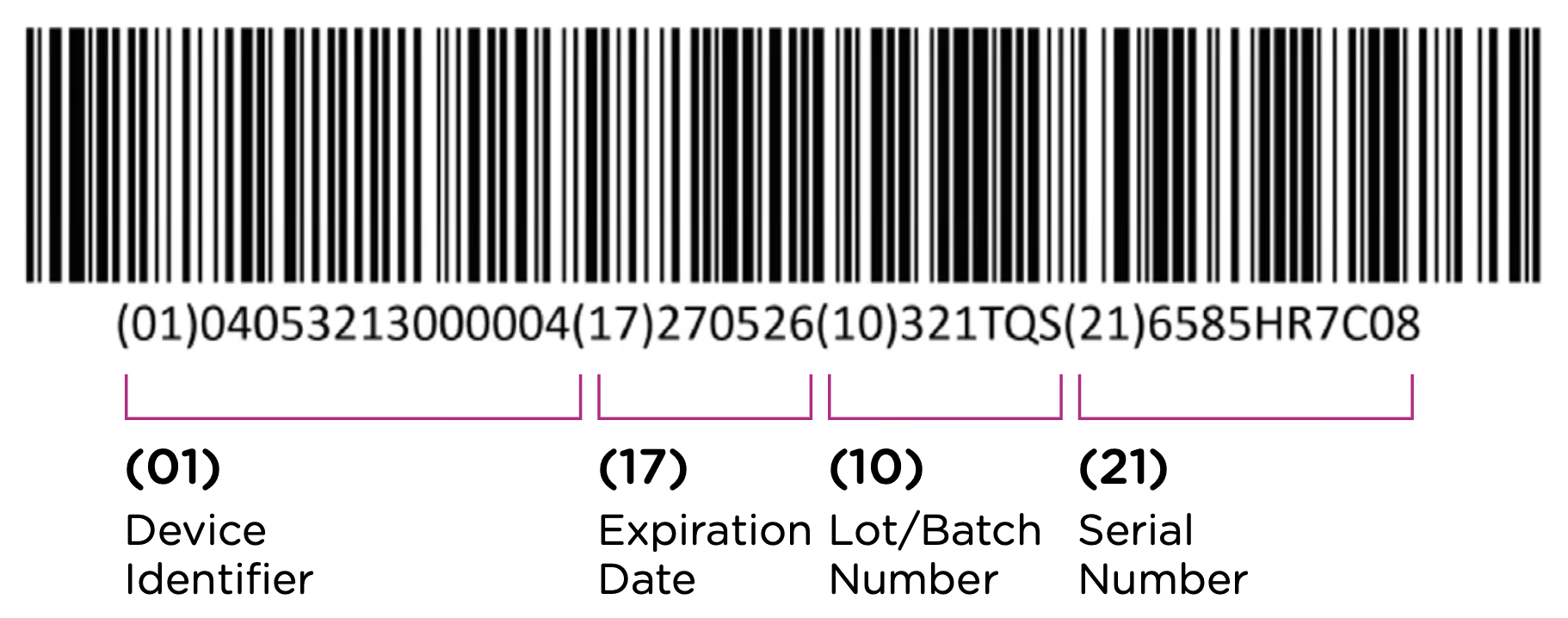
Note that each packaging permutation and level for a given device will need to be assigned its own UDI. So for example, let’s say that a company manufactures 5ml enteral (oral) syringes in two packaging options: 1 – packaged individually and 2 – packaged in a box of 5. Each packaging option would need its own UDI, despite the fact that the underlying product is the same.
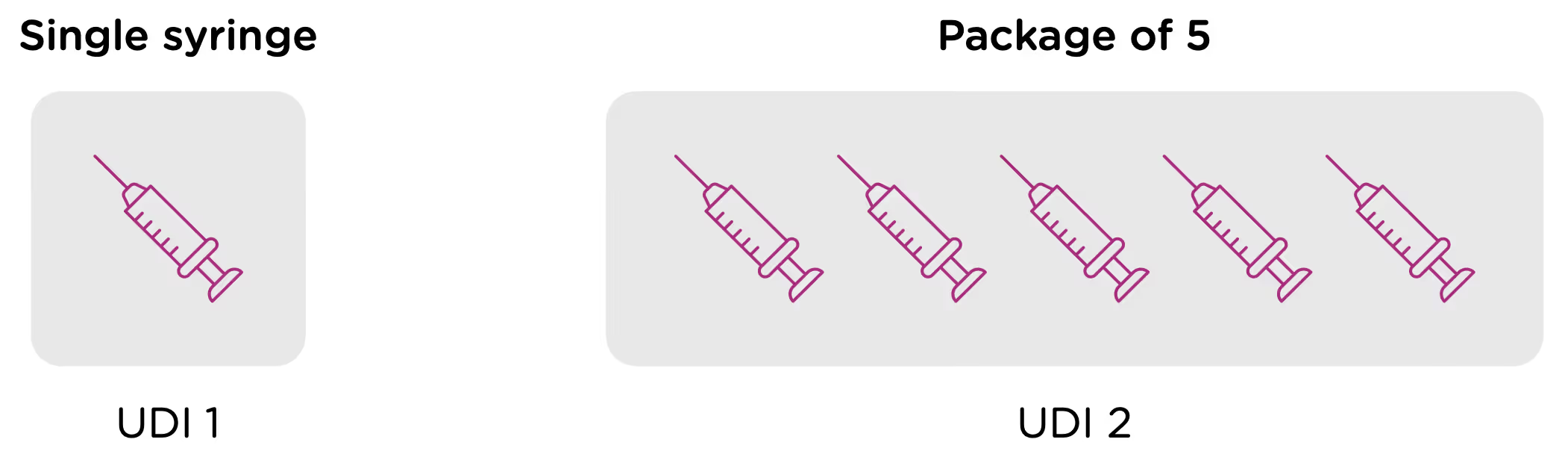
Now looking at packaging levels, let’s assume that the manufacturer packages the single syringe offering into boxes of 6, and again into larger containers of 24. Each of those packaging options needs its own UDI as well.
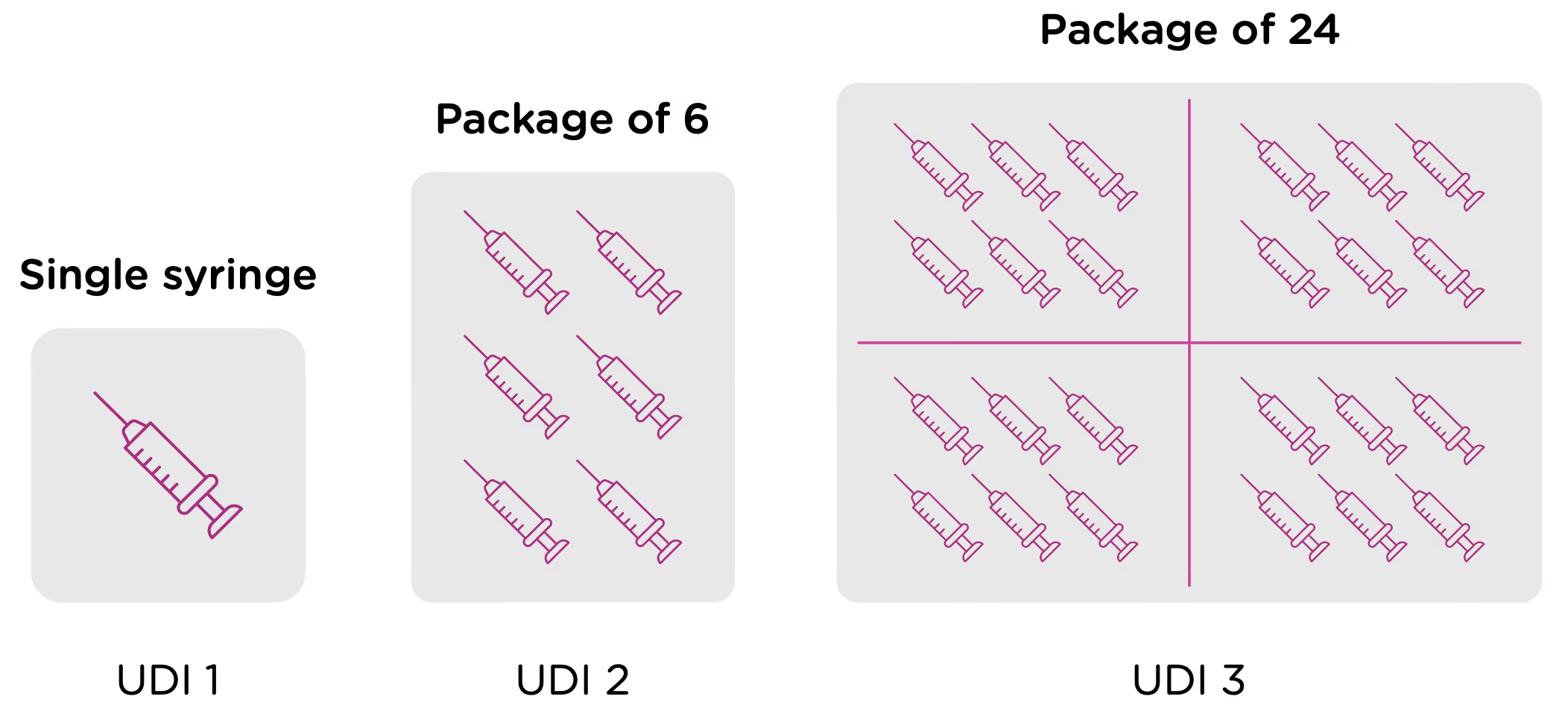
Labeling
In addition to obtaining UDI code for each device as outlined in the previous section, medical device manufacturers are required to ensure that devices are appropriately labeled with the assigned UDI. This label is called the UDI Carrier. The UDI is represented in two forms on the UDI Carrier: a machine-readable form and a human-readable form.
The machine-readable form or automatic identification data capture (AIDC) is a barcode or some other technology that can be used to automatically capture UDI information. The NMPA regulations support 3 types of machine-readable formats: 1-dimensional barcode, 2-dimensional barcode, and radio-frequency identification (RFID).

The regulations note that “use of advanced automatic identification and data collection technologies is encouraged”—prompting manufacturers to use more modern 2D and RFID machine-readable carriers where possible. Note, however, that if a device uses RFID, the UDI Carrier must also include the UDI in barcode format.
The human-readable form or human-readable interpretation (HRI) is the numeric or alphanumeric code for the UDI that can be read and manually entered into systems.

The UDI Carrier should be included on the device and on all levels of packaging. The UDI Carrier must be clear and readable during the operation and use of devices. If there isn’t room on the device for both the human and machine-readable forms of the UDI, then manufacturers should prioritize the machine-readable form.
UDI database
The third component of the NMPA UDI system is the UDI database. This is a centralized database of UDI and product information, administered by the NMPA. Manufacturers are required to submit UDI information into the database within 60 days after a product is approved (for sale in China) and before it is commercialized. The database contains a more detailed product record than what is included in the UDI itself, and it is the responsibility of the manufacturer (and/or their in-country representative) to submit the information correctly, and ensure that it’s kept up to date.
Chapter 3 of this eBook goes into detail about the specific fields and data requirements for UDI database submissions.
To continue reading this eBook including information about UDI format requirements and issuing entities, implementation timelines, and affected device types, please register to download the full version.

The ultimate guide to the EU MDR/IVDR unique device identifier (UDI) System
This article is an excerpt from The ultimate guide to the EU MDR/IVDR UDI ebook.
Table of contents
- Overview
- UDI basics and benefits
- UDI format requirements and issuing entities
- UDI rules for specific device types
- Implementation of UDI and UDAMED in the European Union
- US vs EU UDI comparison
The EU Medical Device Regulation (2017/745) (“MDR”) and EU In Vitro Diagnosis Regulation (2017/746) (“IVDR”) introduce two new systems for information exchange: UDI (Unique Device Identifier) for device identification and EUDAMED (European Databank on Medical Devices) to centralize and disseminate information. UDI is a specific code assigned to all devices and higher levels of packaging. This will allow for devices being sold in the European market to be identified and traced through a globally harmonized approach. EUDAMED is the IT system developed by the European Commission to replace the EUDAMED2 database previously in place under the Medical Device Directives (MDD). EUDAMED is a multi-functional system that will be used to coordinate device registration, provide information about devices to industry professionals and the public, and highlight necessary safety details.
The EU MDR and IVDR UDI system is based upon the guidance of the International Medical Device Regulators Forum (IMDRF). It’s a globally harmonized system that’s designed to increase patient safety and optimize care.
UDI system goals
Increase patient safety
- Improve tracing of devices
- Reduce the presence of counterfeit devices
Ensure access to accurate information
- Unambiguous identification of devices throughout distribution and use
Improve post-market surveillance
- Improve accessibility of adverse event reports
Enhance supply chain Management
- Streamline supply chain process and inventory management
- Simplify medical device documentation processes
The UDI system has four key elements
Element 1: Assignment of UDI (UDI Components)
The first element of the UDI system is the assignment of a UDI. The UDI is a code of alphanumeric characters that acts as the access key to information about a specific medical device on the market. The EU MDR and EU IVDR requires that a UDI be assigned to all medical devices except for custom-made or investigational devices. There are three components of a UDI:
- Basic UDI-DI
- UDI (consisting of UDI-DI and UDI-PI)
- Packaging UDI (Note: This is not an official term used in the EU MDR and IVDR, but we’re using it to help explain the concept. The Packing UDI is part of the UDI itself.)
1. Basic UDI-DI
The Basic UDI-DI identifies the device group that a particular device fits into. A device group is a group of products that all share the same intended purpose, risk class, essential design, and manufacturing characteristics. A device group is generally classified by medical device manufacturers as a “Product Family” or “Product Category,” depending on the internal nomenclature used within the company. The Basic UDI-DI functions as a parent or higher-level descriptor of a device.
NOTE: There can only be one Basic UDI-DI per UDI-DI.
The Basic UDI-DI is not printed on the product itself or on the packaging of a product, but rather it must be included in the following documents and applications:
- Certificates (Including Certificate of Free Sale)
- EU Declarations of Conformity
- Techical Documentation
- Summary of Safety and Clinical Performance
2. UDI (UDI-DI and UDI-PI)
The second component is the UDI itself, which consists of two parts:
Device Identifier (DI)
Production Identifier (PI)
The UDI-DI (Device Identifier DI, also referred to as “static”) identifies specific, detailed information about a particular device. If any of the below details should change, the device will need a new UDI-DI.
- Name or trade name of the device
- Device version or model
- If labelled as a single use device
- Packaged as sterile
- Maximum number of uses
- Need for sterilization before use
- Quantity of devices provided in a package
- Critical warnings or contra-indication
- CMR/endocrine disruptors
NOTE: There can be several UDI-DIs for one Basic UDI-DI.
Meanwhile, the UDI-PI (Production Identifier PI, also referred to as "dynamic") contains manufacturing information (including serial number, lot/batch number, software identification, and manufacturing or expiry date or both types of dates.)
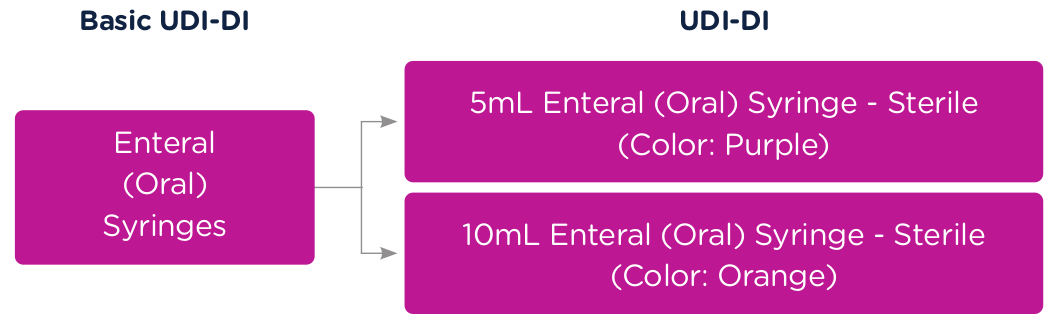
To better illustrate this concept of Basic UDI-DI and UDI (UDI-DI and UDI-PI), let’s use a syringe as an example. The Basic UDI-DI would identify the category of a syringe, for example, "Enteral (Oral) Syringe."
A 5ml Enteral (Oral) Syringe – Sterile (Color: Purple) would get a unique UDI-DI and a 10m Enteral (Oral) Syringe – Sterile (Color: Orange) would get a unique UDI-DI. Both products would be associated to the same Basic UDI-DI. In this case, the "Enteral (Oral) Syringe," which defines the category.
Each time that 5ml Enteral (Oral) Syringe – Sterile (Color: Purple) is manufactured at the same revision, it will get a new UDI-PI per lot. See the graphic below.

Each product is identical and therefore has the same UDI-DI. However, the UDI-PI changes to reflect the manufacturing date, lot number, expiry date, and serial number, as applicable.
The UDI will contain all device-specific information and have the same functions as the comparable database (GUDID) of the United States FDA. The main difference (in EUDAMED) is that the UDI data is divided into components of Basic UDI-DI, UDI, and Packaging UDI.
3. Packaging UDI
The third component of UDI is the Packaging UDI. (Note: This is not an official term used in the EU MDR and IVDR, but we’re using it to help explain the concept.)
Each level of packaging, except shipping containers, must receive its own unique UDI. Packaging UDI refers to the unique UDI assigned to higher levels of packaging instead of the device itself.
In the event of significant space constraints on the unit of use packaging, the UDI Carrier may be placed on the next higher packaging level.
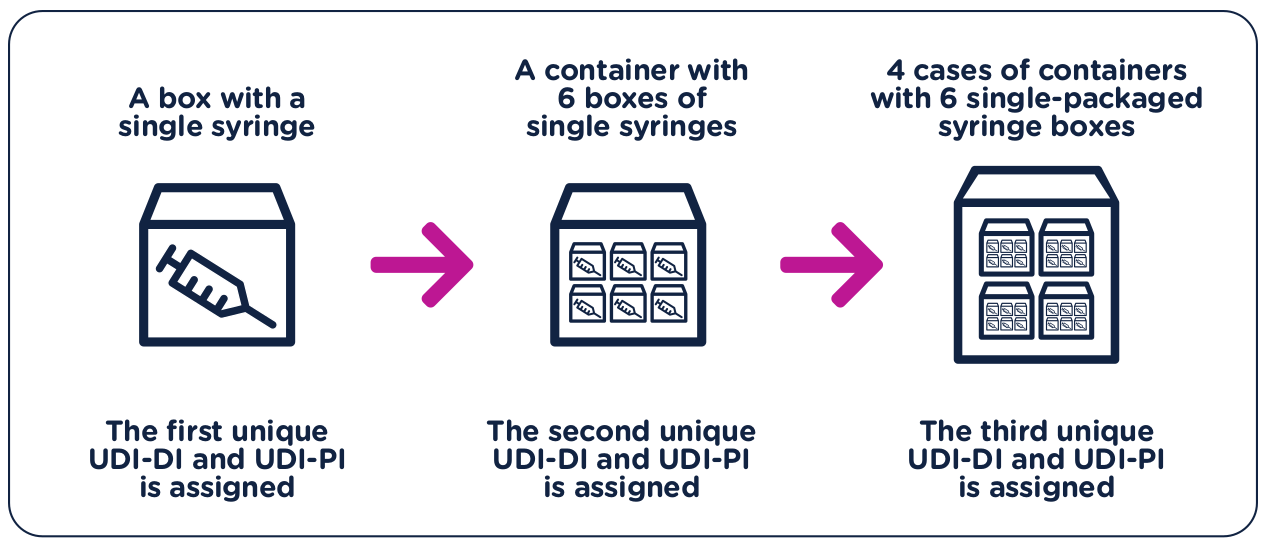
Returning to our earlier example of syringes, if a manufacturer first packages a single sellable syringe into an individual box, this package would receive its own UDI-DI and UDI-PI.
If then the manufacturer packages those individual boxes into containers of six (6), those containers would receive their own UDI-DI and UDI-PI.
And finally, if the manufacturer packages those six (6) containers into cases of four (4), those cases would receive their own UDI-DI and UDI-PI.
Each of those levels of packaging must be assigned its own UDI-DI and UDI-PI. The initial syringe did not change, but the way it is packaged did, therefore, requiring its own UDI-DI and UDI-PI.
Element 2: Placing UDI on the device and/or packaging
The second element to the UDI system is the placing of the UDI on the device or on its packaging through what is referred to as a “UDI Carrier.” The UDI Carrier is the part of the label that contains the UDI information that is applied directly to the device or included on the device packaging. The UDI Carrier should have both a machine-readable portion (AIDC) and a human-readable portion (HRI). (Specific details about each element of the UDI will be covered in Chapter 2.)
- Machine-readable form – AIDC – (Automatic Identification and Data Capture) is a barcode or other machine-readable technology that can be accessed automatically by scanning the UDI information.
- Human-readable form – HRI – (Human Readable Interpretation) is the numeric or alphanumeric code, which can be manually entered into the system for access to the UDI information.
If there are space constraints limiting the use of both the AIDC and HRI on the label, then only the AIDC is required to appear. However, on devices that are intended to be used in home-health care or other non-medical facility settings, the HRI would be required to appear.
Single-use devices may contain the UDI Carrier on its lowest level of packaging rather than on the device itself.
Reusable devices must include the UDI Carrier on the device itself, unless any type of direct marking would interfere with the safety or performance of the device, or if it is not technologically feasible to directly mark the device. If so, this should be properly documented in your design history file.
Most importantly, the UDI Carrier must be readable for the intended lifecycle of the device.
Below is an example of a GS1 AIDC and HRI barcode label.
Element 3: Storage of UDI information by Economic Operators
Storage of UDI information by "Economic Operators" is the third element of the UDI system. 2017/745 Articles 2(35), 22(1), and 22(3) define an economic operator as:
- A manufacturer
- An authorized representative
- A distributor
- An importer
- An investigator for clinical investigations
- A person who sterilizes systems or procedure packs
Class III, implantable device:
According to EU MDR 2017/745 Annex II, the manufacturer shall keep an updated list of all UDIs that it has assigned. Economic operators and all health institutions are required to store, preferably by electronic means, the UDI of all the devices for which they have supplied or with which they have been supplied.
For Devices Other than Class III:
Member States are encouraged, and in some cases require, health institutions to store, preferably by electronic means, the UDI of the devices with which they have been supplied. The UDI must also be included in any field safety notice for reporting serious incidents and field safety corrective actions.
The EU MDR and EU IVDR also give the European Commission authority to make additional requirements regarding the submission or maintenance of UDI information. In making those decisions, the European Commission must consider six (6) areas:
- Confidentiality and data protection
- Risk-based approach
- Cost-effectiveness of the additional measures
- The need to avoid duplications in the UDI system
- The needs of the healthcare systems of the member states
- Harmonization with other medical device identification systems
To continue reading this eBook including information about the EUDAMED database, UDI format requirements and issuing entities, implementation timelines, and key differences between the EU and US UDI systems, please register to download the full version

FDA Class II medical devices
What are medical device classes within the FDA?
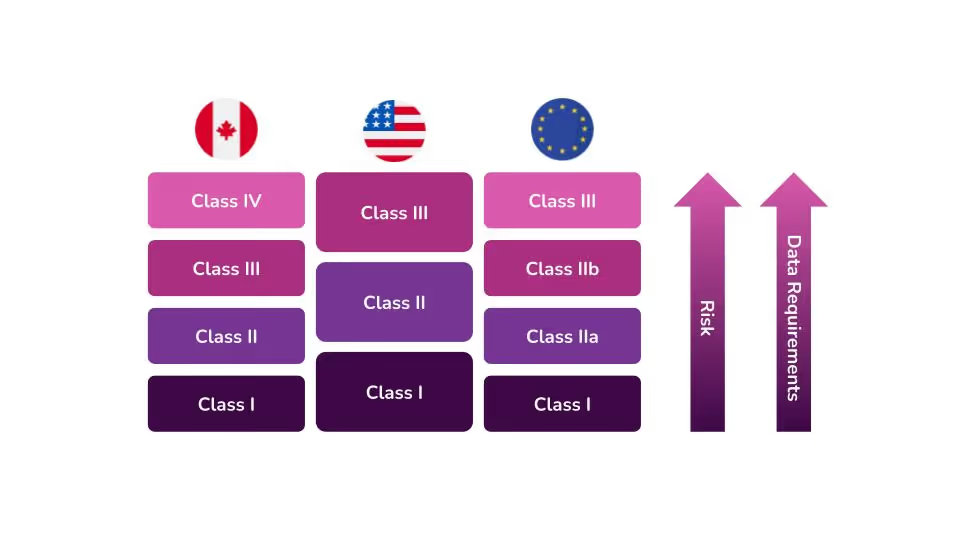
In the United States, the Food and Drug Administration (FDA) categorizes medical devices into three classes. They base these classes largely on the level of perceived risk the device may have. The level of perceived risk determines the data requirements and controls that need to be put into place to ensure safety for patients and/or users.
The FDA determines the level of oversight necessary for each device based on three factors. According to the FDA’s guidance on how to classify your device, device classification depends on the intended use of the device and also upon indications for use. The third and most important criterion is the device's risk to patients and users. The higher the risk associated with the device, the higher the class of that device will be, i.e Class I devices represent the lowest risk, and Class III devices pose the highest risk.
What are Class II Medical Devices?
Class II medical devices, which pose a medium to high risk to patients and users, account for 43 percent of all medical devices in the United States. Some common examples of Class II devices are syringes, pregnancy test kits, electric wheelchairs, and catheters. Class II medical devices must adhere to the provisions of the General Controls as mandated by the Food, Drug, and Cosmetic (FD&C) Act, which applies to all classes of devices.
The FDA also has its own Product Classification Database that can be used to assist in your device’s classification, finding consensus standards and submission types, such as a 510(k) or PMA.
What is the approval process for Class II Medical Devices?
All non-exempt Class II medical devices must go through the premarket notification process, also known as the 510(k). The 510(k) is a premarket submission process used to demonstrate that a device is safe and effective based on its substantial equivalence to a device already on the market, known as a predicate device.
Determining the substantial equivalence of your new device boils down to two things:
- Establishing that your device has the same intended use as the legally marketed predicate device
- Establishing that any technological differences between your device and the predicate device have no negative impact on the effectiveness and safety of the device
Any device with no identified predicate device, including those with a lower risk profile, is automatically classified as a Class III device and must use the more rigorous premarket approval (PMA) submission to receive market approval. Lower-risk devices can request reclassification, however, through a De Novo submission.
Class II medical devices in other countries
Device classification is different in each country. With that in mind, you should not make any assumptions regarding classification in other countries because your device is a Class II device in the United States. Each country with medical device regulations has its own classification scheme that may cause your device to be regulated differently.
During the initial phase of planning for the global commercialization of a product, it is imperative to consider international regulations, their classification schemes, and the registrations that each country will require.
The process of getting a Class II medical device to the market is arduous, and regulatory professionals must navigate disjointed manual data systems and processes. Plus, ever-evolving regulations make it difficult to ensure your new products, and even ones already on the market, are compliant.
Regulatory information management (RIM) software is an almost invaluable tool that can help your company get products to market more quickly and cost-effectively by digitizing and automating regulatory activities in a single system. The right RIM software can make the 510(k) process simpler and more efficient than ever before.
For more information on the 510(k) process, read our Beginner’s guide to the 510(k).

What's up with the duck?
If you’ve seen us online or at tradeshows, you might be wondering, “What’s up with the duck?” His name is Reggie by the way, and we’re pretty fond of him around here. Rimsys is more than software. It’s a team built from the ground up who understand the importance and challenge of managing regulatory affairs in the ever-evolving medical device industry. Our goal here at Rimsys is to help your company get its regulatory ducks in a row, and from that concept, “Reggie”, the regulatory duck was born.

If you could be a part of our company meetings, you’d see that we all love Reggie. After all, he’s more than a mascot to us. He symbolizes our mission to improve global health by accelerating delivery and increasing the availability of life-changing medical technologies. Reggie is our promise to our customers that you’re getting more than software with Rimsys. You’re getting a team of dedicated regulatory experts who understand the urgent need for better regulatory information and processes. That's why we love Reggie, our regulatory duck, and we believe you will too.

Brexit overview for medical device manufacturers
What is Brexit?
Brexit - meaning "British exit" is the process of the official withdrawal of the United Kingdom (UK) from the European Union (EU) on January 31, 2020, at 11:00 PM (GMT). The UK had been a member state of the EU since January 1, 1973, when it was known as the European Communities.
Leaving the EU was no easy task for the UK and it was six years in the making before it was final. When they “left” in January 2020, a discussion and negotiation transition period with the EU began. The negotiation process was both politically challenging and deeply isolating. Under the UK Prime Minister, Boris Johnson, the country continued to participate in many EU institutions during the one-year transition period in order to ensure frictionless trade until a long-term relationship could be agreed upon. Trade deal negotiations continued up until just days before the scheduled end of the transition period (December 31, 2020) and the EU–UK Trade and Cooperation Agreement was signed on December 30, 2020.
Following Brexit, EU law and the Court of Justice of the European Union no longer have power over British citizens and companies, with the exception of select areas related to Northern Ireland. Under the terms of the Brexit withdrawal agreement, Northern Ireland continues to participate in the European Single Market in relation to goods and to be a de facto member of the EU Customs Union.
The European Union Referendum Act 2015 set the wheels in motion. This Act of the Parliament of the United Kingdom made a legal provision for a referendum to be held on whether it should remain a member state of the European Union or leave it completely. The related legislation was introduced to the House of Commons in May of 2015, and it was passed on its third review in the House of Commons in early September 2015 and approved by the House of Lords in December 2015. The Act went into full legal force on February 1, 2016.
The initial withdrawal in March 2019 was delayed by the deadlock in the British parliament after the June 2017 general election. This deadlock then led to three extensions of the UK’s Article 50 of the Treaty of European Union (TEU), which began the member states’ withdrawal, known as Brexit.

Brexit’s effect on medical device regulations
All medical devices, including IVDs, custom-made devices, and systems or procedure packs must be registered with the UK’s Medicines and Healthcare Products Regulatory Agency (MHRA) before they can be placed on the UK market. The MHRA is developing a new regulatory framework for medical devices, designed to safeguard and advance the health of its people by enabling early access to a high-quality supply of safe, effective, and innovative medical products. CE marked devices will initially be recognized in the UK, but manufacturers will have to obtain UK Conformity Assessment (UKCA) certification and follow the marking requirements per UK MDR 2002, beginning July 1, 2023. CE-marked devices will be allowed in the UK market until June 30, 2023, as long as they have been CE marked under one of the following:
- Directive 90/385/EEC - active implantable medical devices
- Directive 93/42/EEC
- Directive 98/79/EC - in vitro diagnostic medical devices
- Regulation 2017/745
- Regulation 2017/746
Medical device manufacturers continue to be able to self-certify CE marked devices until June 30, 2023 - providing the certificates remain valid for the EU market under the transitional timelines listed in the EU MDR and IVDR.
From January 1, 2022, non-UK manufacturers will require a UK Responsible Person for the purposes of registering devices. A Northern Ireland-based Authorized Representative will no longer be able to register devices on a manufacturer’s behalf for Great Britain.
You will need to use the new UKCA marking before January 1, 2023, if your product:
- will be marketed in Great Britain, and
- is covered by legislation that requires the UKCA marking, and
- requires mandatory third-party conformity assessment, and
- conformity assessment has been carried out by a UK conformity assessment body.
This does not apply to existing stock if your goods were fully manufactured, CE marked, and placed on the market before January 1, 2021.
Northern Ireland – the rules are different
In some circumstances, it is a requirement of the UK MDR 2002 that you inform the MHRA when you first place your device on the Northern Ireland market. Under the Northern Ireland Protocol, different rules apply than those in Great Britain. The precise requirements depend on the location of the manufacturer, the location of the Authorized Representative, and the device class. For more information on the regulatory system for medical devices in Northern Ireland, refer to the Regulation of medical devices in Northern Ireland.
The future of medical device regulations under Brexit
As you can see, the rules have changed and may continue to be refined until June 30, 2023. Currently, the CE marking is only valid in the UK for areas where both UK and EU rules remain the same. The UKCA marking is not recognized in the EU market, therefore, products will need the CE marking to sell in the EU. The UK MDR 2002 is up to date with all changes known to be in force on or before June 28, 2022. However, there may be changes that will be brought into force at a future date.
For more information on the EU MDR and IVDR requirements, read our Ultimate guide to the EU MDR/IVDR unique device identifier (UDI) system and Ultimate guide to the EU MDR GSPR - general safety and performance requirements.

The RegUP rundown
What is a RegUP?
The medical device industry is, by its very nature, a high-stress one. New medical technologies are being created all the time, and as a result, regulations are constantly changing. Being a regulatory professional in the medtech industry requires extraordinary attention to detail and nerves of steel. Rimsys was founded by regulatory pros for regulatory pros, and we understand the need to unwind in a professional environment with other leaders in the industry. That’s why we came up with the idea of the RegUP.
So, what’s a RegUP? It’s short for “Regulatory Meetup,” and it’s a small gathering of regulatory professionals, not a large conference. We’ll enjoy delicious food and beverages as we get to know each other and discuss regulatory trends and best practices.
When and where?
Boston - Sept 29th
Our first RegUP event will be held on the East Coast in Boston, MA, on September 29, 2022, at Democracy Brewing. Democracy Brewing, nestled in historic Downtown Crossing (one of the oldest neighborhoods in the United States), is the first cooperative brewery in Boston. Their menu features plenty of delicious craft beers and an eclectic selection of cuisines ranging from Mediterranean to classic American bar food.
San Jose - Oct 13th
Our second event will be held on the West Coast in the San Jose area on Oct 13, 2022, at Big Dog Vineyards. Big Dog Vineyards is a locally owned and operated winery in the picturesque Milpitas Hills, CA. Their Winery & Tasting Room opened in 2009, right beside the estate vineyard, which was planted in 1997.
What should you expect at a RegUP event?
As mentioned, we understand that regulatory professionals in the medical device industry are under constant pressure to ensure they keep up with ever-changing trends and best practices. And if you are like us, the opportunity to hone your trade and sharpen your skills and knowledge in a more casual setting will be welcome.
Here’s the agenda for RegUP Boston to give you an idea of what to expect at our events:
- 12:00 - 12:30 pm Welcome: Increasing confidence in regulatory planning. Many regulatory challenges are driven by a lack of visibility into regulatory timelines, resources, and needs. A comprehensive regulatory data strategy can help RA teams build more resilient plans, and shift their organizational posture from reactive to proactive.
- 12:30 - 1:15 pm Catered lunch
- 1:15 - 1:45 pm TBD Regulatory best practices case study
- 1:45 - 2:15 MDR/IVDR information essentials: MDR/IVDR compliance remains top of mind for RA teams. New information requirements including GSPRs, UDI/EUDAMED, and Post-market surveillance and reporting require a new approach to regulatory information management.
- 2:15 - 4:00 pm Brewery tour, tasting, and networking
Rimsys Speakers
- James Gianoutsos - Founder & CEO
- Bruce McKean - Director of Regulatory (Boston)
- Adam Price - Director of Product, Post Market (San Jose)
We hope to see you there!
Our RegUP events in Boston and San Jose will be the first of many opportunities for us to network, further regulatory knowledge and processes, and even enjoy each other’s company over tasty beverages. Best of all, these events are free for Rimsys customers and qualified guests.
Of course, you can also expect these events to get bigger and better with time. Nonetheless, you don’t want to miss out on the first of these opportunities to get to know us and our industry better. We hope to see you there! If you are unable to attend though, keep an eye on our LinkedIn page for future RegUP events in a city near you.
To get more information and register for our upcoming events, click the links below:
- RegUP Boston: https://regup-boston.eventbrite.com/
- RegUP San Jose: https://regup-sanjose.eventbrite.com/

IVDR: In Vitro Diagnostic Regulation within the European Union
What is the IVDR In Vitro Diagnostic Regulation?
The European Union’s In Vitro Diagnostic Regulation (IVDR) 2017/746 applies to IVD devices and came into force on May 26, 2022. The IVDR is a major change over the In Vitro Diagnostic Directive (IVDD), which it supersedes. The new regulation is designed to better protect patients and address changes in IVD technology through new requirements and stricter controls. As a Regulation, unlike a Directive, the IVDR becomes a requirement in every EU country on the same day, which means that compliance with the IVDR is paramount for market access within the EU.
Major changes in the IVDR
The IVDR includes changes to IVD classification, increased documentation requirements, and UDI specifications. It is critical for manufacturers and their European representatives to understand and implement the new regulations as soon as possible. There is significant concern that notified bodies will not have sufficient resources to handle the increased need for their services.
The major changes between the IVDR and its predecessor, IVDD, are as follows:
Changes to the classification system
Under the IVDD only a small percentage of IVD products were assigned a higher risk classification (based on a predefined list of products). All other products were exempt from notified body oversight and allowed for manufacturers to self-certify through conformity procedures. Under the IVDD, only 10%-20% of IVD products were subject to notified body oversight, whereas, under the IVDR, 80%-90% of IVD products will be subjected to notified body oversight.
Unlike the IVDD, the IVDR defines 4 risk classes based on risk profile:
- Class A: Lowest risk (e.g. specimen containers)
- Class B: Low to moderate risk (e.g. pregnancy tests)
- Class C: Moderate to high risk (e.g. cancer screening products)
- Class D: High risk (e.g. HIV tests)
It is important that IVD manufacturers re-classify their products using the new classification rules as soon as possible. Notified body oversight is required for IVDs in class B through class D.
Increased technical documentation requirements
Under the IVDD, technical documentation requirements were vague and left largely to the discretion of the manufacturer. The IVDR, however, details specific requirements for the content of technical documentation. Annex I details the General Safety and Performance Requirements, Annex II details primary technical documentation requirements, and Annex III details requirements for technical documentation for post-market surveillance.
Unique Device Identification (UDI) requirements
IVDs now require UDI labeling and registration in the European Union Database of Medical Devices, more commonly known as EUDAMED, in the same way as other medical devices. A UDI must be assigned to all medical devices, with some exceptions for custom-made and investigational devices.
Each UDI consists of multiple elements, including a Basic UDI-DI (also known as “BUDI”), a device identifier (DI) with static device information, and a product identifier (PI) with dynamic information provided by the manufacturer (such as serial number and manufacturing date). In addition, manufacturers can now register their device in EUDAMED, though this is not yet required.
Quality management system requirements
All IVD manufacturers are expected to have a quality management system in place, even though only those manufacturing class B to D devices require certification of conformity assessments by a notified body.
Person Responsible for Regulatory Compliance (PRRC)
Manufacturers will now be required to designate at least one person to monitor compliance with regulatory requirements. A PRRC must be qualified by way of a relevant degree and a minimum of one year of professional experience, or at least 4 years of experience in medical device regulatory affairs or quality management. Note that smaller manufacturers do have the option to subcontract their PRRC functions, but one person cannot act as a PRRC for a manufacturer based outside of the EU and for an Authorized Representative.
IVDR deadlines
Manufacturers who were able to self-declare conformity under the IVDD, but require a notified body under IVDR may continue to place IVDs on the market assuming they had issued a declaration of conformity prior to the original May 26, 2022 deadline, introduce no significant changes to the product, meet all post-market surveillance and vigilance requirements, and register in EUDAMED as specified in the IVDR. Assuming that these requirements are met, the new transition dates are as follows:
- May 26, 2022 - All new devices and non-sterile self-declared devices
- May 26, 2025 - Class D devices
- May 26, 2026 - Class C devices
- May 26, 2027 - Class B devices and Class A sterile devices
IVD regulations outside of the EU
This article is specific to requirements in the EU. It is important to note that other countries, such as the United States, have their own regulations related to In Vitro Diagnostics that are covered by the country’s medical device regulations. Each country with medical device regulations has its own classification scheme that may cause your device to be regulated in a different way. During the initial phase of planning for global commercialization of a product and throughout the product life cycle, it is imperative that you consider international regulations, their classification schemes, and the registrations that each country will require.
For additional information, The ultimate guide to EU MDR and IVDR general safety and performance requirements and also The Ultimate Guide to EU MDR/IVDR UDI.

CE marking guide for medical devices in the European Union
This article is an excerpt from the CE marking guide for medical devices in the European Union.
Table of Contents
- What is CE marking?
- Why is CE marking important?
- CE marking responsibilities
- What countries require or accept CE marking?
- Which medical devices require a CE mark?
- Technical documentation
- What are the costs associated with CE marking?
- How do you apply the CE marking?
- CE mark and UDI
- Does the CE mark expire?
- Do I need to CE mark my software?
- Final steps
CE marking is a symbol that consists of “CE, “ which is the abbreviation of the French phrase "Conformité Européene" meaning "European Conformity". The term initially used to describe “CE” was "EC Mark" but it has officially been replaced by "CE marking" according to the EU Directive 93/68/EEC. CE marking is used in all EU official documents, although you will still see "EC Mark" being used in common language. If you are using EC Mark in your documentation, you should change that terminology to CE marking in the future.
The letters ‘CE’ appear on many products traded on the Single Market in all the member states of the European Union plus Iceland, Liechtenstein, Norway and Switzerland. Simply put, The CE mark is a mandatory compliance mark, informing the consumer that the product is compliant with all applicable EU directives and regulations where the CE mark is required.
The Single Market was established in 1993 and is still considered one of the most significant achievements of the European Union. The main goal was to ensure the movement of goods and services freely within all the member states and to establish high safety standards for consumers. The CE mark indicates that goods and services do not need to be verified when shipping into another member country. To further support this movement, in April 2011, the Single Market Act was established to boost growth and strengthen confidence in the economy even further.
CE marking is required for many types of products, not just medical devices. The CE symbol can be found on bicycle helmets, toys, laptop batteries, wheelchairs, construction equipment, gas appliances and cell phone chargers - to name a few. CE marking is required for products manufactured anywhere that are sold in the EU, and only for those products for which EU specifications exist and require CE marking. The CE marking signifies that the product has been found to meet the general safety and performance requirements (GSPRs) of the European health, safety and environmental protection legislation and allows the product to be sold in the EU.
Manufacturer responsibilities for CE marking
Medical device manufacturers are responsible for properly and legally CE marking products before they leave the warehouse.
Most Class II and III medical devices, along with IVDs and some Class I devices, require a conformity assessment performed by a Notified Body to ensure that all legislative requirements are met before it can be placed on the market. Manufacturers of most Class I devices can self assess conformity. This process needs to demonstrate that all the legislative requirements are met, including any testing and inspections, and that all necessary certifications are obtained.
The European Commission lists 6 steps that manufactures should follow to affix a CE marking to their devices:
- Identify the applicable directive(s) and harmonized standards - see EU standards for Medical Devices, In Vitro Diagnostic (IVD) devices, and Implantable Medical Devices.
- Verify product specific requirements using the essential principles identified in the above standards.
- Identify whether an independent conformity assessment by a Notified Body is necessary. Notified bodies will be required to verify compliance with relevant Essential Requirements for most medical devices classified as IIa, IIb, or III - along with sterile class I devices. See the Notified and Designated Organization (NANDO) database for available notified bodies.
- Test the product and check its conformity.
- Create and keep available the required technical documentation.
- Affix the CE marking and create the EU Declaration of Conformity.
Importer responsibilities for CE marking
If you are importing medical devices into the EU, it is your responsibility to review all the technical documentation and maintain a copy, or to make sure that it’s available to you upon request.
You should verify:
- That the device has been CE marked and that the EU declaration of conformity has been completed.
- That the manufacturer has designated and established an authorized representative.
- That the device is labeled appropriately and contains instructions for use (IFU).
- When applicable, that a UDI has been assigned to the product.
- Whether or not the product is registered in EUDAMED (registration is currently voluntary).
Take action:
- List your name and address on the device or packaging, in addition to the manufacturer’s information.
- Keep records of complaints, non-conformities, recalls, etc. on file.
- Report any noticed non-conformity or product complaints from end users to the manufacturer and authorized representative immediately.
- Maintain a copy of the EU declaration of conformity and any other relevant certificates.
Distributor responsibilities for CE marking
If you are a distributor, you are responsible for reviewing the technical documentation provided to you so that you can verify the product is safe to put on the local market. You must also be sure the product is labeled correctly with the CE marking symbol clearly visible. The technical file documentation contains all of the information that is necessary to show conformity of the product to the applicable requirements.
You should verify:
- That the device has been CE marked and that the EU declaration of conformity has been completed.
- That the device includes all the appropriate labeling, including instructions for use.
- That if imported, the importer has complied with all the EU regulations.
- When applicable, that a UDI has been assigned to the product.
Take action:
- Report any noticed non-conformity to the manufacturer, importer, and authorized representative immediately.
- If a product appears to be out of compliance to the regulations and could pose a serious risk, the information should be reported to the Competent Authority, and to the manufacturer, importer and authorized representative.
- Any complaints or reports from end users about the product should be reported to the manufacturer and, if necessary, to the importer and authorized representative.
Important note: If the importer or distributor markets the product under their own company name, then they become responsible for CE marketing, and take over that role from the manufacturer.
CE marking is mandatory when importing products into the European Union, which is part of the larger European Economic Area (EEA). The EEA Agreement, established in 1992 and made official in 1994, is an international agreement that enables the extension of the European Union’s single market to non-EU members. It consists of the 27 EU countries plus the four European Free Trade Association (EFTA) countries - Iceland, Liechtenstein, Norway and Switzerland. Today, the EFTA has 29 Free Trade Agreements (FTAs) with 40 countries and territories outside the EU. Because these countries operate in the single market, this allows free movement of goods and services across all of the EEA.

Source: European Environment Agency (EEA).
All medical devices sold in the EU require a CE mark. While a CE mark is not required for items such as chemicals and pharmaceuticals, it can be required for combination devices and medical device software. For these two situations, how do you know if your product requires a CE mark?
To continue reading this ebook, including an overview of CE mark costs, and the associated technical documentation/general safety and performance requirements (GSPRs) that manufacturers are required to maintain please register to download the full version




