

Featured
Rimsys Announces Rimsys AI to Eliminate Repetitive Tasks and Enhance Decision-Making for MedTech Regulatory Teams
Rimsys, the leading Regulatory Information Management (RIM) platform for the MedTech industry, today announced the launch of Rimsys AI, a suite of embedded artificial intelligence (AI) agents.

Post-market surveillance for medical devices in the European Union
This article is an excerpt from Post-market surveillance for medical device in the European Union.
Table of Contents
- What is post-market surveillance?
- What classes of medical devices require post-market surveillance?
- Components of a successful post-market surveillance plan
- PMS data requirements
- Post-market surveillance system goals
- Required post-market surveillance reporting
- Embracing post-market surveillance as an integral part of your quality program
- Getting started with post-market surveillance
Post-market surveillance (PMS) is designed to monitor the performance of a marketed medical device by collecting and analyzing field use data. Article 10 of the EU MDR and IVDR requires all device manufacturers to have a post-market surveillance system in place. The main elements of the PMS are laid out in Article 83, and additional details for lower-risk and higher-risk devices are covered in articles 84 and85, respectively.
In general, a PMS system consists of both proactive activities and reactive, or vigilance, activities. While post-market surveillance and vigilance are sometimes used interchangeably, vigilance consists of separate activities that feed post-market surveillance programs.
Post-market surveillance systems are used to collect and analyze data not only about the manufacturer’s device but also about related competitors’ devices that are on the market. Data collected through PMS procedures is then used to identify trends that may lead to, among other things, quality improvements, updates to user training and instructions for use, and identification of manufacturing issues.
Note that “market surveillance” encompasses activities performed by a Competent Authority to verify MDR compliance, and should not be confused with the topic of this ebook,“post-market surveillance," which is performed by the manufacturer.
All medical devices marketed in the EU require some level of post-market surveillance, and all medical device manufacturers must implement a post-market surveillance system (PMS). The requirements of the PMS, however, vary and should be “proportionate to the risk class and appropriate for the type of device” (MDR Chapter VII). In particular, the type and frequency of reporting vary based on a device’s risk class.
A post-market surveillance plan (PMS) is an integral part of a manufacturer’s quality management system and provides a system for compiling and analyzing data that is relevant to product quality, performance, and safety throughout the entire lifetime of a device. The PMS should also provide methods for determining the need for and implementing any preventative and corrective actions. A PMS system should include and define:
Surveillance data sources
With the increased focus on proactive risk identification in the MDR, it is important to design post-market surveillance systems that actively acquire knowledge and detect potential risks. It is not sufficient to rely solely on spontaneous reporting by healthcare providers, patients, and other stakeholders.
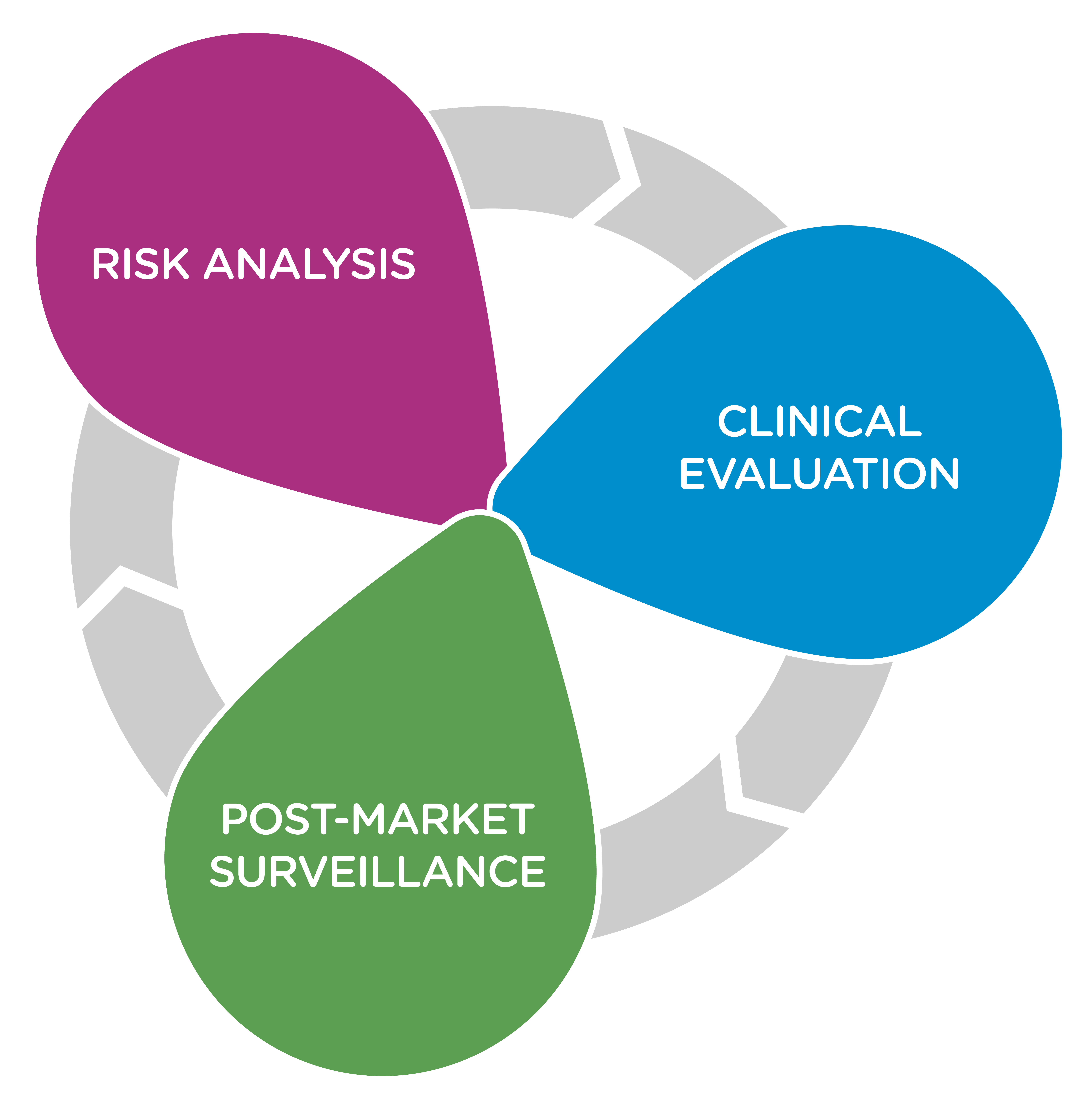
In addition to information coming from Clinical Evaluation Reports and complaint and adverse event reporting, typical sources of surveillance data include:
• Social media networks: Because many of your stakeholders may be communicating on social media networks, it is important to employ social listening techniques and/or tools to identify issues and concerning trends as they develop.
• Industry and academic literature: Any studies, academic papers, and other literature that addresses similar devices or the specific use cases for which your device is designed should be evaluated. In particular, risk factors and adverse events identified with similar devices should be closely examined. It is also important to identify newer technologies that may affect the benefit-risk ratio and establish a new definition of “state of the art” for the device type.
• EUDAMED: While the European Database on Medical Devices (EUDAMED) is not yet fully functional, it is intended to provide a living picture of the lifecycle of all medical devices marketed in the EU. Manufacturers should take special care to consider information for similar devices made available through the EUDAMED system in the future.
• Registries: Patient, disease, and device registries can provide information that informs the clinical evaluation process which provides input into the post-market surveillance system.
Data analysis methodology
A well-defined data analysis methodology will accurately identify trends and lead to defendable decisions in the application of post-market experience. Once the necessary information has been identified and collected, and potentially cleaned of incomplete or otherwise unusable data, the data needs to be analyzed.
The goal is to identify meaningful trends, correlations, variations, and patterns that can lead to improvements in the safety and efficacy of the device. There are many data analysis tools available that can assist with:
• Regression analysis that will identify correlations between data (e.g. the device location/geography correlates to battery life).
• Data visualization that can be useful in spotting trends in the data.
• Predictive analytics, which can be particularly useful with large data sets, to identify future trends based on historical data.
• Data mining, which is also normally used with large datasets, to organize data and identify data groups for further analysis.
Benefit-risk indicators and thresholds
The MDR requires that medical device manufacturers not only demonstrate the clinical benefit of their device but also quantify the benefit-risk ratio. The benefit of a device must be shown to clearly outweigh the risk for it to gain market approval. Article 2 (24) of the MDR defines the benefit-risk determination as “the analysis of all assessments of benefit and risk of possible relevance for the use of the device for the intended purpose when used in accordance with the intended purpose given by the manufacturer.”
A PMS system should clearly define benefit-risk calculations and the data used to support them. Post-market surveillance activities are critical in order to re-evaluate and maintain the benefit-risk calculations and determinations of a device throughout its life. Information that is gained through a PMS system can lead to:
• Identification of new risk factors.
• Adjustments to risk frequency and/or severity values based on actual use data.
• Adjustments to established risk calculations based on new “state of the art” technologies becoming available.
• Adjustments to established benefit calculations based on actual use data.
While complaint handling and other feedback tracking are more often described as part of post-market vigilance systems, they play a role in the more proactive post-market surveillance processes as well. A PMS system should define ...
To continue reading this ebook, download the full version.

An overview of 21 CFR Part 820 - quality systems for medical device manufacturers
What is 21 CFR Part 820?
21 CFR 820 is the FDA federal regulation that pertains to quality systems for medical device manufacturers, and it is part of the agency’s set of Current Good Manufacturing Practices (CGMP) for industry. Also referred to as the FDA’s quality system regulation (QSR), the regulation defines design controls and quality processes at all stages of device development in order to ensure that all medical devices marketed in the United States are safe and effective.
21 CFR 820 consists of 15 subparts, which define quality system requirements for each stage and function within the medical device manufacturing process. We define each subpart below.
Federal regulations are organized as Title → Chapter → Subchapter → Part, which means that 21 CFR 820 is short-hand for:

21 CFR 820 vs ISO 13485
ISO 13485 is the de facto international quality system standard for medical device manufacturers, but this is not currently the standard in the United States. While Part 820 and ISO 13485 are structured differently, they have no conflicting requirements. Therefore, companies that are marketing medical devices in the U.S. and in other markets will need to comply with both ISO 13485 and the FDA’s QSR, as defined in 21 CFR 820.
However, the FDA is moving towards harmonizing these standards, and on February 23, 2022 issued a proposed rule to amend the QSR to align more closely with the international consensus standard for Quality Management Systems, primarily by incorporating reference to the ISO 13485 standard. The FDA has published FAQ’s about the proposed rule.
21 CFR Part 820 Requirements
Part 820: General Controls (subpart A)
The General Controls subpart contains three sections providing general information about the regulation, including the scope and applicability along with key definitions.
Scope
The regulation defines current good manufacturing practice (CGMP) requirements governing the methods, facilities, and controls used for the “design, manufacture, packaging, labeling, storage, installation, and servicing of all finished devices intended for human use." Specifically, this subpart defines:
- Applicability:
The requirements of this regulation are intended to ensure the safety and efficacy of all finished medical devices intended for human use that are manufactured in or imported into the United States. Manufacturers that are involved in some, but not all, manufacturing operations should comply with those requirements that are applicable to the functions they are performing.
Exceptions:
- This regulation does not apply to manufacturers of medical device components, but such manufacturers are encouraged to use this regulation as guidance.
- Class I medical devices are exempt from the Design Controls defined in this regulation, except for those listed in § 820.30(a)(2).
- Manufacturers of blood and blood components are not subject to this regulation but are subject to Biologics good manufacturing practices as defined in Subchapter F, Part 606 of the regulation.
Definitions
This section of the regulation contains definitions for a number of terms used throughout the document. The following are the major definitions related to quality records:
- Design history file (DHF): A compilation of records that describes the design history of a finished device.
- Design input: The physical and performance requirements of a device that are used as a basis for device design.
- Design output: The results of a design effort at each design phase and at the end of the total design effort. The finished design output is the basis for the device master record. The total finished design output consists of the device, its packaging and labeling, and the device master record.
- Device history record (DHR): A compilation of records containing the production history of a finished device.
- Device master record (DMR): A compilation of records containing the procedures and specifications for a finished device.
Quality System
The section of the regulation sets the basic requirement for a quality system by stating that “Each manufacturer shall establish and maintain a quality system that is appropriate for the specific medical device(s) designed or manufactured, and that meets the requirements of this part.”
The term “appropriate” is used throughout this regulation and can be open to interpretation. A manufacturer, however, should assume that all requirements are appropriate and applicable except in cases where non-implementation of the requirement can be shown to have no effect on the product's specified requirements or ability to carry out necessary corrective actions.
Quality system requirements (subpart B)
This section of the regulation defines the overall responsibilities and the resources required for the management of the quality system.
Management responsibilities
Executive management is responsible for establishing a quality policy and ensuring adequate resources to effectively maintain and manage the quality system. In addition, management is responsible for establishing a specific quality plan, consisting of relevant practices, resources, activities, and procedures.
Quality audit
Periodic audits of the quality system are required to be conducted by personnel not directly responsible for the activities being audited. The dates and results of each audit need to be documented, along with the results of the audit. It is expected that corrective actions and, when necessary, reaudits, be performed for any identified noncompliances.
Personnel
Manufacturers are responsible for assigning sufficient personnel with appropriate experience and training to perform all tasks required by the quality system plan.
Design controls (subpart C)
Manufacturers of all class II and class III medical devices, along with the specific class I devices listed in paragraph (a)(2) of this regulation, are required to establish design control procedures that ensure design requirements are met as specified.
Design controls shall define:
- Design and development planning - Plans that describe the design and development activities, and responsibilities for these activities and their implementation.
- Design input - Procedures that ensure design requirements are appropriate and address the intended use of the device.
- Design output - Procedures that document design output, including acceptance criteria, so that conformance to design input requirements can be adequately evaluated.
- Design review - Formal and documented reviews of the ensign results that include participation from representatives of all.
- Design verification - Procedures for verifying the device design that confirm that the design output meets the design input requirements.
- Design validation - Procedures for validating the device design, ensuring that devices conform to defined user needs and intended uses, and including testing of production units under actual or simulated conditions.
- Design transfer - Procedures to ensure that the device design is correctly translated into production specification.
- Design changes - Procedures for identifying, documenting, validating, and managing the verification and approval process of all design changes before they are implemented.
- Design history file - A design history file (DHF) is required for each type of device and should include or reference the records necessary to demonstrate that the design was developed in accordance with the approved design plan and device requirements.
Document controls (subpart D)
Medical device manufacturers are required to put in place document controls for all documents required in this regulation.
Document approval and distribution
One or more people must be assigned to review and approve documents prior to issuance. The approval must be documented, include a date and the signature of the approver, and be made available at all locations where applicable. Procedures must also be in place to ensure that obsolete documents are removed and/or prevented from being used.
Document changes
Similar to document approval procedures, changes to documents must be approved, reviewed, and documented. Records of all changes must be maintained.
Purchasing controls (subpart E)
To continue reading this Regulatory Brief, including a definition of the remaining subparts and a comparison of 21 CFR 820 to ISO 13485, please download the full brief.

Rimsys releases new automated unique device identification (UDI) module for its holistic medtech RIM platform
Rimsys, a world-leading Regulatory Information Management (RIM) software platform for medical technology companies, announced the release of an innovative and automated solution to address the global Unique Device Identification (UDI) requirements. This enhancement to the Rimsys ecosystem is immediately available to new and existing customers, providing a compliant method for tracking and traceability of UDI data that is fully compatible with global health authority databases.
UDI is a global harmonization effort to provide more consistent data that benefits overall product traceability throughout the medical device supply chain. It aims to adequately identify medical devices from manufacturing through distribution to patient use. Because global markets have different UDI requirements, product data can become a maintenance nightmare, even for the most mature medical technology companies. Data management is further complicated as UDI data is not static and must be updated based on changing regulatory requirements, such as market dates and registration status.
"Rimsys is the first automated UDI solution to fully integrate into a product’s registration lifecycle, ensuring that changing regulatory information is properly captured, registered, and maintained with the product and within government UDI databases like the GUDID (USA) and EUDAMED (EU)," said James Gianoutsos, Founder & President at Rimsys, "The current solutions landscape revolves around creating in-house, custom, and expensive projects with custom-built software or existing ERP software that were not designed to keep up with the fast-paced and ever-changing regulatory landscape."
In order to stay compliant and competitive, medical technology companies need to adapt quickly and flawlessly to the regulatory environment. As UDI requirements are rolled out across the globe, Rimsys’ UDI module seamlessly integrates with product registration data that is already actively managed within Rimsys, resulting in less maintenance, reduced costs, better compliance, and ultimately decreased time-to-market.
"We have already seen how our system has helped world-leading medical technology companies, such as Johnson & Johnson, Omron, and Terumo, digitize, automate, and navigate the global regulatory landscape,” said Brad Ryba, Chief Technology Officer at Rimsys, "As these requirements and demands continue to evolve, we are committed to ensuring that regulatory professionals can leverage the data integrations within Rimsys to more proactively manage their regulatory information."
Interested customers can schedule a preview of the new UDI module.

Rimsys named 2020 top technology company finalist by Tech 50 awards
Rimsys has been named a Finalist in Tech 50’s 2020 awards program hosted by the Pittsburgh Technology Council. The awards program, which was held November 12, 2020 at a virtual gala event, announced the winners and finalists. Rimsys was nominated as Innovator of the Year in the MedTech category, along with Sentact, Philips, and TeleTracking Technologies. In addition to the Company’s nomination, Rimsys’ Founder and CEO, James Gianoutsos, was nominated for CEO of the Year.
The awards program honors technology innovation in the region. Rimsys Inc., provider of the only holistic Regulatory Information Management (RIM) software for medtech is headquartered in Pittsburgh, Pennsylvania and was proud to be among the 2020 nominees. Rimsys was named a finalist this year, as Sentact, a provider of healthcare technology solutions for the patient care journey, walked away as the winner. Barbara VanKirk, CEO of IQ Inc., won this year’s CEO of the Year award.
"Rimsys is honored to be a finalist in both categories. Thank you to the Pittsburgh Technology Council for highlighting all of these innovative companies, and congratulations to this year’s winners," said Gianoutsos, "Rimsys is already used and trusted by leading companies, including Johnson & Johnson and Terumo, and we look forward to the near future where Rimsys’ automation of the global regulatory landscape is commonplace for medical technology companies and regulatory affairs professionals."
James Gianoutsos founded Rimsys in 2017, recognizing that while regulatory management platforms existed for pharmaceutical companies, medical technology companies face an entirely different set of challenges and requirements. Equipped with the expertise and drive to give regulatory affairs professionals a better way, he developed Rimsys: a RIM software built 100% for medtech companies.
Rimsys consolidates all the major functions of regulatory affairs on a 100% secure, cloud-based software, making product registration, standards management, essential principles/GSPR, and regulatory intelligence easy. Its newest integrated module manages global UDI requirements.
"It’s been an unparalleled year with unthinkable challenges," said Audrey Russo, President & CEO of the Pittsburgh Technology Council, "The COVID-19 Pandemic has tested everyone’s mettle in ways never imagined. This year’s Tech 50 is a testament to the fortitude, creativity, and innovation that exists across our industry, membership, and in every Tech 50 winner and finalist."
For a full list of finalists and winners, visit the Pittsburgh Technology Council’s website.
Rimsys secures $1.5 million to accelerate growth of its leading medtech regulatory information management platform
Rimsys Inc., provider of the leading Regulatory Information Management (“RIM”) software designed specifically for medical technology (“medtech”) companies, announced today it closed a $1.5 million investment round, led by Allos Ventures. The financing round will support Rimsys’ penetration of the medtech RIM market through planned expansions of its product offering, sales, and marketing execution. Rimsys serves an expanding list of enterprise customers, including industry leaders such as Johnson & Johnson and Terumo.
"Complex regulatory challenges create barriers that delay product time-to-market, stall revenue growth and increase exposure to compliance risks for even the most experienced medtech companies," said James Gianoutsos, founder & president of Rimsys. "Regulatory teams are in need of digital solutions that provide more efficient and compliant ways to stay on top of a constantly changing regulatory environment"
Rimsys’ solution seamlessly integrates with medtech manufacturers’ existing quality management systems, product lifecycle management systems, and sales and distribution software systems. Rimsys’ robust digital platform, with its intuitive user interface and global intelligence, enables its customers to meet market entrance requirements and grow internationally. John McIlwraith, managing director at Allos Ventures will join Rimsys’ board of directors.
"The maze of global regulations covering medical technology is growing more complex and frequently results in dead ends and delays that can greatly impact commercialization of these products," said McIlwraith. "This financing round will enable the company to further accelerate its momentum with large enterprise customers."
For more information on Rimsys, please visit www.rimsys.io.

Rimsys announces new brand identity for world-leading regulatory information management (RIM) software
Rimsys, a world-leading Regulatory Information Management (RIM) software platform for medical technology companies, announced a new brand identity and tagline. Rimsys, the only holistic RIM software on the market designed specifically for medical technology companies, with functionality for the pillars of regulatory affairs, rebranded to accurately reflect its novel and advanced offering through a distinct, modern brand identity and messaging platform.
The new visual identity, including logo, color palette, graphic elements, and iconography mirror the trusted, relatable, and modern personality of Rimsys. The colors, which feature a vibrant purple and dark blue, were strategically chosen to differentiate Rimsys from other RIM solutions on the market. The visuals are accompanied by a new mission statement, “to digitize, automate, and create regulatory order for the medical technology industry,” and messaging platform that conveys its value propositions:
- Used and trusted by the world’s leading medtech companies
- Built by and for regulatory affairs professionals in medtech
- Easy to start and simple to scale as your company grows
"We’re pleased to announce this rebrand to our customers and partners, with complete confidence that the new identity and messaging accurately reflect our enterprise software solution," said James Gianoutsos, Founder & President at Rimsys.
Rimsys consolidates all the major functions of regulatory affairs on a 100% secure, cloud-based software, making product registration, standards management, essential principles/GSPR, and regulatory intelligence easy. These functions, plus soon-to-be-released features, were formally messaged in the rebrand, including superior server security, system compliance, and simple integrations with many leading enterprise QMS and ERP/PLM software systems.
"With successful implementations in some of the world’s leading medical technology companies including Johnson & Johnson and Terumo, we already know Rimsys has the power to modernize medtech companies of all sizes and scales," said Gianoutsos. "And now, with a brand that mirrors our capabilities, we’re even better poised to reach out and help more."
Components of the rebrand can be seen on rimsys.io, and the full rebrand will be revealed on a new website that is currently under development.

Announcing the release of Rimsys 3.0: Rimsys Insight
Rimsys Regulatory Management Software, the leading and only Regulatory Information Management (RIM) system platform designed specifically for the medtech industry, has just released Rimsys 3.0, which includes its much anticipated regulatory intelligence module, Rimsys Insight.
Rimsys 3.0 now offers curated regulatory news along with changes to laws, regulations, and guidances that are timely and linked to customers’ specific products, markets and the other customizable filters available to each company. Additionally, the integration of market entrance requirements for the top 50+ global markets, further strengthen the already powerful Rimsys Registrations workflow which manages medical device and IVD registrations at the SKU level.
"Information is meaningless unless you can apply context to it as it relates to your company and products. As regulatory professionals ourselves, we know the specific pain that is experienced by our customers. The user experience should be seamless, fully integrated, and intuitive enough that, regardless of how long that person has been in the industry"
Rimsys was built for and by regulatory affairs professionals, enabling teams to digitize and automate otherwise disjointed, paper-based and manual processes. Rimsys has spent the last year working with customers from some of the world’s leading medical device manufacturers to develop the requirements that seamlessly integrate their business processes with its existing ecosystem of cloud-based regulatory affairs software solutions. This includes global product registrations, submissions management, standards management, essential principles and more.
"There’s simply no other holistic and vertically integrated solution quite like Rimsys out in the marketplace. Our initial features were focused on bringing MedTech companies together to collaborate and connect with each other internally. Built on this solid foundation, our latest release truly empowers and connects them to the entire global regulatory ecosystem"
Rimsys is a holistic approach to modernizing, digitizing and automating regulatory affairs activities for the MedTech industry by providing a single source of truth. Rimsys is now aligned and positioned to continue its growth and mission to "digitize, automate and createregulatory order for the medical technology industry™."

5 signs you are ready to take your medical device regulatory team digital
The medical device industry is in dire need of robust, practical and easy-to-use software to make regulatory professionals’ lives easier. Without a unified, collaborative, and regulatory digital system, serious consequences to a business can occur, including an increased risk of noncompliance, increased costs, and a significant reduction in a product’s revenue potential.
Here are the five biggest indicators that it’s time to take your medical device regulatory team digital.
1. You miss simple regulatory compliance requirements
Has your company missed an update to a standard? When a standard is updated that compliance is claimed for your products, a thorough review and associated gap analysis need to be conducted to determine if there is any impact to your products. You also need to go through every single essential requirements checklist to determine where that standard is referenced and update it throughout. If you miss those activities, you will most likely receive a finding when being audited that will require corrective action and significant resources to fix and ensure it doesn’t happen again.
Additionally, as the new Medical Device Single Audit Program (MDSAP) is rolled out, regulators from different markets are now working together to identify instances of noncompliance as well as misalignment of information in submissions and other communications.
MDSAP requires medical device manufacturers to produce evidence of marketing authorization for each country that they sell into. Your regulatory team needs automation to work for them in a way that creates safeguards to prevent unintentional release of products into markets.
There is a high need for more effective control of the submission process, enabled by a unified platform, which can lead to a leaner, higher quality submission and a reduced regulatory burden.
2. Your revenue is impacted
Are you missing registration dates, experiencing slow-to-market losses or long-term, cascading impacts such as loss of customer loyalty? All of these have an immediate and lasting impact on market capitalization.
If your marketing authorization lapses, your company legally cannot continue to sell within that country or market, guaranteeing your sales team becomes frustrated because they won’t hit their sales numbers and your company’s financial projections will be impacted.
Moreover, improper release of a product due to lack of visibility to regulatory statuses can cause fines and loss of credibility with authorities, which can result in increased scrutiny.
Based on a recent survey of 100 companies, 65% of regulatory professionals require at least a week to gather the information needed to determine where their products are sold and whether they are properly registered within a country or market.
If you can’t easily find the information, how effective and compliant can you really be? It may be time to take your regulatory team digital.
3. You miss your time-to-market targets
How do you organize and manage your regulatory information?
If you immediately thought of SharePoint, Excel, Word, Email, Outlook, or Dropbox, you probably aren’t working in the most efficient manner.
In fact, based on a Deloitte study, up to 50% of a regulatory team member’s time is wasted looking for information. Not only is your process inefficient but the way that you manage data and documents from a regulatory perspective is broken.
Based on FDA’s published data, 35% of all 510(k)s submitted to the FDA get stamped with Refuse to Accept (RTA) designation due to simple and avoidable mistakes.
Avoiding these needless delays in getting your products to market should be a top priority to ensure months or years are not added to getting your product the proper clearances.
4. You are burdened by administrative activities
Are you having trouble with efficiency, collaboration, and talent retention on your regulatory team?
Employee turnover on regulatory teams is linked to stress and increases greatly if team members consider processes to be inefficient or wasteful. Being able to perform one’s job efficiently and the perception of being part of a high-performing organization contributes to employee satisfaction and retention.
Regulatory processes touch multiple functional areas of a business in the highly regulated medical device industry. Regulatory teams have been piecing together disparate systems to achieve marginal improvement for years and are notoriously understaffed.
By giving them the right tools, so that they can do their jobs effectively and efficiently, should be priority number one.
5. You rely on institutionalized knowledge
Has a top member of your regulatory team left the organization, leaving you with no idea about what projects they had their hands in, the status of current submissions, broken down communications with external stakeholders, or lost critical tribal knowledge that wasn’t passed down?
Have you ever called that employee at their new company just to “pick-their-brain” because that critical information wasn’t transferred before they left?
Having a fail-safe in place now for when (not if) your top talent leaves prevents the loss of company and product specific tribal knowledge.
Bringing your regulatory processes into the digital age so your team and company can perform work within a central location ensures everything is properly documented and builds that critical archive of information. A unified system and collaboration hub keeps everyone on the same page within a single regulatory platform. Think of it as your company’s regulatory insurance policy.
Employees change roles, leave departments, and move on to other companies, leaving you to pick up the pieces. Retraining a new employee without the subject matter expert can cause delays and wasted time. So stop relying on disparate systems, disjointed processes, color-coded excel files, and emails that get lost in the shuffle and inhibit progress.
The good news
There is good news. Software solutions already exist that create a collaboration hub to help medical device companies actively navigate the changing regulatory landscape.
Software solutions such as Rimsys Regulatory Management Software can empower your current team. They provide better planning and tracking in a unified system that can monitor process metrics, milestones, and automatically inform submissions plan timelines with actual performance. A solution that connects planning to execution, allowing improved, real-time process monitoring provides teams visibility to quickly spot constraints and take action, allowing products to get through your regulatory process faster and with improved compliance.
It is time to set the new standard for the industry. It is time to go digital and start automating your broken systems.





