

Featured
Rimsys Announces Rimsys AI to Eliminate Repetitive Tasks and Enhance Decision-Making for MedTech Regulatory Teams
Rimsys, the leading Regulatory Information Management (RIM) platform for the MedTech industry, today announced the launch of Rimsys AI, a suite of embedded artificial intelligence (AI) agents.

The beginner's guide to the FDA 510(k)
This article is an excerpt from The beginner's guide to the 510(k) ebook.
Table of Contents
- Introduction
- 510(k) basics
- Contents of a Traditional 510(k)
- 510(k) submission and timelines
- Other 510(k) forms
Congratulations! You have successfully developed a new medical device. Now you need to take it to market. In the United States, this often means submitting a 510(k). A 510(k) is a structured package of information about your device and its performance and safety that you submit to the Food and Drug Administration (FDA) for “clearance” before you can sell your device in the U.S. In order to receive clearance from the FDA, your 510(k) will need to demonstrate that your medical device is substantially equivalent to another legally marketed device (called a predicate device). The substantial equivalence approval process is a simple equation that looks something like this:

The 510(k) is generally the most efficient route to market clearance in the U.S. because you show your device is safe and effective based on this substantial equivalence standard, instead of needing to present more extensive clinical trial data.
There are three types of 510(k): Traditional, Abbreviated, and Special. This eBook will begin with a general overview of the 510(k) process, including its purpose and benefits. Next, we will explore the Traditional 510(k) and the sections and components required in depth. Finally, we will look at the Special and Abbreviated 510(k).
FDA: background and device oversight
Before we explain what a 510(k) is let’s first talk generally about the FDA and device oversight. The FDA is the U.S. governmental agency responsible for overseeing medical devices, drugs, food, and tobacco products. When it comes to medical devices, the FDA’s mission is to “protect the public health by ensuring the safety, efficacy, and security of…medical devices.” At the same time, the FDA also has an interest in “advancing public health by helping to speed innovations.” In other words, the FDA’s goal is to make sure devices are safe and effective for public use, while also ensuring that devices have a quick and efficient path to market.
In order to achieve this balance of safety and efficiency, the FDA has three different levels of oversight depending on the risk level of the device: (1) exempt from premarket submission, (2) Premarket Notification, also known as 510(k), and (3) Premarket Approval (PMA).
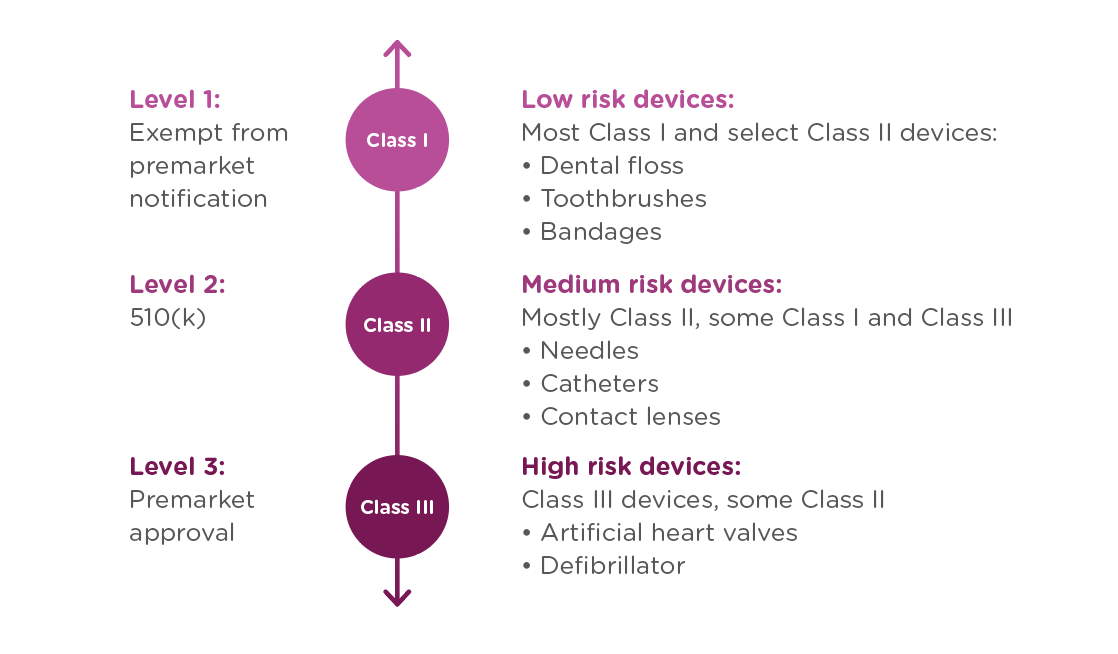
When is a 510(k) required?
A 510(k) is required for medium risk devices that have a predicate on the market which can be used to demonstrate the safety and effectiveness of the new device. Meanwhile, a PMA is required for high-risk or novel devices which require a higher level of scrutiny to be confirmed safe and effective.
A 510(k) is not only required for new devices, but also for devices that have been modified in a way that could impact safety or effectiveness. This could include changes to the:
- Design
- Components
- Materials
- Chemical composition
- Energy source
- Manufacturing process
- Intended use
You must submit your 510(k) at least 90 days before marketing the device.
What Exactly is Substantial Equivalence?
Now that we know what a 510(k) is, let’s talk about the substantial equivalence standard. You’ll recall from the introduction that your 510(k) must show that the new (or modified) device is substantially equivalent to at least one other legally marketed device, called a predicate device. Substantial equivalence looks at the intended use and the technological characteristics of the two devices.
More specifically, you must show:
- that the new device has the same intended use as the predicate, and
- the differences between the two devices do not raise questions about the safety and effectiveness of the new device.
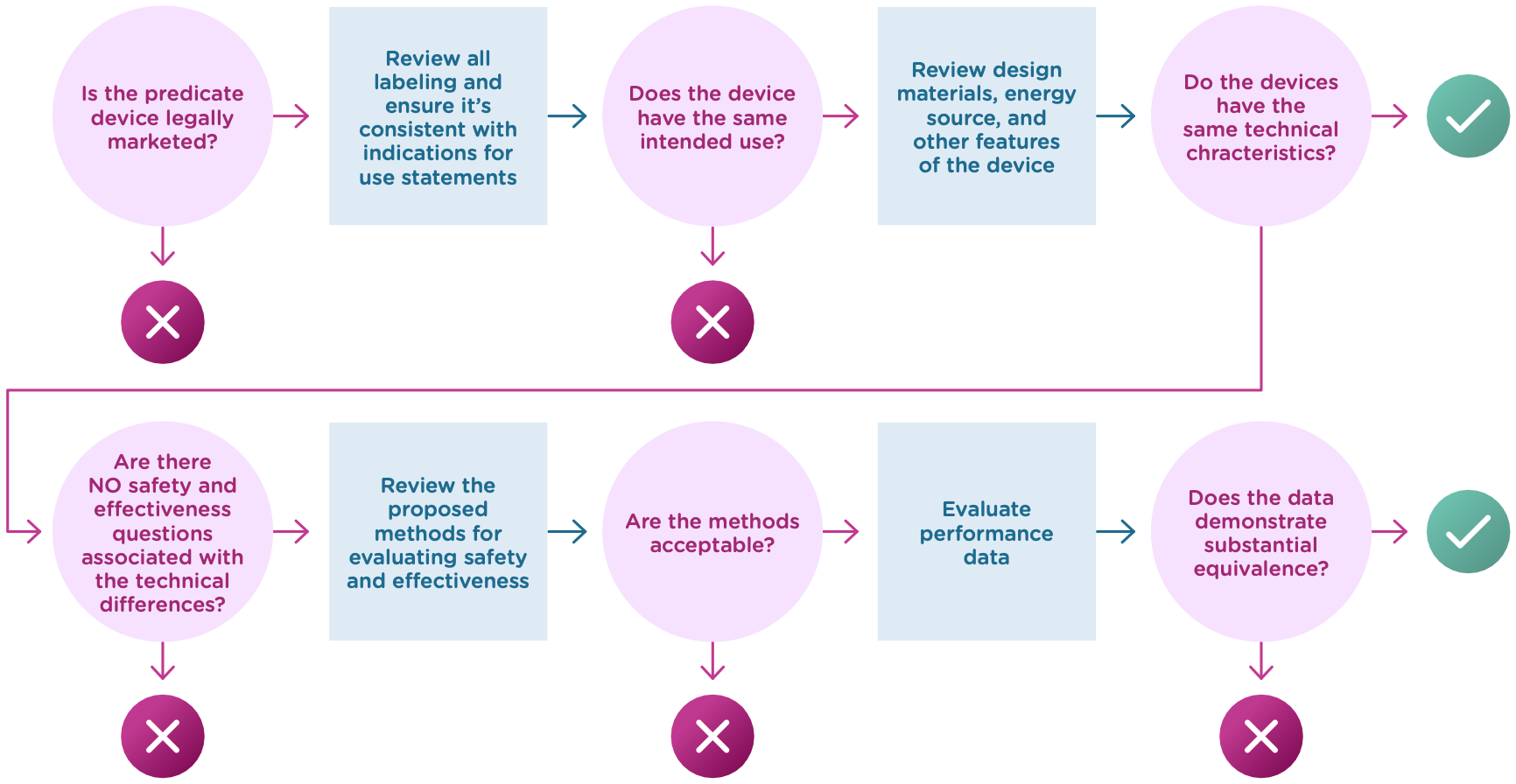
Now let’s take a closer look at intended use and technological characteristics.
Intended use
Intended use means the general purpose or function of the device. The FDA will look at your proposed labelling and your Indications of Use section of the 510(k) to determine the intended use of your device (this is covered in Chapter 2). Intended use includes:

Technological characteristics
Once the FDA has determined that a predicate device exists and that the new device and the predicate device have the same intended use, it will move on to compare the technological characteristics. Technological characteristics include:
- Materials
- Design
- Energy source
- Other device features
The two devices do not have to be identical, and in fact they almost never are. The key here is to demonstrate that any differences do not have a significant impact on safety or effectiveness. Here’s what to cover when you compare your device’s technological characteristics with that of the predicate device:
Overall description of the device design
- Engineering drawings or diagrams to explain the device and component parts.
- List of component parts and explanation of how each component contributes to the overall use and function of the device.
- Physical specifications: dimensions, weight, temperature, tolerances, etc.
Materials
- Detailed chemical formulation used in all materials of constructions (especially those that come into contact with a patient).
- Any additives, coatings, paint, or surface modifications.
- How materials have been processed and what state they’re in.
Energy Sources
- Use of batteries, electricity, etc.
Other technological features
- Software/hardware
- Features
- Density
- Porosity
- Degradation characteristics
- Nature of reagents
- Principle of the assay method
In deciding whether the differences in technological characteristics impact safety or effectiveness, the FDA will typically rely on descriptive information about the technological characteristics as well as non-clinical and clinical performance data.
Let’s look at an example: A manufacturer submits a 510(k) for a new type of contact lens. Both the new device and the predicate device are indicated for daily wear for the treatment of astigmatism. The predicate device is only available in a clear lens, but the new device comes in a line of colors, including purple tinted lenses.
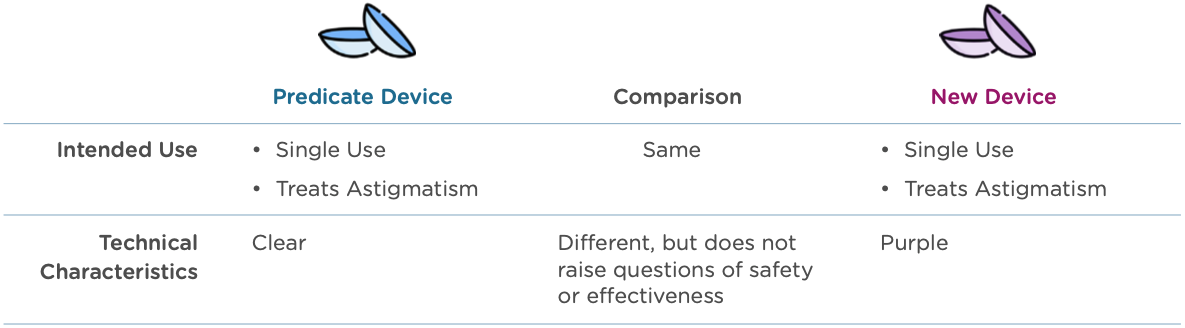

Who is responsible for submitting a 510(k)?
The following four types of organizations may be responsible for submitting a 510(k):
Manufacturers
- End-of-line device manufacturers who will be placing a device on the U.S. market.
- Note: Does not apply to component part manufacturers unless components will be marketed independently.
Specification developers
- Companies that develop the specifications for a finished device which has been manufactured elsewhere
Repackers or relabelers
- Required to submit a 510(k) if they significantly alter the labeling or condition of the device, including modification of manuals, changing the intended use, deleting or adding warnings, contraindications, sterilization status.
- Note: This is rare. The manufacturer, not the repackager or labeler, is typically responsible for the 510(k) submission.
Importers
- Importers that introduce a new device to the U.S. market may need to submit a 510(k), if it hasn’t already been submitted by the manufacturer.
Now that we’ve covered the basics, let’s explore what actually goes into your 510(k).
A Traditional 510(k) should contain all the following components in the list below. In some cases, a particular section may not apply to your device. When that happens, it’s a good idea to include the section anyway and just state “This section does not apply” or “N/A” under that heading.
To continue reading this eBook including a detailed walk-through of all the Traditional 510(k) components, submission requirements and timelines, and an overview of the other 510(k) forms including the Abbreviated 510(k) and the Special 510(k), please register to download the full version

The ultimate guide to the China UDI system and database
This article is an excerpt from The ultimate guide to the China NMPA UDI system and database ebook.
Table of Contents
- Overview
- UDI basics and benefits
- UDI format requirements and issuing entities
- UDI database and submission requirements
- Implementation of UDI and the UDI database in China
The current Chinese medical device regulatory regime kicked-off in 2014 with the Regulation on Supervision and Administration of Medical Devices. This core set of registration requirements, modeled after the United States and European Union systems, established a set of device classifications (class I, II, and III) based on risk and procedures for obtaining market clearance for each type of device.
Medical devices in China are regulated by the National Medical Products Administration (NMPA). Class I devices, such as clinical laboratory equipment or non-invasive skin dressings, require only notification to the NMPA for marketing authorization, and that authorization does not expire. Class II and III devices such as implantable devices or devices with a measuring function require full registration and a formal review before market clearance can be obtained.
These initial regulations have been expanded since their introduction, adding accelerated pathways to market for certain products in certain regions, easing acceptance of clinical data from overseas, and more specific roles and responsibilities for local agents of international manufacturers. In addition, in 2019, the regulations added a provision that medical devices carry a unique device identification (UDI). China’s UDI requirements are similar to those in the US and European Union. They establish specific device ID and labeling requirements, as well as a central, state-administered database of devices.
This eBook walks through the basics of medical device UDIs, the specifics of China’s implementation, and how MedTech companies who market their devices in China can prepare for the full rollout of these regulations in the coming years.
A UDI is a unique alphanumeric code that is designed to identify medical devices sold in a particular country/region from manufacturing, through distribution, to use by a patient. Like other aspects of the medical device regulatory regime, the UDI system in China follows the approach taken by the United States FDA and European Commission, and is based on the guidance from the International Medical Device Regulators Forum (IMDRF). Generally, UDI systems are designed to improve patient safety and optimize care by:
- Increasing the traceability of medical devices, including field safety corrective actions
- Providing an unambiguous identification method for medical devices throughout distribution and use
- Making adverse event reports more accessible
- Reducing medical errors by providing detailed information related to the device
- Simplifying medical device documentation and making it more consistent
There are three components to the UDI system in China:
- UDI code: The actual UDI code can be assigned by one of three (3) issuing agencies and contains information about the product, it’s expiration date, and the manufacturing batch/lot it’s associated with.
- UDI labeling: Put simply, medical devices must carry the UDI code on them. The regulations stipulate how devices and their packaging must be labeled for compliance.
- UDI database: In addition to labeling, all device UDIs must be submitted to a central database that is administered by the NMPA.
The following sections explore each of these components in more detail.
The UDI code
The first element of the UDI system is the code itself. The UDI code is the alphanumeric identifier that is associated with a specific medical device. UDI codes have two (2) elements to them, the UDI device identifier (UDI-DI) or static portion, and the UDI production identifier (UDI-PI) or dynamic portion. You can see the two components in the UDI diagram below:

The UDI-DI contains information about the issuing entity—the organization that is authorized to assign UDI codes. In China, this can be one of three entities: GS1, an international barcode and electronic data interchange standards organization, and two domestic organizations: the Zhongguancun Industry & Information Research Institute (ZIIOT), and AliHealth. Additional details about the issuing agencies are covered in Chapter 2. In addition, the UDI-DI contains information about the manufacturer and the specific model or version of the device.
The UDI-PI contains information about the manufacturing and production of the device. This typically includes information about the lot or batch number in which the device was manufactured, the manufacturing date and expiration date for the device (if applicable), and the specific serial number for the device. Here you can see all of the components marked up using the same UDI example:
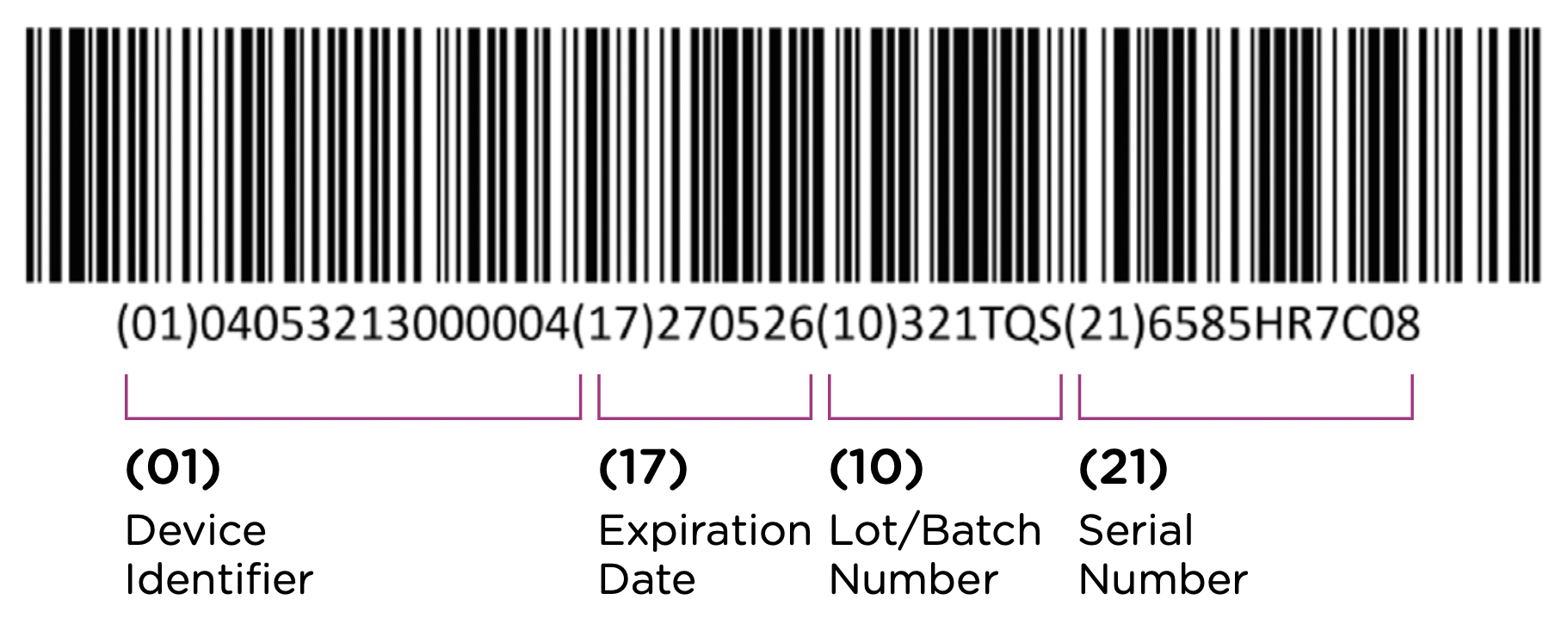
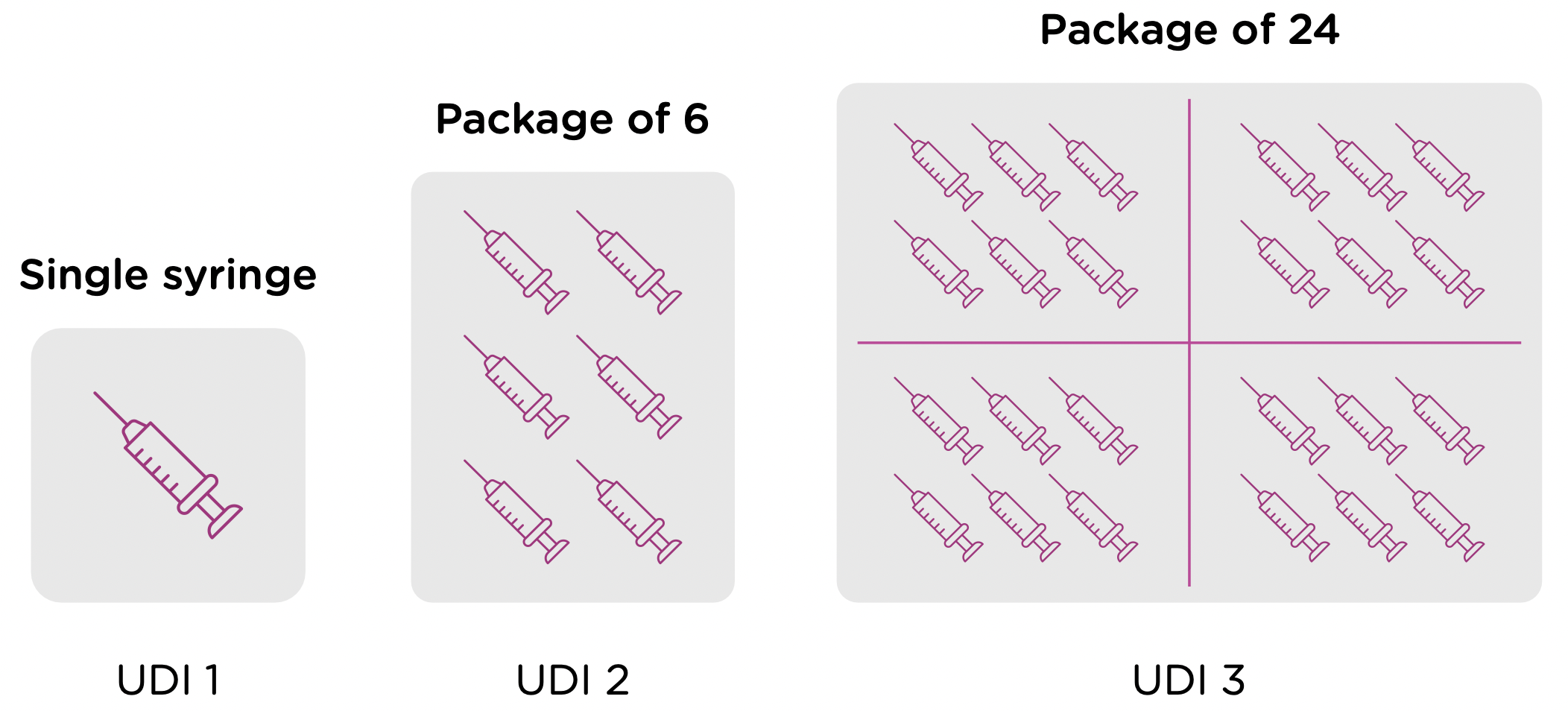
Note that each packaging permutation and level for a given device will need to be assigned its own UDI. So for example, let’s say that a company manufactures 5ml enteral (oral) syringes in two packaging options: 1 – packaged individually and 2 – packaged in a box of 5. Each packaging option would need its own UDI, despite the fact that the underlying product is the same.
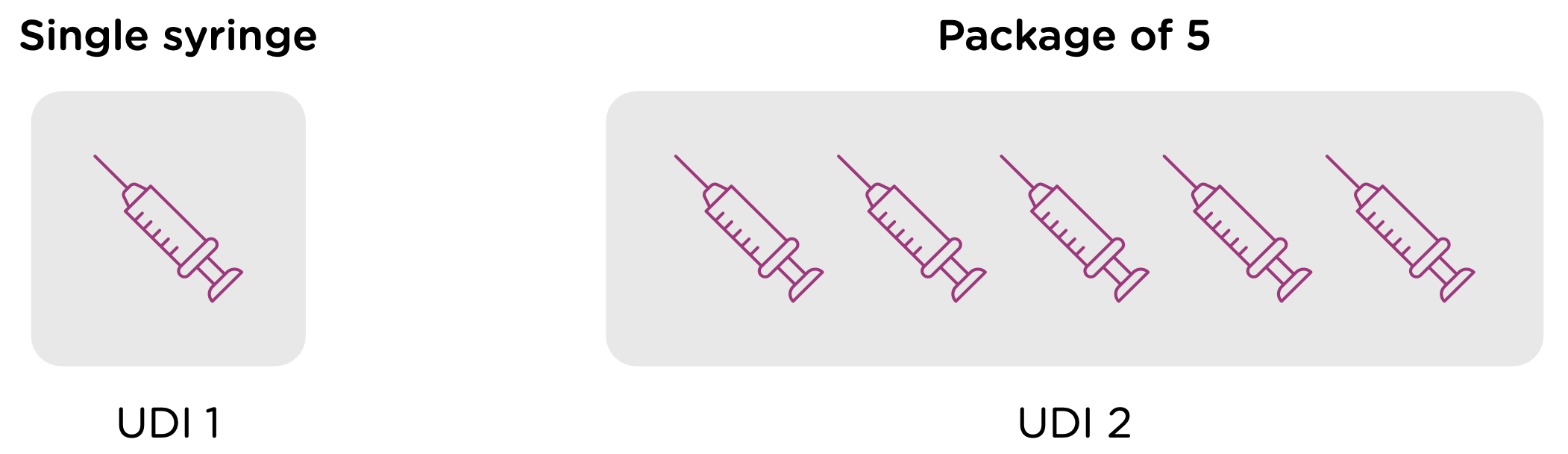
Now looking at packaging levels, let’s assume that the manufacturer packages the single syringe offering into boxes of 6, and again into larger containers of 24. Each of those packaging options needs its own UDI as well.
Labeling
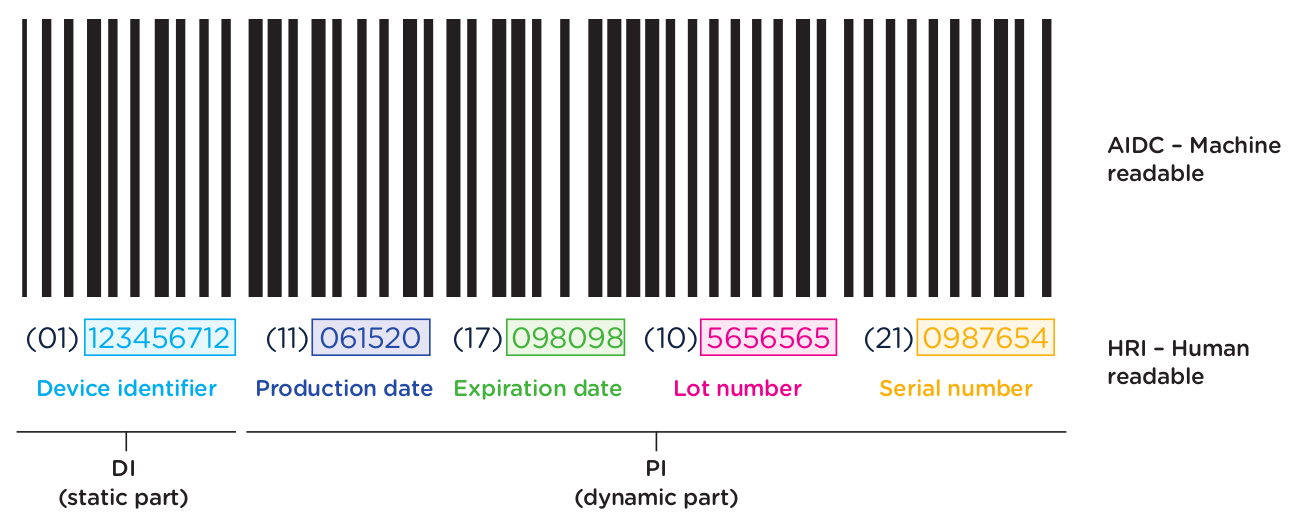
In addition to obtaining UDI code for each device as outlined in the previous section, medical device manufacturers are required to ensure that devices are appropriately labeled with the assigned UDI. This label is called the UDI Carrier. The UDI is represented in two forms on the UDI Carrier: a machine-readable form and a human-readable form.
The machine-readable form or automatic identification data capture (AIDC) is a barcode or some other technology that can be used to automatically capture UDI information. The NMPA regulations support 3 types of machine-readable formats: 1-dimensional barcode, 2-dimensional barcode, and radio-frequency identification (RFID).

The regulations note that “use of advanced automatic identification and data collection technologies is encouraged”—prompting manufacturers to use more modern 2D and RFID machine-readable carriers where possible. Note, however, that if a device uses RFID, the UDI Carrier must also include the UDI in barcode format.
The human-readable form or human-readable interpretation (HRI) is the numeric or alphanumeric code for the UDI that can be read and manually entered into systems.

The UDI Carrier should be included on the device and on all levels of packaging. The UDI Carrier must be clear and readable during the operation and use of devices. If there isn’t room on the device for both the human and machine-readable forms of the UDI, then manufacturers should prioritize the machine-readable form.
UDI database
The third component of the NMPA UDI system is the UDI database. This is a centralized database of UDI and product information, administered by the NMPA. Manufacturers are required to submit UDI information into the database within 60 days after a product is approved (for sale in China) and before it is commercialized. The database contains a more detailed product record than what is included in the UDI itself, and it is the responsibility of the manufacturer (and/or their in-country representative) to submit the information correctly, and ensure that it’s kept up to date.
Chapter 3 of this eBook goes into detail about the specific fields and data requirements for UDI database submissions.
To continue reading this eBook including information about UDI format requirements and issuing entities, implementation timelines, and affected device types, please register to download the full version.

The ultimate guide to the EU MDR/IVDR unique device identifier (UDI) System
This article is an excerpt from The ultimate guide to the EU MDR/IVDR UDI ebook.
Table of contents
- Overview
- UDI basics and benefits
- UDI format requirements and issuing entities
- UDI rules for specific device types
- Implementation of UDI and UDAMED in the European Union
- US vs EU UDI comparison
The EU Medical Device Regulation (2017/745) (“MDR”) and EU In Vitro Diagnosis Regulation (2017/746) (“IVDR”) introduce two new systems for information exchange: UDI (Unique Device Identifier) for device identification and EUDAMED (European Databank on Medical Devices) to centralize and disseminate information. UDI is a specific code assigned to all devices and higher levels of packaging. This will allow for devices being sold in the European market to be identified and traced through a globally harmonized approach. EUDAMED is the IT system developed by the European Commission to replace the EUDAMED2 database previously in place under the Medical Device Directives (MDD). EUDAMED is a multi-functional system that will be used to coordinate device registration, provide information about devices to industry professionals and the public, and highlight necessary safety details.
The EU MDR and IVDR UDI system is based upon the guidance of the International Medical Device Regulators Forum (IMDRF). It’s a globally harmonized system that’s designed to increase patient safety and optimize care.
UDI system goals
Increase patient safety
- Improve tracing of devices
- Reduce the presence of counterfeit devices
Ensure access to accurate information
- Unambiguous identification of devices throughout distribution and use
Improve post-market surveillance
- Improve accessibility of adverse event reports
Enhance supply chain Management
- Streamline supply chain process and inventory management
- Simplify medical device documentation processes
The UDI system has four key elements
Element 1: Assignment of UDI (UDI Components)
The first element of the UDI system is the assignment of a UDI. The UDI is a code of alphanumeric characters that acts as the access key to information about a specific medical device on the market. The EU MDR and EU IVDR requires that a UDI be assigned to all medical devices except for custom-made or investigational devices. There are three components of a UDI:
- Basic UDI-DI
- UDI (consisting of UDI-DI and UDI-PI)
- Packaging UDI (Note: This is not an official term used in the EU MDR and IVDR, but we’re using it to help explain the concept. The Packing UDI is part of the UDI itself.)
1. Basic UDI-DI
The Basic UDI-DI identifies the device group that a particular device fits into. A device group is a group of products that all share the same intended purpose, risk class, essential design, and manufacturing characteristics. A device group is generally classified by medical device manufacturers as a “Product Family” or “Product Category,” depending on the internal nomenclature used within the company. The Basic UDI-DI functions as a parent or higher-level descriptor of a device.
NOTE: There can only be one Basic UDI-DI per UDI-DI.
The Basic UDI-DI is not printed on the product itself or on the packaging of a product, but rather it must be included in the following documents and applications:
- Certificates (Including Certificate of Free Sale)
- EU Declarations of Conformity
- Techical Documentation
- Summary of Safety and Clinical Performance
2. UDI (UDI-DI and UDI-PI)
The second component is the UDI itself, which consists of two parts:
Device Identifier (DI)
Production Identifier (PI)
The UDI-DI (Device Identifier DI, also referred to as “static”) identifies specific, detailed information about a particular device. If any of the below details should change, the device will need a new UDI-DI.
- Name or trade name of the device
- Device version or model
- If labelled as a single use device
- Packaged as sterile
- Maximum number of uses
- Need for sterilization before use
- Quantity of devices provided in a package
- Critical warnings or contra-indication
- CMR/endocrine disruptors
NOTE: There can be several UDI-DIs for one Basic UDI-DI.
Meanwhile, the UDI-PI (Production Identifier PI, also referred to as "dynamic") contains manufacturing information (including serial number, lot/batch number, software identification, and manufacturing or expiry date or both types of dates.)
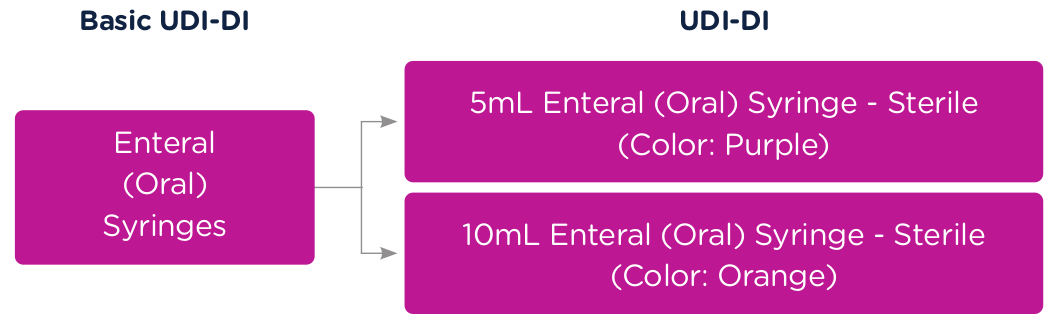
To better illustrate this concept of Basic UDI-DI and UDI (UDI-DI and UDI-PI), let’s use a syringe as an example. The Basic UDI-DI would identify the category of a syringe, for example, "Enteral (Oral) Syringe."
A 5ml Enteral (Oral) Syringe – Sterile (Color: Purple) would get a unique UDI-DI and a 10m Enteral (Oral) Syringe – Sterile (Color: Orange) would get a unique UDI-DI. Both products would be associated to the same Basic UDI-DI. In this case, the "Enteral (Oral) Syringe," which defines the category.
Each time that 5ml Enteral (Oral) Syringe – Sterile (Color: Purple) is manufactured at the same revision, it will get a new UDI-PI per lot. See the graphic below.

Each product is identical and therefore has the same UDI-DI. However, the UDI-PI changes to reflect the manufacturing date, lot number, expiry date, and serial number, as applicable.
The UDI will contain all device-specific information and have the same functions as the comparable database (GUDID) of the United States FDA. The main difference (in EUDAMED) is that the UDI data is divided into components of Basic UDI-DI, UDI, and Packaging UDI.
3. Packaging UDI
The third component of UDI is the Packaging UDI. (Note: This is not an official term used in the EU MDR and IVDR, but we’re using it to help explain the concept.)
Each level of packaging, except shipping containers, must receive its own unique UDI. Packaging UDI refers to the unique UDI assigned to higher levels of packaging instead of the device itself.
In the event of significant space constraints on the unit of use packaging, the UDI Carrier may be placed on the next higher packaging level.
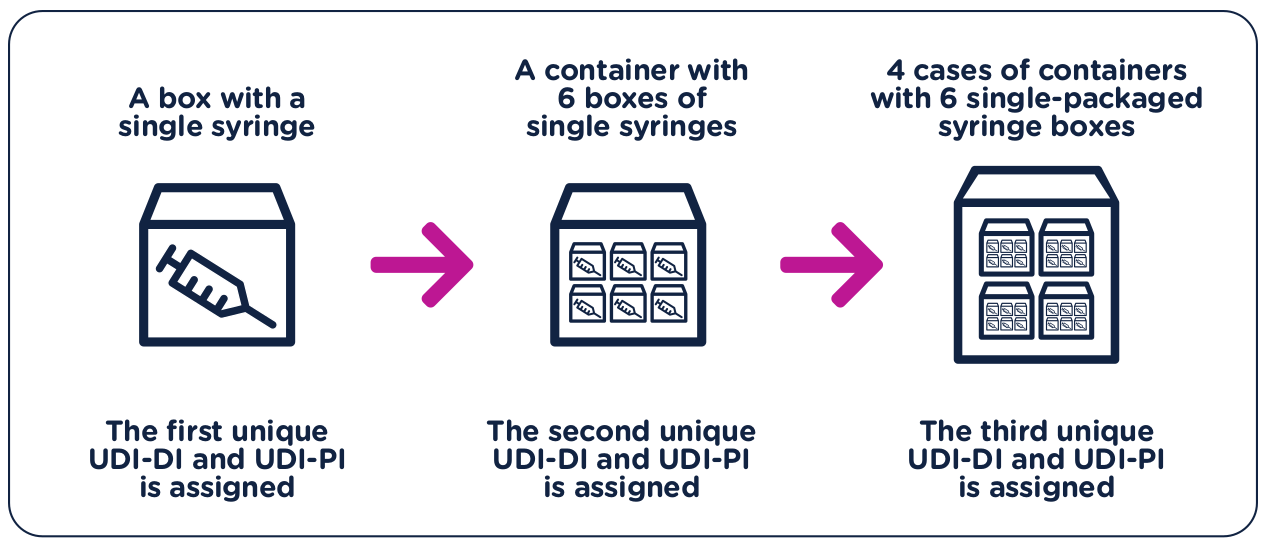
Returning to our earlier example of syringes, if a manufacturer first packages a single sellable syringe into an individual box, this package would receive its own UDI-DI and UDI-PI.
If then the manufacturer packages those individual boxes into containers of six (6), those containers would receive their own UDI-DI and UDI-PI.
And finally, if the manufacturer packages those six (6) containers into cases of four (4), those cases would receive their own UDI-DI and UDI-PI.
Each of those levels of packaging must be assigned its own UDI-DI and UDI-PI. The initial syringe did not change, but the way it is packaged did, therefore, requiring its own UDI-DI and UDI-PI.
Element 2: Placing UDI on the device and/or packaging
The second element to the UDI system is the placing of the UDI on the device or on its packaging through what is referred to as a “UDI Carrier.” The UDI Carrier is the part of the label that contains the UDI information that is applied directly to the device or included on the device packaging. The UDI Carrier should have both a machine-readable portion (AIDC) and a human-readable portion (HRI). (Specific details about each element of the UDI will be covered in Chapter 2.)
- Machine-readable form – AIDC – (Automatic Identification and Data Capture) is a barcode or other machine-readable technology that can be accessed automatically by scanning the UDI information.
- Human-readable form – HRI – (Human Readable Interpretation) is the numeric or alphanumeric code, which can be manually entered into the system for access to the UDI information.
If there are space constraints limiting the use of both the AIDC and HRI on the label, then only the AIDC is required to appear. However, on devices that are intended to be used in home-health care or other non-medical facility settings, the HRI would be required to appear.
Single-use devices may contain the UDI Carrier on its lowest level of packaging rather than on the device itself.
Reusable devices must include the UDI Carrier on the device itself, unless any type of direct marking would interfere with the safety or performance of the device, or if it is not technologically feasible to directly mark the device. If so, this should be properly documented in your design history file.
Most importantly, the UDI Carrier must be readable for the intended lifecycle of the device.
Below is an example of a GS1 AIDC and HRI barcode label.
Element 3: Storage of UDI information by Economic Operators
Storage of UDI information by "Economic Operators" is the third element of the UDI system. 2017/745 Articles 2(35), 22(1), and 22(3) define an economic operator as:
- A manufacturer
- An authorized representative
- A distributor
- An importer
- An investigator for clinical investigations
- A person who sterilizes systems or procedure packs
Class III, implantable device:
According to EU MDR 2017/745 Annex II, the manufacturer shall keep an updated list of all UDIs that it has assigned. Economic operators and all health institutions are required to store, preferably by electronic means, the UDI of all the devices for which they have supplied or with which they have been supplied.
For Devices Other than Class III:
Member States are encouraged, and in some cases require, health institutions to store, preferably by electronic means, the UDI of the devices with which they have been supplied. The UDI must also be included in any field safety notice for reporting serious incidents and field safety corrective actions.
The EU MDR and EU IVDR also give the European Commission authority to make additional requirements regarding the submission or maintenance of UDI information. In making those decisions, the European Commission must consider six (6) areas:
- Confidentiality and data protection
- Risk-based approach
- Cost-effectiveness of the additional measures
- The need to avoid duplications in the UDI system
- The needs of the healthcare systems of the member states
- Harmonization with other medical device identification systems
To continue reading this eBook including information about the EUDAMED database, UDI format requirements and issuing entities, implementation timelines, and key differences between the EU and US UDI systems, please register to download the full version

Taking SaMDs to market in the US: How is the FDA regulating adaptive machine learning algorithms?
Rimsys recently held a panel discussion, Taking SaMDs to market in the US. During it, Prabhu Raghavan, Principal at MDQR Solutions, and Rimsys Chief Solutions Officer, Brad Ryba, shared an overview of SaMDs and provided their insights about getting and maintaining market clearance for them in the United States. Topics ranged from FDA risk classifications and submissions, cybersecurity best practices, and machine learning algorithms, which brought about an important question: How is the FDA currently regulating adaptive machine learning algorithms in SaMDS?
Adaptive machine learning algorithms use post-market data in real time and evolve their models based on the data they're consuming. As such, every patient utilizing a device with adaptive machine learning algorithms may have a new model compared to the previous patient. While the FDA doesn't have any formal guidance on the subject just yet, manufacturers can work with the FDA to get a plan in place for maintaining a state of validation post market.
Watch the snippet from the webinar to learn about taking a staged approach with the FDA to get a proper validation plan in place.
To watch all discussion topics, download the webinar replay here.

The five guiding principles for machine learning-enabled medical devices using PCCPs
On October 24th, 2023, the FDA, Health Canada, and the MHRA published a joint document providing harmonization for machine learning-enabled medical devices (MLMD) that use predetermined change control plans (PCCPs). PCCPs are plans proposed by the manufacturer that state the specific modifications to a MLMD, the process for implementing these modifications, and the assessment of impacts from them.
The document details five guiding principles for MLMDs in an effort to set a foundation for PCCPs and encourage collaboration on them. According to the UK government’s website, these principles are:
- Focused and Bounded: Describing specific changes that a manufacturer intends to implement.
- Risk-based: The intent, design, and implementation of a PCCP are driven by a risk-based approach that adheres to the principles of risk management.
- Evidence-based: Demonstrating that benefits outweigh the risks throughout the product lifecycle.
- Transparent: Provide clear and appropriate information and detailed plans for ongoing transparency to all stakeholders, from patients to healthcare professionals.
- Total Product Lifecycle Perspective: Improve the quality and integrity of a PCCP by continually considering the perspectives of all stakeholders.
Here are some examples of how these principles could be applied:
- Focused and bounded: A manufacturer of an MLMD that diagnoses cancer might develop a PCCP to implement a change to the algorithm that improves its accuracy in detecting a specific type of cancer.
- Risk-based: A manufacturer of an MLMD that monitors a patient's vital signs might develop a PCCP to implement a change to the algorithm that reduces the likelihood of false alarms.
- Evidence-based: A manufacturer of an MLMD that delivers medication to patients might develop a PCCP to implement a change to the algorithm that improves the accuracy of the dosage.
- Transparent: A manufacturer of an MLMD might publish a white paper that describes the device's algorithm and how it was developed and tested. The manufacturer might also make available a user manual that provides clear instructions on how to use the device safely and effectively.
- Total product lifecycle perspective: A manufacturer of an MLMD might collect feedback from patients and healthcare professionals on how the device is performing after it is marketed. The manufacturer might also use this feedback to identify and address any potential problems with the device.
The five guiding principles for MLMDs using PCCPs are based on the 10 guiding principles for Good Machine Learning Practices (GMLP) published in 2021, which were designed to help medical device manufacturers develop and deploy machine learning models that are safe, effective, and high quality. Similarly, the goal of these five guiding principles is to help MLMD manufacturers develop and maintain safe and effective products that meet the needs of patients and healthcare professionals. They are also intended to streamline the regulatory process for MLMDs, making it easier for manufacturers to bring new products to market and make updates to existing products in a timely manner.
If you’re looking for additional information about MLMD requirements in the US, join Rimsys and MDQR Solutions for Taking SaMDs to market in the US on Thursday, November 30th, at 1 PM ET. We’ll discuss the various types of SaMDs, considerations to make when obtaining market clearance, and how the FDA is regulating AI/ML in devices. Those interested in attending can register here: Taking SaMDs to market in the US.

An overview of the Accreditation Scheme for Conformity Assessment (ASCA) Program
Introduced in 2021, the Accreditation Scheme for Conformity Assessment (ASCA) program is a voluntary program that allows device manufacturers to use an ASCA-accredited testing laboratory to conduct testing to be included in premarket submissions to the FDA. The ASCA program is designed to speed up FDA review times, reduce guesswork on documentation to provide in a premarket submission, and improve the quality of testing conducted.
In September of 2023, the program was converted from a pilot to a permanent volunteer program. This blog post provides an overview of the ASCA program to help medtech companies determine if they should consider participating.
How the ASCA program works
Under the ASCA program, the FDA grants ASCA Recognition to qualified accreditation bodies, which certifies testing laboratories to perform premarket testing for medical device companies. The FDA uses international conformity assessment standards and FDA-identified ASCA program specifications to assess ASCA Accreditation status to qualified testing laboratories.
The ASCA program includes FDA-recognized consensus standards and related test methods across two scopes:
- Biocompatibility: This scope includes standards for testing the safety of medical devices when they come into contact with human tissues.
- Basic safety and essential performance: This scope includes standards for testing the safety and performance of medical devices.
It’s important to note that medical device manufacturers should continue to reference additional FDA-recognized standards and provide declarations of conformity in their premarket submissions, but standards outside of biocompatibility and basic safety and essential performance are not eligible for ASCA program benefits.
Medical device manufacturers can choose an ASCA-accredited laboratory to conduct its testing for FDA premarket submissions. The ASCA-accredited testing laboratory will provide the manufacturer with all information listed in the ASCA program specifications.
For each eligible FDA-recognized consensus standard and test method, the manufacturer will need to document results on an ASCA Summary Test Report. Upon testing completion, the device manufacturer will receive an ASCA Summary Test Report from the laboratory. When the manufacturer prepares their premarket submission for FDA approval, they will need to include a declaration of conformity with the ASCA Summary Test Report as part of their submission.
Benefits of participating in the ASCA program
Medical device companies that participate in the ASCA program can see a variety of benefits, including:
- Faster FDA review times: The FDA has stated that it expects to review premarket submissions that include ASCA Summary Test Reports more quickly than submissions that do not.
- More clarity on documentation needed in a premarket submission: The ASCA Summary Test Report template provides a guide on what information to include in the report, which can help device manufacturers avoid having to guess what the FDA is looking for. This can save time and resources and help to ensure that the premarket submission is complete and accurate.
- Improved quality of testing conducted: ASCA-accredited testing laboratories must meet rigorous standards for competence and impartiality.
- Enhanced credibility: Participating in the ASCA program can help device manufacturers enhance their credibility with the FDA and other stakeholders. This is because the ASCA program is designed to improve the quality and efficiency of the premarket review process.
While the FDA has not announced any plans to make the ASCA program mandatory, it has stated that it intends to review premarket submissions that include an ASCA Test Summary report faster. This means that device manufacturers who participate in the ASCA program may be more likely to receive faster approvals.
In addition, some countries outside of the United States require device manufacturers to use accredited testing laboratories for premarket approval. By participating in the ASCA program, device manufacturers can demonstrate that their testing is conducted to high standards and more easily meet the requirements of these countries.
Funded through the MDUFA V User Fee program, the FDA does not charge an additional fee for manufacturers to participate in the ASCA program. For more guidance and training on the ASCA program, see the FDA’s website.

Your eSTAR submission questions answered by FDA experts
Your eSTAR submission questions answered
Starting on October 1, 2023, all 510(k) submissions, unless exempted, will need to be submitted electronically using eSTAR. eSTAR, which is short for Electronic Submission Template and Resource, is a dynamic PDF submission template that contains automation, guides, integrated databases, integrated policies and procedures, and automatic verification to help users prepare a comprehensive medical device submission.
Rimsys recently hosted a webinar, eSTAR submissions overview and live Q&A with FDA, to help the medtech community prepare for the quickly approaching eSTAR deadline. Patrick Axtell, Assistant Director for Tools and Templates Team, and Sajjad Syed, Software Engineer for Tools and Templates Team, from FDA joined our panel of Rimsys regulatory experts to provide an overview of eSTAR, demo, and live question and answer session. If you're interested in watching the webinar replay, you can find it here.
Due to high participation, we couldn't answer all questions live. This blog post provides Patrick's and Sajjad's answers to questions we couldn't get to during the webinar. Read below to learn what other industry professionals want to know about eSTAR!
Q: In the past, the sections were numbered Section 10 - Device Description. How should section(s) be numbered in the eSTAR?
You may number attachments how you prefer, this includes numbering attachments according to the previous section numbers of the Format for Traditional and Abbreviated guidance document. However, the numbering hierarchy in the IMDRF documents, which the attachment questions in eSTAR correlate to, may be better, since that numbering scheme is internationally harmonized. So for example, if you are using the nIVD eSTAR, the IMDRF document specifies the Comprehensive Device Description would be numbered 2.04.01: https://www.imdrf.org/sites/default/files/docs/imdrf/final/technical/imdrf-tech-190321-nivd-dma-toc-n9.pdf.
Q: After October 1, 2023, will the In Vitro Diagnostics eSTAR Version be acceptable to use for a Dual 510(k) and CLIA Waiver by Application (Dual Submission)?
Yes, the next IVD eSTAR update will fully support Dual submissions, and the workaround we were previously implementing will no longer be needed. CLIA waiver submissions will continue to be submitted via current methods, and are not required to use eSTAR after Oct 1, 2023.
Q. It is not possible to view eSTAR online from cloud storage platforms. eSTAR like IFU Form and CDRH Form cannot be viewed online without users downloading these files. I will highly appreciate if someone from the panel can give a solution to this. I understand these are special pre-programmed PDFs but it will immensely help if these can be shared for online viewing without having users download these files.
You need to choose to open eSTAR in the default application from within the cloud application you use, you can’t just click on it, since it will open in the browser, and browsers can’t open dynamic PDFs like eSTAR, Form 3881, Form 3514, and other forms FDA uses.
We can’t say that all cloud applications will work, but using Box does work. Once eSTAR is loaded in, click on the three dots, then choose the application you have installed, see screenshots below. I have Adobe Acrobat 2017 and Adobe Acrobat Pro both installed.
Be aware that every time you save the form, you upload it back into the cloud, so depending on how large it is and how fast your internet connection is, it may take many seconds to save each time, though you will see a progress bar.
Q: Does the eSTAR submission need to be submitted by only the US Agent or can this be done by the Foreign Manufacturer?
510(k) eSTARs, like 510(k) eCopies, can be submitted by foreign applicants.
Q: Will it be mandatory to use the eStar template for PMA supplement submissions?
Yes, by the end of 2023, eSTAR for PMA will be released. Similar to eSTAR for 510(k), there will be a pilot, guidance, and a transition period before it becomes mandatory.
Q: When do you expect to release the next version or sub-version of the non-IVD eSTAR template (4.x or 5.0) and will it be more elaborate on cybersecurity?
We are at the mercy of updating when policies are updated, which is irregular and unpredictable. Please email CDRH management and recommend a more consistent (e.g. quarterly) policy deployment schedule so that eSTAR can also have a more predictable deployment schedule. We are updating approximately one to every two months currently. Please be sure to read the Version History on page 1 of eSTAR regarding versioning and which version to use.
Q: How should a device categorized as a breathing gas pathway device in accordance with ISO 18562 be handled in eSTAR? One cannot find ISO 18562 categorization for a device in the eSTAR form.
This is a regulatory and policy question, and we are not sure what is meant by the statement “be handled.” Please reach out to OPEQ Submission Support OPEQSubmissionSupport@fda.hhs.gov with this question and they will direct your question appropriately.
Q: How often does FDA anticipate revising the eSTAR form?
eSTAR updates are almost exclusively timed according to policy updates, which the Tools and Templates Team has no control over. The T&T Team, as well as other groups in CDRH, are pushing for a quarterly update, where any policy updates in a quarter have an implementation date set for the beginning of the next quarter (e.g. Oct 1st, Jan 1st, Apr 1st). Please email Center management and promote this.
Q: The guidance Format for Traditional and Abbreviated 510(k)s: Guidance for Industry and FDA staff recommends a specific format for submissions. Biocompatibility, for example, is section 15. Should attachments in the eSTAR submission cross-reference the sections cited in the guidance? (So still using biocompatibility as an example, attachment 15.1 would be Cytotoxicity, attachment 15.2 would be Sensitization and so on)
The Format guidance, as well as the eCopy guidance, RTA guidance, and many other guidances, no longer apply for eSTARs. Eliminating the applicability of guidances - simplifying the preparation process - is something we are proud of doing. You do not need to follow the numbering of this guidance. See response above, where we recommend using the IMDRF numbering scheme instead, which is internationally harmonized.
Q: Where is information for risk assessments and management best included?
Depending on the type of submission you have selected (e.g. 510(k), De Novo, then Traditional, Special, Abbreviated), certain sections will become visible and active and some of them will be disabled. However, the bookmark pane will show all the sections in the entire eSTAR. Hence, please fill the sections that are visible to you since they are based on your selections. For example, if you have selected a Traditional 510k, the “Benefits, Risks and Mitigation Measures” section is not applicable. Hence it is not displayed and clicking on it leads a user back to the first page of the eSTAR. However, if you select “Special” as the 510k you are submitting, the “Benefits, Risks and Mitigation Measures” section does become applicable, and is displayed if you click on the bookmark. Also note that if you select De Novo, the section does become active as well. Another point to note is that for a Traditional 510(k) submission, if you do want to submit a Risks, Mitigations, Benefits report, you can attach it in the Performance Testing --> Bench Testing section of the eSTAR and identify it as “Other Non-Clinical Evidence”.
Q: Under Biocompatibility any idea when there will be endpoint questions for hemocompatibility or coagulation?
Hemocompatibility endpoint information, including Hemolysis, Complement Activation, and Thrombogenicity information, will appear depending on the tissue contact type and duration you choose. If you choose Implant Device >30 days, you will see this tab appear for example. The tabs that show are based on our Biocompatibility guidance.
Q: Guidance and Special Controls Adherence Section: According to the 510(k) electronic submission guidance document, identification of any applicable device-specific guidance documents or special controls should be included, which was done in the past; however, eSTAR requires each specific special control regulation or guidance recommendation to be listed. Can you please specify to what level of detail needs to be included within this section? The text box contains a character limitation, so it is unclear how specific information needs to be.
There are four textboxes like this in eSTAR. The specifications, characteristics, etc., of the device should not be provided in these textboxes. Instead, these textboxes should be used to refer to the attachments where these controls or recommendations are found, per each specific recommendation. These textboxes do expand as text is typed in, if needed. Keep in mind that the special controls, device-specific guidance citations would be divided among these four textboxes.
Q: Why are Advertisements included within the Labeling section, when they should be considered promotional materials? Could reference to advertisements be removed from this section?
Advertisements and promotional materials are included under the Other Labeling, and within the sub-attachment type "Other Labeling and promotional material" since this is consistent with Internationally harmonized document N9 and N13. As the help text states, whether you actually need to attach it at all (it is an optional attachment) is dependent on the jurisdiction. For FDA, you would need to reach out regarding your device and current policy at opeqsubmissionsupport@fda.hhs.gov.
Q: I need to know how eSTAR would promote efficiency.
There are many efficiency gains with eSTAR, this is not an exhaustive list. The eSTAR website also includes some of this information.
-eSTAR complements the reviewer's internal smart review template used to review the submission (i.e. the questions correlate). Therefore the reviewer is getting what they are expecting
-eSTAR provides a standardized format so that the reviewer (and applicant) always know where to find certain information
-eSTAR auto-updates many aspects of the submission, most notably it ensures the content is present negating the need for an RTA review by the reviewer, and therefore RTA holds
-eSTAR autocompletes information that you enter, ensuring you never need to enter the same information twice
-eSTAR includes built-in databases that ensure you see the information pertinent to your device (e.g. device-specific guidances), classification information automation, and the standards database, for auto-filling standards info accurately
-eSTAR has many forms built in, so that you don’t need to attach or upload them (e.g. T&A statement, Form 3514, 510(k) Summary, Declaration of Conformity, Form 3881)
-eSTAR guides the applicant through what is needed throughout, ensuring we collect everything that needs to be provided, and you know how to do it correctly
-eSTAR is collecting submission data in a structured format, which will help automate many aspects of our processing. This will provide applicants and reviewers many benefits (e.g. automating the submission log-in process, therefore permitting reviewers to receive a submission within minutes of when the submission is uploaded in the CDRH Portal)
-eSTAR is intended to be used as a resource also, since it consolidates all the information needed (e.g., regulation links, guidance links, submission process information) to prepare a submission

Rimsys ranks number 156 on the 2023 Inc. 5000
Rimsys is happy to announce today that it has been ranked number 156 on the 2023 Inc. 5000 list of fastest-growing private companies in America. Companies on the 2023 Inc. 5000 are ranked by their percentage of revenue growth over a three-year period. With exponential growth over the past three years, Rimsys joins a prestigious list of organizations across the country.
Rimsys, a cloud-based software for end-to-end regulatory process digitization and automation, is designed by and for medtech regulatory affairs professionals who experienced the painful challenges and compliance risks that result from not having a centralized, collaborative hub for regulatory information.
"Being included on this year's Inc. 5000 list of fastest-growing private companies is a tremendous milestone for Rimsys," said James Gianoutsos, Founder and CEO. "I created Rimsys to help medical device manufacturers overcome the challenges I experienced in the industry, and our regulatory information management (RIM) platform has increasingly gained the trust of leading medical device manufacturers globally over the past few years. I'm excited to continue our mission of improving global health by accelerating delivery and increasing availability of life-changing medical technologies with the support of our team members, customers, and partners."
The top 500 companies, including Rimsys, are featured in the September issue of Inc. Magazine, which will be available beginning August 23. To see the complete results of the Inc. 5000, view company profiles, and access an interactive database of honorees, visit www.inc.com/inc5000.
About Rimsys
Rimsys is improving global health by accelerating delivery and increasing availability of life-changing medical technologies. Rimsys Regulatory Information Management (RIM) software digitizes and automates regulatory activities, helping medtech regulatory affairs teams to plan more effectively, execute more quickly, and confidently ensure global regulatory compliance. Unlike complex, color-coded spreadsheets, or expensive external consultants, Rimsys centralizes all regulatory information, automates submission processes, and provides detailed visibility into product registrations, expirations, relevant standards, and global regulations. Traditional approaches to regulatory affairs can’t keep pace with the growing complexity of the global landscape, and overburdened teams face increasing compliance risks. Rimsys is designed around medtech regulations and workflows and supports a full breadth of regulatory activities including registrations, submissions, UDI, essential principles, standards management, and regulatory intelligence in a single, integrated platform. Leading global medtech companies including Johnson & Johnson, Siemens Healthineers, and Omron rely on Rimsys to better manage regulatory projects and resources, get new products to market more quickly, and reduce revenue risk of non-compliance, product recalls, and unexpected expirations. For more information, visit www.rimsys.io.
About Inc.
Inc. Business Media is the leading multimedia brand for entrepreneurs. Through its journalism, Inc. aims to inform, educate, and elevate the profile of our community: the risk-takers, the innovators, and the ultra-driven go-getters who are creating our future. Inc.’s award-winning work reaches more than 50 million people across a variety of channels, including events, print, digital, video, podcasts, newsletters, and social media. Its proprietary Inc. 5000 list, produced every year since 1982, analyzes company data to rank the fastest-growing privately held businesses in the United States. The recognition that comes with inclusion on this and other prestigious Inc. lists, such as Female Founders and Power Partners, gives the founders of top businesses the opportunity to engage with an exclusive community of their peers, and credibility that helps them drive sales and recruit talent. For more information, visit www.inc.com.

An overview of the Medical Device Discovery Appraisal Program (MDDAP)
Regulatory affairs within the medtech industry is uniquely challenging. Teams are faced with external changes in the form of new regulations (such as the MDR/IVDR in the European Union), growing information needs (including expanding unique device identification requirements around the world), newer audit requirements (MDSAP), and post-market surveillance requirements.
While there are emerging technologies that can help teams better address these issues, building more effective and efficient regulatory teams requires more than better tools. The traditional, largely manual approach to regulatory procedures and processes must also evolve, including the measurement of regulatory maturity. The Medical Device Discovery Appraisal Program (MDDAP) was born out of the recognition that regulatory compliance does not, by itself, guarantee the highest quality devices and was designed to enable device makers to measure their capability to produce high-quality devices.
This blog post provides a high-level overview of the Medical Device Discovery Appraisal Program (MDDAP) to help organizations assess the benefits of participating.
What is the Medical Device Discovery Appraisal Program (MDDAP)?
MDDAP provides the model for the Case for Quality Voluntary Improvement Program, a collaborative program between the FDA Center for Devices and Radiological Health (CDRH), the Medical Device Innovation Consortium (MDIC), Information Systems Audit and Control Association (ISACA), and the medical device industry. The Case for Quality program was initially started by the FDA in 2011 to identify manufacturers that consistently produce high-quality devices along with the practices that have the greatest impact on quality.
A timeline of MDDAP:
- 2011 – FDA launches Case for Quality
- 2018 – FDA and the Medical Device Innovation Consortium (MDIC) implement a voluntary pilot program for medical device manufacturing sites using the key business process and best practices detailed in the ISACA Capability Maturity Model Integration (CMMI) system
- 2022 – On May 5, 2022 the FDA issued the draft guidance, Fostering Medical Device Improvement: FDA Activities and Engagement with the Voluntary Improvement Program.
The draft guidance issued in May, 2022 outlines the transition from the pilot program to a permanent program, titled the Case for Quality Voluntary Improvement Program. The Voluntary Improvement Program (VIP) is facilitated through the Medical Device Innovation Consortium (MDIC) which will utilize the Capability Maturity Model Integration (CMMI) to evaluate the capability and performance of the participating medical device manufacturers. Originally developed to optimize an organization’s software development process, CMMI is now used in many industries to provide a methodology and assessment tools for continuous improvement.
The MDDAP program is voluntary and leverages the CMMI model to provide medical device manufacturers, who are already in compliance with FDA quality and regulatory requirements, with insight into how they perform against selected best practices. The program is designed to help already-compliant organizations identify gaps in existing processes and increase the ability to react to change and avoid previously unforeseen quality and process issues.
Requirements for MDDAP participation
Any facility which “designs, manufacturers, fabricates, assembles, or processes a finished device” in the United States is eligible for participation, with the following additional requirements:
- The organization must have a prior compliance history or compliance profile through an FDA inspection or MDSAP audit.
- The participating site must be registered with the FDA.
- The device must be listed with the FDA.
- The organization cannot currently be under an Official Action Indicated (OAI) or subject to judicial action.
Participants in the program can include those with Class I, II, or III devices and, in addition to being device manufacturers, may also perform contract sterilization, relabeling, remanufacturing, repacking, or specification development.
Visit the ISACA MDDAP site to see if your organization qualifies.
Advantages for manufacturers participating in MDDAP
The MDDAP program provides operational advantages by streamlining multiple regulatory processes with the FDA, as well as longer-term benefits to product quality and organizational processes. The program is built on the CMMI framework which identifies processes most effective in decreasing risk and improving product quality.
MDDAP participants who have completed appraisals through the program will have the following advantages when working with the FDA:
1. Reduced inspection activities - A risk-based approach to FDA inspections allows manufacturers to bypass routine FDA surveillance audits and PMA preapproval inspections for participating sites. The participating site will have demonstrated compliance with the quality system regulations verified by FDA through inspection (a prerequisite for joining the program). MDDAP appraisals and quarterly checkpoints evaluate the participating organization against a proven set of best practices and provide guidance on continuous improvement projects.
Participants should understand that the FDA will still perform “for cause” or directed inspections as required based on safety signals or as a follow-up to a safety event. Also, note that organizations participating in the MDSAP program will still need MDSAP audits.
2. Streamlined change notices - Participants in the MDDAP program have access to modified submission formats for:
- PMA and HDE 30-day change notices. Resources permitting, the FDA intends to review changes within the reduced timeframe of 14 calendar days.
- PMA and HDE manufacturing site change supplements.
- PMA or HDE manufacturing modules.
3. A more collaborative process with the FDA - The FDA’s Case for Quality program was designed to provide a more collaborative approach to medical device compliance and quality. This differs from the traditional oversight models by going beyond regulatory compliance and focusing on continuous improvement projects that optimize device quality.
Perhaps the biggest benefit of participating in the MDDAP program, however, is that the program provides a methodology for evaluating an organization's “maturity level” and implementing continuous improvements toward the goal of optimizing quality. Participating organizations are committing to a proven continuous improvement program. This results in the ability to consistently ensure a high-level of quality that can yield significant competitive and market advantages.
Are you looking for more tips to help your regulatory team achieve competitive advantages? Read our ebook, Regulatory strategy as a competitive advantage.




